Difference between revisions of "Antepartum Record"
Tsoutherland (talk | contribs) |
Tsoutherland (talk | contribs) |
||
| Line 748: | Line 748: | ||
|+ Antepartum H&P Social History Entries | |+ Antepartum H&P Social History Entries | ||
|- | |- | ||
| − | |Tobacco Use - Amount per day pre-pregnancy ||365981007 ||SNOMED CT ||R || ||PQ || || | + | |Tobacco Use - Amount per day pre-pregnancy ||365981007 ||SNOMED CT ||R || ||PQ ||/day || |
|- | |- | ||
| − | |Tobacco Use - Amount per day post-pregnancy || ||SNOMED CT ||R || ||PQ || || | + | |Tobacco Use - Amount per day post-pregnancy || ||SNOMED CT ||R || ||PQ ||/day || |
|- | |- | ||
|Tobacco Use - # years use || ||SNOMED CT ||R || ||PQ || || | |Tobacco Use - # years use || ||SNOMED CT ||R || ||PQ || || | ||
|- | |- | ||
| − | |Alcohol Use - Amount per day pre-pregnancy ||228273003 / 427013000 ||SNOMED CT ||R || ||PQ || || | + | |Alcohol Use - Amount per day pre-pregnancy ||228273003 / 427013000 ||SNOMED CT ||R || ||PQ ||/day || |
|- | |- | ||
| − | |Alcohol Use - Amount per day post-pregnancy || ||SNOMED CT ||R || ||PQ || || | + | |Alcohol Use - Amount per day post-pregnancy || ||SNOMED CT ||R || ||PQ ||/day || |
|- | |- | ||
|Alcohol Use - # years use || ||SNOMED CT ||R || ||PQ || || | |Alcohol Use - # years use || ||SNOMED CT ||R || ||PQ || || | ||
|- | |- | ||
| − | |Illicit/Recreational Drugs - Amount per day pre-pregnancy ||361055000 / 199254001 ||SNOMED CT ||R || ||PQ || || | + | |Illicit/Recreational Drugs - Amount per day pre-pregnancy ||361055000 / 199254001 ||SNOMED CT ||R || ||PQ ||/day || |
|- | |- | ||
| − | |Illicit/Recreational Drugs - Amount per day post-pregnancy || ||SNOMED CT ||R || ||PQ || || | + | |Illicit/Recreational Drugs - Amount per day post-pregnancy || ||SNOMED CT ||R || ||PQ ||/day || |
|- | |- | ||
|Illicit/Recreational Drugs - # years use || ||SNOMED CT ||R || ||PQ || || | |Illicit/Recreational Drugs - # years use || ||SNOMED CT ||R || ||PQ || || | ||
Revision as of 06:59, 20 May 2008
Introduction
This is a draft of the Antepartum Record Profile (AR) supplement to the PCC Technical Framework. This draft is a work in progress, not the official supplement or profile.
Profile Abstract
The Antepartum Record Profile (AR)
The Antepartum Record Profile extends the description of the content structures for the Antepartum Summary (APS), and is based on the data elements from prenatal records currently in common use. The Antepartum Record includes the following additional documents:
- Antepartum History & Physical - The initial assessment and physical
- Antepartum Laboratory - Laboratory Evaluations
- Antepartum Education - Education Record
Additional commonly used forms not included in this profile are:
- A patient generated obstetric medical history
- A postpartum form
A sample form showing the data elements may be found at: http://www.acog.org/acb-custom/aa128.pdf
This profile defines the implementation of HL7 CDA documents to represent these data elements along with the XDS, XDR and XDM bindings. This profile also defines mechanisms to group them into a single logical folder.
Glossary
The following elements are found in the Antepartum History & Physical document of the Antepartum Record:
- Abortion, Induced (AB, Induced)
- Number of induced abortions by patient. An induced abortion is a deliberate termination of pregnancy.
- Abortion Spontaneous (AB, Spontaneous)
- Number of spontaneous abortions by patient. A spontaneous abortion is a natural loss of the products of conception.
- Ectopic pregnancy
- Number of ectopic pregnancies by patient. An ectopic pregnancy is the development of a fertilized ovum outside the uterus, as in a Fallopian tube.
- Estimated Date of Delivery(EDD)/Estimated Date of Confinement(EDC)
- Date of anticipated delivery (confinement).
- Final/Corrected Estimated Date of Delivery (EDD)
- Corrected EDD/EDC based upon parameters such as ultrasound, first auscultation of fetal heart tones, etc.
- Full term
- Number of babies the mother has delivered that were between 37 and 42 completed weeks of gestation.
- Living Children
- Number of living children of patient
- Multiple births
- Number of deliveries of more than one baby by patient
- Premature
- Delivery between 20 and 36 6/7 weeks gestation
- Total Pregnancies
- Number of total pregnancies
Antepartum History & Physical - Menstrual History
- Frequency
- Specify in days the duration of the patient's monthly cycle; from first day of menses to the first day of next menses.
- hCG+
- Human Chorionic Gonadotropin pregnancy test.
- LMP (last menstrual period)
- Date measured as the first day of the patient's most recent menstrual period.
- Approximate (month known) - Patient is unsure of exact date but can offer an approximate date.
- Definite - Patient can say with certainty the date of her last menstrual period.
- Final - Finally agreed upon date of LMP.
- Unknown - Patient does not know the date of her last menstrual period.
- Menarche
- Age at onset of initial menstrual period.
- Menses Monthly
- Yes/No. Specify that the patient has or does not have a monthly period.
- Normal Amount/duration
- Yes/No. Specify whether the patient's last menstrual was typical or not in amount and duration.
- On Birth Control Pills (BCP) at conception
- Yes/No. Specify if the patient was on birth control pills at the time of conception.
- Prior Menses
- Date of patient's latest period.
Antepartum History & Physical - Past Pregnancies
- Anesthesia
- Specify the type of labor and delivery anesthesia used in previous pregnancies.
- Artificial Reproductive Technology (ART) Treatment
- List any artificial reproductive technology treatments used previously.
- Autoimmune disorder
- List any autoimmune disorders. An autoimmune disorder is a condition in which the body attacks its own tissues. (ACOG)
- Birth weight
- Specify the weight of patient's previous babies at birth.
- Date
- Month/Year of birth of patient's previous babies.
- D (Rh) sensitized
- Specify if the Rh negative mother is sensitized to the Rh D antigen. A sensitized mother produces IgG anti-D (antibody) that crosses the placenta and coats D-positive fetal red cells which are then destroyed in the fetal spleen.
- Gestational Age weeks
- Specify gestational age in weeks at delivery of patient's previous pregnancies.
- Infertility
- Specify history of infertility. Infertility primarily refers to the biological inability of a man or a woman to contribute to conception. Infertility may also refer to the state of a woman who is unable to carry a pregnancy to full term.
- Kidney disease/Urinary Tract Infection (UTI)
- List any kidney disease or urinary tract infections. Kidney disease is either a declining or a sudden loss in renal function. A urinary tract infection (UTI) is a bacterial infection that affects any part of the urinary tract.
- Length of labor
- Specify the number of hours patient was in labor for previous pregnancies.
- Place of Delivery
- Specify the location patient delivered for previous pregnancies. (Hospital name, city and state if known)
- Preterm labor
- Yes/No. Specify if the patient had preterm labor with previous pregnancies
- Pulmonary (TB, Asthma)
- Specify if patient has a history of asthma, TB or other pulmonary problems.
- Sex M/F
- Specify sex of patient's previously delivered babies.
- Type Delivery
- Specify type of delivery for previous pregnancies: Vaginal (spontaneous, forceps, vacuum), Cesarean section (low-transverse, classical, low-vertical).
- Uterine Anomaly/DES
- – Specify if the patient has any uterine structural abnormalities or exposure to diethylstilbesterol.
- Varicosities/Phlebitis
- Specify if patient has a history of swelling or inflammation of her veins.
Antepartum History & Physical - Other elements:
- Abdomen
- Area of the body that lies between the chest and the pelvis and encloses the stomach, intestines, liver, spleen and pancreas
- Adnexa
- Appendages of the uterus which include the fallopian tubes, the ovaries and the supporting ligaments of the uterus.
- BMI
- Body Mass Index. Measurement of the relative percentages of fat and muscle mass in the human body.
- BP
- Pressure exerted by the blood against the walls of the arteries, maintained by the contraction of the left ventricle, the resistance of the arterioles and capillaries, the elasticity of the arterial walls, and by the viscosity and volume of the blood.
- Breasts
- In humans, one of the paired regions in the anterior portion of the thorax. The breasts consists of mammary glands, the skin, the muscles, the adipose tissue and connective tissues.
- Cervix
- The lower, narrow end of the uterus, which protrudes into the vagina. (ACOG)
- Diagonal Conjugate
- The distance from the promontory of the sacrum to the lower margin of the pubic symphysis
- Extremities
- A bodily limb or appendage.
- Fundi
- Concave, interior of the eye, consisting of the retina, the choroid, the sclera, the optic disk, and blood vessels, seen by means of the opthalmoscope.
- Gynecoid pelvic type
- The normal female pelvis.
- Heart
- The hollow, muscular organ that maintains the circulation of the blood.
- HEENT
- Head, Eyes, Ears, Nose and Throat
- Height
- Measurement of stature
- Lungs
- Either of the pair of organs occupying the cavity of the thorax that effect the aeration of the blood.
- Lymph nodes
- Any of the accumulations of lymphoid tissue organized as definite lymphoid organs varying from 1 to 25 mm in diameter situated along the course of lymphatic vessels and consisting of an outer cortical and inner medullary part.
- Rectum
- The distal segment of the large intestine, between the sigmoid colon and the anal canal.
- Sacrum
- Triangular bone below the lumbar vertebrae.
- Skin
- Outer protective covering of the body
- Spines
- (Ischial Spines) Two parts of the maternal pelvis resulting from the bony processes projecting backward and medially from the posterior border of the ischium.
- Subpubic arch
- Arch formed by the conjoined rami of the ischia and pubic bones of the two sides of the body.
- Teeth
- one of the hard, calcified structures set in the alveloar processes of the jaws for the biting and mastication of food.
- Thyroid
- The thyroid gland. One of the largest endocrine glands in the body. This gland is found in the neck below the thyroid cartilage and at approximately the same level as the cricoid cartilage. The thyroid controls how quickly the body burns energy, makes proteins, and how sensitive the body should be to other hormones.
- Uterus size
- In pregnancy the uterine size is estimated in terms of weeks of gestation. e.g 12 weeks if the fundus reaches the top of the smphysis pubis or 20 weeks' gestation when the fundus reaches the umbilicus.
- Vagina
- The genital canal in the female, leading from the opening of the vulva to the cervix of the uterus.
- Vulva
- The external genital organs of the female, including the labia majora, labia minora, clitoris, and vestibule of the vagina.
- Patient Weight
- A measurement of mass.
The following terms are found in the Antepartum Laboratory document of the Antepartum Record:
- 1st Trimester Aneuploidy risk assessment
- Non-invasive screening for chromosomal abnormalities, such as Down syndrome, performed in the first trimester. Screening tests that uses a combination of fetal measurements (crown rump length and nuchal translucency) and maternal blood tests for beta-human chorionic gonadotropin (hCG) and pregnancy associated plasma protein (PAPP-A) to determine risk for trisomy 21, trisomy 13 and trisomy 18.
- 2nd Trimester serum screening
- Non-invasive screening test for chromosomal abnormalities, such as Down yndrome, trisomy 18, or open neural defects. Blood test to measure alpha-fetoprotein (AFP), estriol, human chorionic gonadotropin (hCG) [free or total], and inhibin-A.
- Amnio/CVS
- Amniocentesis: Percutaneous transabdominal puncture of the uterus during pregnancy to obtain amniotic fluid. It is commonly used for fetal karotype determination in order to diagnose abnormal fetal conditions. Chorionic Villus Sampling (CVS): A method of diagnosis of fetal diseases by sampling the cells of the placental chorionic villi for DNA analysis, presence of bacteria, concentration of metabolites, etc.
- Amniotic Fluid (AFP)
- Test to detect the presence of Alpha-fetoprotein in vaginal secretions and amniotic fluid. Test to indicate several birth defects. Usually performed at gestation week 16.
- Antibody screen
- Anti-D Immune Globulin (RHIG)
- Blood type
- Test to determine blood group, i.e. A, B, AB or O
- Chlamydia
- Test done to detect the most common sexually transmitted disease caused by the bacterium, Chlamydia trachomatis.
- Cystic Fibrosis
- Test to detect the abnormal gene that causes cystic fibrosis. Usually performed before 20 weeks gestation.
- D (Rh) Antibody screen
- Screening test for presence of IgG antibodies.
- D (Rh) type
- Test to type red blood surface antigen.
- Diabetes screen
- Laboratory screen to determine blood glucose levels.
- Familial Dysautonomia
- Autosomal disorder of the peripheral and autonomic nervous systems limited to individuals of Ashkenazic Jewish descent; clinical manifestations are present at birth and include diminished lacrimation, defective thermoregulation, orthostatic hypotension, fixed pupils, excessive sweating, loss of pain and temperature sensation, and absent reflexes; pathologic features include reduced numbers of small diameter peripheral nerve fibers and autonomic ganglion neurons.
- Genetic Screening Test
- Screening for genetic disorders based on racial or ethnic background, i.e. sickle cell, Thalassemia, Tay-Sachs, Canavan, Cystic fibrosis. Also other genetic disorders based on familial history, i.e. fragile X syndrome, Duchenne’s muscular dystrophy.
- Gonorrhea
- Test for Neisserai gonorrheae
- Group B Strep
- Culture test of rectovaginal swabs at 35 – 37 weeks gestation to determne Group B colonization in the pregnant woman.
- GTT (if screen abnormal)
- Glucose Tolerance Test. Used to determine how quickly the body metabolizes blood sugar. Test to screen for gestational diabetes mellitus between 24 and 28 weeks.
- HBsAg
- Test for the surface antigen of the Hepatitis-B virus
- HCT/HGB/MCV
- HCT- Hematocrit – blood test measuring percentage of red blood cells found in a given volume of whole blood.
- HGB- Hemoglobin – blood test measuring the level of the protein carrying oxygen in red blood cells.
- MCV - Mean corpuscular volume - average volume of red blood cells calculated from the hematocrit red blood cell count
- Hemoglobin Electrophoresis
- Blood test done to measure the types of hemoglobin. The test can detect abnormal levels of hemoglobin such as that found in sickle cell anemia.
- HIV
- Human immunodeficiency virus antibody testing.
- HIV Counseling/Testing
- Discussion with pregnant patient regarding Human Immunodeficiency Virus HIV status, risks and prevention strategies. Blood test to determine HIV status.
- Karotype
- Test done on cells/tissue to identify and evaluate chromosomes.
- MSAFP/Multiple markers
- Screening blood test on the mother for Maternal Serum Alphafetoprotein. This test is offered to pregnant woman between 15 and 20 weeks gestation. Test screens for neural tube defects.
- Pap test
- Cervical cytology test to determine abnormal cells of the cervix.
- PPD
- - Mantoux test with purified protein derivative for tuberculosis.
- Rubella
- Determination of level of immunity to the rubella virus (German measles).
- Tay-Sachs
- Test done to detect enzyme responsible for causing Tay Sachs disease.
- Ultrasound
- Assessment of gestational age, size and growth of a fetus.
- Urine Culture/Screen
- Test for bacteria, sugar and/or protein in urine.
- Varicella
- Blood test to screen for varicella antibodies. A pregnant patient is at increased risk for chicken pox if testing shows no antibodies,
- VDRL
- A blood test to screen for syphillis antibodies.
The following terms are found in the Antepartum Education document of the Antepartum Record:
First Trimester
- Alcohol
- Discussion with patient about past and present use of alcohol and the perinatal implications of continued use during pregnancy; referral to treatment program if appropriate.
- Anticipated Course of prenatal care
- Discussion with the patient on the scope of care that will be performed in the office, lab work that may be performed, signs and symptoms that should be reported, anticipated schedule of visits, physician coverage of labor and delivery.
- Childbirth classes/hospital facilities
- Discussion with the patient on educational programs available for childbirth and hospital choice.
- Domestic violence
- Screening/Discussion with patient regarding physical threats/abuse/safety concerns; referral to appropriate counseling, legal and/or social advocacy program if appropriate.
- Environmental/Work hazards
- Discussion with patient about potential exposures to environmental agents at work, home, or locations that may affect pregnancy.
- Exercise
- Discussion with patient on appropriate level of exercise activities during the pregnancy.
- Illicit/Recreational drugs
- Discussion with patient about past and present use of illicit or recreational drugs and the perinatal implications of continued use during pregnancy; referral to treatment program if appropriate.
- Indications for ultrasounds
- Discussion with patient regarding reasons ultrasound test will be performed during pregnancy.
- Influenza vaccine
- Discussion with patient of risks/benefits of influenza and influenza vaccine.
- Nutrition and weight gain counseling, special diet
- Information about balanced nutrition, ideal caloric intake and weight gain.
- Risk factors identified by prenatal history
- Seatbelt use
- Discussion with patient on use of seatbelts.
- Sexual activity
- Discussion with the patient of sexual activity: concerns, restrictions, warning signs and/or safe sex practices.
- Smoking counseling
- Discussion with patient regarding smoking cessation and smoke exposure.
- Tobacco (Ask,advise,assess,assist,and arrange)
- status; Advise patient to stop smoking; Assess patient's willingness to attempt to quit smoking; Assist patients who are interested in quitting by providing pregnancy specific cessation materials; Arrange follow up visits to track progress.
- Toxoplasmosis precautions
- Discussion with patient of risk factors for toxoplasmosis and precautions for avoiding/preventing infection.
- Travel
- Discussion with patient on travel precautions, if any.
- Use of any medications (including supplements, vitamins, herbs or OTC drugs)
- Discussion with patient of risks/benefits/safety of any medications currently used by patient.
Second Trimester
- Abnormal lab values
- Discussion with patient of lab results that fall outside normal range and that may require further testing.
- Domestic violence
- Screening/Discussion with patient regarding physical threats/abuse/safety concerns; referral to appropriate counseling, legal and/or social advocacy program if appropriate.
- Influenza vaccine
- Discussion with patient of risks/benefits of influenza and influenza vaccine.
- Postpartum family planning/tubal sterilization
- Discussion with patient of intended postpartum contraception options, including tubal sterilization.
- Selecting a newborn care provider
- Discussion with patient to identify newborn care provider; referral to resources to help patient choose provider if none previously identified.
- Signs and symptoms of preterm labor
- Discussion with patient on risks, signs and symptoms of preterm labor.
- Smoking counseling
- Discussion with patient regarding smoking cessation and smoke exposure.
Third Trimester
- Anesthesia/Analgesia plans
- Discussion with patient to determine intended method of pain management/discomfort during labor and delivery.
- Breast or bottle feeding
- Discussion with patient of nutritional advantages/disadvantages of human breast milk, bottled formula; advise on available lactation consultation services.
- Circumcision
- Discussion with patient on circumcision of male newborn.
- Domestic violence
- Screening/Discussion with patient regarding physical threats/abuse/safety concerns; referral to appropriate counseling, legal and/or social advocacy program if appropriate.
- Family medical leave or disability forms
- Fetal Movement monitoring
- Discussion with patient regarding her perception and assessment of fetal movement.
- Influenza vaccine
- Discussion with patient of risks/benefits of influenza and influenza vaccine.
- Labor signs
- Discussion with patient on signs of labor, i.e. contractions, membrane rupture, bleeding, etc.
- Newborn education (Newborn screening, jaundice, SIDS, car seat)
- Prenatal discussion with patient of preventive public health screening procedures available to newborns; testing that will occur on baby after birth to screen for up to 30 disorders.
- Postpartum depression
- Discussion with patient of signs of postpartum depression.
- Postterm counseling
- Discussion with patient of risks of pregnancy extending beyond 42 weeks.
- Signs & Symptoms of Pregnancy-induced hypertension
- Discussion with patient of signs and symptoms of hypertension.
- Smoking counseling
- Discussion with patient regarding smoking cessation and smoke exposure.
- VBAC counseling
- Discussion with patient of risks/benefits of vaginal birth after previous cesarean surgery.
- History and physical have been sent to hospital
- Notation of date and initials of person transmitting history and physical to hospital prior to delivery.
- Tubal sterilization consent signed
- Notation of date the consent form for tubal sterilization signed and the initials of person witnessing.
Issue Log
Open Issues
- Issue
- Issue
Closed Issues
Volume I
Add the following bullet to the list of profiles
- Antepartum Record - A folder of content profiles that contains the summarization record or the antepartum care delivery including initial patient history and physical, ambulatory checks of mother and fetus, laboratory studies, and patient education.
Dependencies
Add the following row(s) to the list of dependencies
| Integration Profile | Dependency | Dependency Type | Purpose |
|---|---|---|---|
| Antepartum Record A&B | IHE History and Physical | Child | Initial Intake and Assessment for antepartum care |
| Antepartum Summary Form C&F&G | Medical Summary | Child | Update and Progress Note |
| Antepartum Summary Form D | XD-Lab | Child | Obstetric Lab Evaluation |
| Antepartum Summary Form E | Obstetric Education Form |
Profile Name
The Antepartum Record Profile (AR)
There are over 4 million births in the United States each year, including more than 1 million cesarean sections and more than 300,000 preterm or low birth weight babies. Obstetric patients in labor and admitted to Labor and Delivery must have a complete summary of their antepartum ambulatory care available at the time of admission to evaluate and / or ameliorate risk. This same data is required at any visit to Labor and Delivery for any other problems or special needs a patient may require. The antepartum record must be available in its entirety for appropriate care and legal concerns.
Practitioners who would use the aggregated record include: obstetricians, perinatologists, certified nurse midwives, family practice physicians, pediatricians, labor and delivery staff, emergency department staff, anesthesiologists, hospitalists, social workers, other medical specialists and patients.
During the 40 weeks of a typical pregnancy duration, the patient will have an initial History and Physical Examination, followed by repetitive office visits with multiple laboratory studies, imaging (usually ultrasound) studies, and serial physical examinations with recordings of vital signs, fundal height, and the fetal heart rate. As the patient is seen over a finite period in the office, aggregation of specific relevant data important to the evaluation of the obstetric patient upon presentation to Labor and Delivery is captured on paper forms. The antepartum record contains the most critical information needed including the ongoing Medical Diagnoses, the Estimated Due Date, outcomes of any prior pregnancies, serial visit data on the appropriate growth of the uterus and assessments of fetal well being, authorizations, laboratory and imaging studies. This data must all be presented and evaluated upon entry to the Labor and Delivery Suite to ensure optimal care for the patient and the fetus.
Although the patient and her care provider may plan for a vaginal (natural) method of delivery, there is a substantive chance the delivery route may be surgical, requiring anesthesia and post-surgical care.
Current practice is to copy the patient's (paper) chart at various times during the pregnancy (as at 28 weeks and at 36 weeks of completed gestation), and transport the copies of the chart to the hospital the patient intends to use for delivery. Should the patient arrive prior to the chart copy arriving, or if the chart (or information within the chart) is missing on presentation of the patient to Labor and Delivery (a frequent occurrence), the staff or clinicians repeat laboratory or imaging studies. This results in unwarranted and duplicative tests, is wasteful of time and resources, and leads to dissatisfied patients. Further, missing or incomplete information about the patient’s clinical status may create a situation where critical information is unavailable to clinicians, which may ultimately result in an injury, inadequate aftercare or other undesirable outcome.
Significantly, a large portion of patients arrive in L&D without complete documentation. In one recent U.S. study , ~70% of patients (with paper charts) arrived in L&D without their current medical record being available. While only one hospital was involved in this study, one can see the extent of the issue, with pregnant patients possibly going to a different hospital than planned (preterm labor, rapid labor and unable to make it to the planned delivery hospital, or visiting a distant city), moving mid-care, or with a covering physician (rather than the primary obstetrician) on call.
In a Swedish study done in the 1990’s, critical data on paper records were incomplete from 45 to 87.5% of the time. Thus, availability of current medical records remains a significant problem for most hospital Labor and Delivery units; availability of key information electronically will significantly enhance patient safety.
Use Cases
Use Case 1: Basic Antepartum Record Summary Use Case
Pre-condition
The patient’s obstetrician sees the patient for her initial and subsequent prenatal visits. During the initial and/or subsequent prenatal visits information is collected and may be updated within the office Electronic Health Record (EHR), these include:
- Patient demographics
- Menstrual history
- Obstetric history
- Medical history including surgical history, psych-social history
- Genetic history and screening/Teratology counseling
- Infection history
- Family history
- Initial and subsequent physical examination
- Medications
- Problems and risk factors for preterm birth
- Allergies
- Prenatal visit information
- Prenatal Laboratory results
- Patient education information and plans for delivery if known
The information collected during the patient’s prenatal visits is the components which are included in the patient’s Antepartum Record Summary.
Event(s)
Scenario 1 - At a specified time an initial and/or subsequent patient Antepartum Record Summary is transmitted by the patient’s obstetrician EHR to the intended facility for delivery.
The intended facility of delivery health information system receives the transmitted initial and/or subsequent patient Antepartum Record Summary.
Scenario 2 - At a specified time the initial and/or subsequent patient Antepartum Record Summary registry information is transmitted by the patient’s obstetrician EHR to a registry.
The facility of delivery health information system queries the registry repository for the applicable patient’s Antepartum Record Summary(s). A request is made for the patient’s Antepartum Record Summary. The applicable system which contains the patient’s Antepartum Record Summary then makes available the patients Antepartum Record Summary information to the requesting facility of delivery.
Post-condition
The received patient Antepartum Record Summary can be viewed and/or imported into the facility for delivery health information system to facilitate patient care by healthcare professional at the time of delivery for the mother and newborn.
Use Case 2: Antepartum Care Delivery
Pre-condition
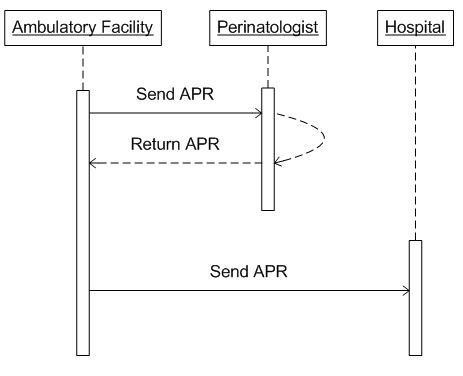
The patient’s obstetrician sees the patient for her pregnancy in the ambulatory (office) setting. During the pregnancy, the patient is noted to have a medical problem requiring consultation with a Maternal-Fetal Medicine specialist (perinatologist). The office obtains pre-authorization from the insurance payer for the consult, and for the intended or anticipated route of delivery, and transmits that information to both the consultant and to the hospital.
Events
The patient is seen in the obstetrician’s office where a complete medical and relevant social history are taken by the nurse and recorded in the office EHR, incorporating data from the perinatologist’s consultation report as appropriate. Laboratory and imaging reports ordered by the perinatologist as well as the perinatologist’s consultation report are displayed electronically to the obstetrician. The obstetrician reviews the consultation report from the perinatologist’s office and imaging studies ordered by the perinatologist along with data recorded by the nurse. Physical exam reveals some abnormalities. The obstetrician orders additional laboratory studies, and sends the patient to the hospital to Labor and Delivery.
When the laboratory results return, the physician completes the admission H&P, Allergies, Medications, includes the data prepared or ordered by the perinatologist, and makes it available to L&D. This data includes an assessment of the patient’s health status, and the requisite data summarized from the antepartum care given. The charge nurse for L&D documents that the complete collection of documents needed is available. The Post-Partum discharge planning is notified and assures that there is a suitable environment with appropriate support for post-delivery after-care.
Post-condition
The Pre-delivery H&P and Antepartum Summary with appropriate relationships to the Perinatologist Consultation, and all the antepartum laboratory and imaging studies are available to the obstetrician and the birthing center personnel for incorporation into their respective EHRs. The H&P is also available to the patient for viewing and incorporation into the patient’s PHR, and into the newborn baby’s PHR. For the APS profile, summary content is available to the obstetrician, with a plan for full content to be added in future years through other content profiles that share this use case.
Use Case Name 3
A pregnant diabetic patient is seen by her obstetrician in the office for a prenatal care. An ultrasound is performed to determine gestational age. The patient is sent for perinatology consult as a high-risk patient. Her obstetrician transmits preauthorization insurance information, labs and anticipated route of delivery to perinatologist and hospital.
The patient returns to her perinatologist biweekly for blood testing and ultrasounds when necessary in addition to regular ob visits. The perinatologist reports back to the obstetrician after each visit. Complete History and Physical, imaging and additional labs are performed during patient’s regular visit with her obstetrician.
The patient arrives at labor and delivery at the hospital. Obstetrician completes the admission H&P, Allergies, Medications, and includes the data prepared or ordered by the perinatologist, and makes it available to L&D. This data includes an assessment of the patient’s health status, and the requisite data summarized from the antepartum care given. The charge nurse for L&D documents that the complete collection of documents needed is available.
The patient’s obstetrician delivers by Cesarean Section after anesthesia. The post-partum discharge planning is notified and assures that there is a suitable environment with appropriate support for post-delivery after-care. Delivery information, i.e. birth weight, APGAR scores, type of delivery, etc is available for pediatrician. The patient can then incorporate H&P into her own and her newborn’s PHR.
Actors/Transaction
There are two actors in this profile, the Content Creator and the Content Consumer. Content is created by a Content Creator and is to be consumed by a Content Consumer. The sharing or transmission of content from one actor to the other is addressed by the appropriate use of IHE profiles described below, and is out of scope of this profile. A Document Source or a Portable Media Creator may embody the Content Creator Actor. A Document Consumer, a Document Recipient or a Portable Media Importer may embody the Content Consumer Actor. The sharing or transmission of content or updates from one actor to the other is addressed by the use of appropriate IHE profiles described by section 3.7 Content Bindings with XDS, XDM and XDR found in the Patient Care Coordination Technical Framework
Options
| Actor | Option | Section |
|---|---|---|
| Content Consumer | View Option (1) Document Import Option (1) |
PCC TF-1: 2.13.1 PCC TF-1: 2.13.2 |
| Content Creator | Referral Option (1) Discharge Summary Option (1) |
PCC TF-1: 2.13.5 PCC TF-1: 2.13.6 |
Note 1: The Actor shall support at least one of these options.
Grouping
Content Bindings with XDS, XDM and XDR
It is expected that the transfers of care will occur in an environment where the physician offices and hospitals have a coordinated infrastructure that serves the information sharing needs of this community of care. Several mechanisms are supported by IHE profiles:
- A registry/repository-based infrastructure is defined by the IHE Cross Enterprise Document Sharing (XDS) and other IHE Integration Profiles such as patient identification (PIX & PDQ), and notification of availability of documents (NAV).
- A media-based infrastructure is defined by the IHE Cross Enterprise Document Media Interchange (XDM) profile.
- A reliable messaging-based infrastructure is defined by the IHE Cross Enterprise Document Reliable Interchange (XDR) profile.
- All of these infrastructures support Security and privacy through the use of the Consistent Time (CT) and Audit Trail and Node Authentication (ATNA) profiles.
For more details on these profiles, see the IHE IT Infrastructure Technical Framework.
Content profiles may impose additional requirements on the transactions used when grouped with actors from other IHE Profiles.
Cross Enterprise Document Sharing, Media Interchange and Reliable Messages
Actors from the ITI XDS, XDM and XDR profiles embody the Content Creator and Content Consumer sharing function of this profile. A Content Creator or Content Consumer must be grouped with appropriate actors from the XDS, XDM or XDR profiles, and the metadata sent in the document sharing or interchange messages has specific relationships to the content of the clinical document described in the content profile.
Notification of Document Availability (NAV)
A Document Source should provide the capability to issue a Send Notification Transaction per the ITI Notification of Document Availability (NAV) Integration Profile in order to notify one or more Document Consumer(s) of the availability of one or more documents for retrieval. One of the Acknowledgement Request options may be used to request from a Document Consumer that an acknowledgement should be returned when it has received and processed the notification. A Document Consumer should provide the capability to receive a Receive Notification Transaction per the NAV Integration Profile in order to be notified by Document Sources of the availability of one or more documents for retrieval. The Send Acknowledgement option may be used to issue a Send Acknowledgement to a Document Source that the notification was received and processed.
Document Digital Signature (DSG)
When a Content Creator Actor needs to digitally sign a document in a submission set, it may support the Digital Signature (DSG) Content Profile as a Document Source. When a Content Consumer Actor needs to verify a Digital Signature, it may retrieve the digital signature document and may perform the verification against the signed document content.
Content Modules
Content modules describe the content of a payload found in an IHE transaction. Content profiles are transaction neutral. They do not have dependencies upon the transaction that they appear in.
Content Module 1
Process Flow
More text about process flow
Actor Definitions
Actors are information systems or components of information systems that produce, manage, or act on information associated with operational activities in the enterprise.
- Content Creator
- The Content Creator Actor is responsible for the creation of content and transmission to a Content Consumer.
- Content Consumer
- A Content Consumer Actor is responsible for viewing, import, or other processing of content created by a Content Creator Actor.
Transaction Definitions
Transactions are interactions between actors that transfer the required information through standards-based messages.
- Transaction
- Definition
Volume II
General to do items for face-to-face 5/19-5/23
- Review proposed document structures (APH&P, APL, APE)
- Determine where to use SHALL, SHOULD and MAY
- Review/discuss selection of SNOMED CT codes (Christine Spisla is available from 4-4:30pm on Monday and 12pm-till on Tuesday)
Antepartum Record Content
Consists of the following documents:
- Antepartum History and Physical (Forms A&B)
- Antepartum Summary (Forms C&F)
- Antepartum Laboratory (Form D)
- Antepartum Education (Form E)
Standards
- CDAR2
- Clinical Document Architecture, Release 2, 2005 HL7
- CRS
- Implementation Guide for CDA Release 2 – Level 1 and 2 – Care Record Summary (US realm), 2006, HL7.
- CCD
- ASTM/HL7 Continuity of Care Document (Draft)
Antepartum History and Physical (APH&P)
The Antepartum History and Physical inherits all constraints from the IHE History and Physical and also requires the following additional constraints.
Data Element Index
| Data Element | CDA Section | Comments |
|---|---|---|
| Header data | Need to include Language, Ethnicity, Husband/Domestic Partner, Father of Baby; needs further analysis | |
| Chief Complaint | Chief Complaint | |
| Pregnancy History (Form A) | Pregnancy History | Summary (Gravida Para Abortus) and detailed history of pregnancies |
| Menstrual/Gynecological History (Form A) | Resolved Problems(PMH) | |
| Medical History (Form A) | Resolved Problems (PMH) | Exclude social and family history (included in other sections) |
| Medical History - Tobacco, Alcohol, Drugs (Form A) | Social History | |
| Medical History - Relevant Family History (Form A) | Family History | |
| Medications | Medications | |
| Allergies | Allergies and Other Adverse Reactions Section | |
| Symptoms Since LMP (Form B) | History of Present Illness | |
| Genetic Screening/Teratology Counseling (Form B) | Review of Systems | |
| Infection History (Form B) | Review of Systems | |
| Initial Physical Examination (Form B) | Physical Examination | |
| Vital Signs (Form B) | Vital Signs | |
| Diagnostic Findings | this section is required by CDA4CDT H&P - The intention for APR is to have the antepartum specific labs in the APL document. However, lab data may be put here as well. | |
| Assessment and Plans | this section is required by CDA4CDT H&P - The intention for APR is to have the antepartum specific education in the APE document. However, education data may be put here as well. |
Document Specification
| Data Element | Opt | Template ID | Comments |
|---|---|---|---|
| Header This section is the same as it is for history and physical, however it SHALL also include coded participant elements for husband/domestic partner and father of baby. Ethnicity for the patient SHOULD also be included. The coding system SHALL be SNOMED CT for all three entries. For husband the code SHALL be 127849001. For domestic partner the code SHALL be 414043009. For father of baby the code SHALL be 9947008. For ethnicity the code SHALL be 397731000. |
R | See below this table for more details | |
| Chief Complaint |
R | 1.3.6.1.4.1.19376.1.5.3.1.1.13.2.1 | |
| History of Present Illness This section will be the same as it is for History & Physical and SHOULD contain clinical statements about patient reported symptoms since the last menstrual period. |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.4 | |
| Resolved Problems This section is the same as it is for History & Physical and represents the patient's past medical history and gynecological history. These entries SHOULD use the codes specified in the appropriate Antepartum Resolved Problems Entries tables and SHALL be grouped into organizers with classCode='CLUSTER' |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.8 | |
| Pregnancy History This section will consist of two entries, both of which will live under the existing Pregnancy History section. Pregnancy Summary History: Required; will use the existing observation Pregnancy Observation and add SNOMED codes for additional fields. Pregnancy Detail History: Optional; will contain the details of each pregnancy as list in the table below. |
R | 1.3.6.1.4.1.19376.1.5.3.1.1.5.3.4 | Fields that don't exist in the current Pregnancy Observation list: Summary - ectopics, multiple births Details - length of labor, birth weight, sex, type of delivery, anesthestics, place of delivery, preterm labor |
| Social History This section is the same as it is for History & Physical, however it SHALL contain coded entries as specified in the Antepartum Social History table. |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.16 | |
| Family History This section is the same as it is for History & Physical, however it SHALL contain the coded entry as specified in the Antepartum Family History table. |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.14 | |
| Review of Systems This section is the same as it is for History & Physical, however it SHALL include coded entries for genetic screening and infection history. These entries SHOULD use the codes specified in the appropriate Antepartum Review of Systems tables and SHALL be grouped into organizers with classCode='CLUSTER'. The code system for genetic screening SHALL be LOINC and the code SHALL be 19102-3. |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.18 |
- use organizers to group genetic screening and infection history? this should be same structure as Resolved Problems (PMH) |
| Physical Examination This section is the same as it is for History & Physical, however it SHALL include coded entries for physical examinations related to antepartum care. These required entries SHOULD use the codes from the Anterpartum Physical Examination table. |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.24 | |
| Vital Signs This section is the same as it is for History & Physical, however it SHALL include coded entries for vital signs related to antepartum care. These required entries SHOULD use the codes from the Anterpartum Vital Signs table. |
R | 1.3.6.1.4.1.19376.1.5.3.1.3.25 |
Antepartum Header - Details
| Data Element | Example |
|---|---|
| Husband/Domestic Partner This element SHALL be included as a participant in the header of the CDA document in the event of the pregnancy. If this does not apply to the patient this element SHALL use a null flavor. |
<!-- Husband/Domestic Partner -->
<participant typeCode="IND"> <!-- what is IND? -->
<associatedEntity classCode="NOK"> <!-- what is NOK? -->
<code code="184142008" displayName="patient's next of kin"
codeSystem="2.16.840.1.113883.6.96" codeSystemName="SNOMED CT"/>
<addr>
<streetAddressLine>45 Chunn Dr.</streetAddressLine>
<city>Spring Hill</city>
<state>TN</state>
<postalCode>37174</postalCode>
<country>USA</country>
</addr>
<telecom value="tel:(999)555-1212" use="WP"/>
<associatedPerson>
<name>
<prefix>Mr.</prefix>
<given>John</given>
<family>Youngston</family>
</name>
</associatedPerson>
</associatedEntity>
</participant>
|
| Father of Baby This element SHALL be included as a participant in the header of the CDA document in the event of the pregnancy. If the father of the baby is unknown this element SHALL use a null flavor. |
<!-- Father of baby -->
<participant typeCode="IND"> <!-- what is IND? -->
<associatedEntity classCode="NOK"> <!-- what is NOK? -->
<code code="9947008" displayName="natural father"
codeSystem="2.16.840.1.113883.6.96" codeSystemName="SNOMED CT"/>
<addr>
<streetAddressLine>18 Oak Valley Dr.</streetAddressLine>
<city>Monteagle</city>
<state>TN</state>
<postalCode>37205</postalCode>
<country>USA</country>
</addr>
<telecom value="tel:(999)555-1212" use="WP"/>
<associatedPerson>
<name>
<prefix>Mr.</prefix>
<given>Thomas</given>
<family>Caster</family>
</name>
</associatedPerson>
</associatedEntity>
</participant>
|
| Ethnicity This element SHOULD be included in recordTarget/patientRole/patient/ethnicGroupCode in the header of the CDA document. This information can be relevant to the course of care provided to the patient. |
<recordTarget>
<patientRole classCode="PAT">
<id root="27143B24-E580-4F47-9405-3D0DC2BF1223" extension="1022"/>
<addr>
<streetAddressLine/>
<city/>
<state>FM</state>
<postalCode/>
<country>Canada</country>
</addr>
<telecom nullFlavor="UNK" use="HP"/>
<patient classCode="PSN" determinerCode="INSTANCE">
<name>
<prefix/>
<given>Christine</given>
<family>Smith</family>
<suffix/>
</name>
<ethnicGroupCode code="364699009" displayName="ethnic group"
codeSystem="2.16.840.1.113883.6.96" codeSystemName="SNOMED CT"/>
<administrativeGenderCode code="F" codeSystem="2.16.840.1.113883.5.1"/>
<birthTime value="20040725"/>
</patient>
<providerOrganization classCode="ORG" determinerCode="INSTANCE">
<id root="2.16.840.1.113883.19.5"/>
</providerOrganization>
</patientRole>
</recordTarget>
|
Antepartum H&P Resolved Problems Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Date of Last Menstrual Period | 21840007 | SNOMED CT | R | TS | |||
| Menses Monthly | SNOMED CT | R | BL | ||||
| Prior Menses Date | 84292000 | SNOMED CT | R | TS | |||
| Duration of Menstrual Flow | 161720007 | SNOMED CT | R | Frequency | PQ | days | |
| Oral Contraceptive Preparation | 59261009 | SNOMED CT | R | on BCP at conception | BL | ||
| Menarche | 20016009 | SNOMED CT | R | PQ | |||
| hCG+ | SNOMED CT | R | several codes | TS |
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Diabetes | 161445009 / 266991009 | SNOMED CT | R | diabetes mellitus / metabolic disorder? | BL | ||
| Hypertension | 161501007 | SNOMED CT | R | BL | |||
| Heart Disease | 275544003 | SNOMED CT | R | BL | |||
| Autoimmune Disorder | SNOMED CT | R | BL | ||||
| Kidney Disease | 275552000 | SNOMED CT | R | BL | |||
| UTI | 267002001 | SNOMED CT | R | BL | |||
| Neurologic/Epilepsy | 161480008 | SNOMED CT | R | BL | |||
| Psychiatric | 161464003 | SNOMED CT | R | BL | |||
| Depression/Postpartum Depression | 161469008 | SNOMED CT | R | BL | |||
| Hepatitis/Liver Disease | 161535005 | SNOMED CT | R | BL | |||
| Varicosities/Phlebitis | 413154005 | SNOMED CT | R | BL | |||
| Thyroid Dysfunction | 275536003 | SNOMED CT | R | BL | |||
| Trauma/Violence | 161472001 | SNOMED CT | R | BL | |||
| History of Blood Transfusion | 161664006 | SNOMED CT | R | BL | |||
| D(Rh) Sensitized | SNOMED CT | R | BL | ||||
| Pulmonary | 161523006 | SNOMED CT | R | BL | |||
| Seasonal Allergies | 161524000 | SNOMED CT | R | BL | |||
| Drug/Latex Allergy/Reactions | 161611007 | SNOMED CT | R | BL | |||
| Breast | 429087003 | SNOMED CT | R | H/O malignant neoplasm of breast? | BL | ||
| Gyn Surgery | SNOMED CT | R | Complex Type | ||||
| Operations/Hospitalizations | 161615003 | SNOMED CT | R | Complex Type | |||
| Anesthetic Complications | 161593001 | SNOMED CT | R | BL | |||
| History of Abnormal Pap | 271902005 | SNOMED CT | R | H/O gynecological disorder? | BL | ||
| Uterine Anomaly/DES | 267016006 | SNOMED CT | R | H/O abnormal uterine bleeding? | BL | ||
| Infertility | 169589005 | SNOMED CT | R | BL | |||
| Art Treatment | SNOMED CT | R | BL |
Antepartum H&P Pregnancy History Entries
| Description | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Summary over All Pregnancies | |||||||
| Gravida (Number of Total Pregnancies) | 161732006 | SNOMED CT | R | PQ | |||
| Number of Full Term Deliveries | 267015005 | SNOMED CT | R | PQ | |||
| Number of Premature Deliveries | 161765003 | SNOMED CT | R | PQ | |||
| Number of Abortion, Induced | 252114001 | SNOMED CT | R | PQ | |||
| Number of Abortion, Spontaneous (Miscarriages) | 248989003 | SNOMED CT | R | PQ | |||
| Number of Ectopic Pregnancies | 29717002 | SNOMED CT | R | PQ | |||
| Number of Multiple Births | 364323006 | SNOMED CT | R | PQ | |||
| Number of Living Children | 364325004 | SNOMED CT | R | PQ | |||
| Number of Live Births | SNOMED CT | R | PQ | ||||
| Detailed Pregnancy Data | |||||||
| Date Month/Year | SNOMED CT | R | TS | ||||
| Weeks Gestation at Delivery | 268477000 | SNOMED CT | R | PQ | |||
| Length of Labor | 271562002 | SNOMED CT | R | PQ | |||
| Birth Weight | 364589006 | SNOMED CT | R | PQ | |||
| Sex | 365873007 | SNOMED CT | R | CD | Male Female | ||
| Type of Delivery (Past Pregnancy Outcome) | 267013003 | SNOMED CT | R | CD | Vaginal Caesarian | ||
| Type of Anesthetic | 399084002 | SNOMED CT | R | ST | |||
| Place of Delivery | SNOMED CT | R | narrative text | ST | |||
| Preterm Labor | 6383007 | SNOMED CT | R | BL | |||
Antepartum H&P Social History Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Tobacco Use - Amount per day pre-pregnancy | 365981007 | SNOMED CT | R | PQ | /day | ||
| Tobacco Use - Amount per day post-pregnancy | SNOMED CT | R | PQ | /day | |||
| Tobacco Use - # years use | SNOMED CT | R | PQ | ||||
| Alcohol Use - Amount per day pre-pregnancy | 228273003 / 427013000 | SNOMED CT | R | PQ | /day | ||
| Alcohol Use - Amount per day post-pregnancy | SNOMED CT | R | PQ | /day | |||
| Alcohol Use - # years use | SNOMED CT | R | PQ | ||||
| Illicit/Recreational Drugs - Amount per day pre-pregnancy | 361055000 / 199254001 | SNOMED CT | R | PQ | /day | ||
| Illicit/Recreational Drugs - Amount per day post-pregnancy | SNOMED CT | R | PQ | /day | |||
| Illicit/Recreational Drugs - # years use | SNOMED CT | R | PQ |
Antepartum H&P Family History Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Relevant Family History | 57177007 | SNOMED CT | R | need to specify specific structure here? also have codes for Date(410671006) and Treatment(182991002) |
Antepartum H&P Review of Systems - Genetic Screening Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Thalassemia | 40108008 | SNOMED CT | R | ||||
| Neural Tube Defect | 253098009 | SNOMED CT | R | ||||
| Congenital Heart Defect | 59494005 | SNOMED CT | R | ||||
| Down Syndrome | 41040004 | SNOMED CT | R | ||||
| Tay-Sachs | 111385000 | SNOMED CT | R | ||||
| Canavan Disease | 80544005 | SNOMED CT | R | ||||
| Familial Dysautonomia | 29159009 | SNOMED CT | R | ||||
| Sick Cell Disease | 417357006 | SNOMED CT | R | ||||
| Sick Cell Trait | 16402000 | SNOMED CT | R | ||||
| Hemophilia | 90935002 | SNOMED CT | R | ||||
| Blood Disorders | 266992002 | SNOMED CT | R | ||||
| Muscular Dystrophy | 58795000 | SNOMED CT | R | ||||
| Cystic Fibrosis | 190905008 | SNOMED CT | R | ||||
| Huntington's Chorea | 58756001 | SNOMED CT | R | ||||
| Mental Retardation | 91138005 | SNOMED CT | R | ||||
| Autism | 408856003 | SNOMED CT | R | ||||
| Chrosomosal Disorder | 409709004 | SNOMED CT | R | Other inherited genetic or chromosomal disorder | |||
| Maternal Metabolic Disorder | SNOMED CT | R | metabolic disorder following molar and/or ectopic pregnancies | ||||
| Dysmorphism (Birth Defect) | 276720006 | SNOMED CT | R | Patient or baby's father has a child with birth defects | |||
| Stillbirth | 161743003 | SNOMED CT | R | Recurrent pregnancy loss/stillbirth | |||
| Counseling | 409063005 | SNOMED CT | R | ||||
| Hydrocephaly | SNOMED CT | R | |||||
| History of cleft Lip or palate | SNOMED CT | R | |||||
| Polycystic kidney disease | SNOMED CT | R |
Antepartum H&P Review of Systems - Infection History Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Tuberculosis | 161414005 | SNOMED CT | R | ||||
| Genital Herpes | 402888002 | SNOMED CT | R | ||||
| Viral Exanthem (Viral Rash) | 49882001 | SNOMED CT | R | Rash or viral illness since LMP | |||
| Hepatitis B | SNOMED CT | R | |||||
| Viral Hepatitis C | 50711007 | SNOMED CT | R | ||||
| History of STD | 275881005 | SNOMED CT | R | ||||
| History of Gonorrhea | 274118001 | SNOMED CT | R | Venereal Disease in Pregnancy | |||
| History of Chlamydia | SNOMED CT | R | |||||
| History of HPV | SNOMED CT | R | |||||
| History of HIV | SNOMED CT | R | |||||
| History of Syphilis | SNOMED CT | R |
Antepartum H&P Physical Examination Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| HEENT | 162824006(head) 271894002(eyes) 271896000(ENT) |
SNOMED CT | R | ||||
| FUNDI | SNOMED CT | O | |||||
| Teeth | 270479002 | SNOMED CT | R | ||||
| Thyroid | 162836000 | SNOMED CT | R | ||||
| Breasts | 163433006 | SNOMED CT | R | ||||
| Lungs | 423649001 | SNOMED CT | R | ||||
| Heart | 309652009 | SNOMED CT | R | ||||
| Abdomen | 271911005 | SNOMED CT | R | ||||
| Extremeties | 164443003 | SNOMED CT | R | ||||
| Skin | 271303006 | SNOMED CT | R | ||||
| Lymph Nodes | 284427004 | SNOMED CT | R | ||||
| Vulva | 275961008 | SNOMED CT | R | ||||
| Vagina | 274297000 | SNOMED CT | R | ||||
| Cervix | 309668003 | SNOMED CT | R | ||||
| Uterus Size | 163509002(fundus = term size) 163498004(gravid uterus size) |
SNOMED CT | R | ||||
| Adnexa | SNOMED CT | R | |||||
| Rectum | SNOMED CT | R | |||||
| Diagonal Conjugate | SNOMED CT | O | |||||
| Spines | 163576005 | SNOMED CT | O | ||||
| Sacrum | 164565001 | SNOMED CT | O | ||||
| Subpubic Arch | SNOMED CT | O | |||||
| Gynecoid Pelvic Type | 163555000 | SNOMED CT | O |
Antepartum H&P Vital Signs Entries
| CDA Entry | Code(s) | Code System | Opt | Comments | xsi:Type | units | value set |
|---|---|---|---|---|---|---|---|
| Weight | 424927000(w/shoes) 425024002(w/o shoes) |
SNOMED CT | R | ||||
| Height | 24833004 | SNOMED CT | R | ||||
| BMI | 60621009 | SNOMED CT | R | ||||
| Blood Pressure | 75367002 | SNOMED CT | R |
Antepartum Laboratory (APL)
Data Element Index
| Data Element | CDA Section | Comments |
|---|---|---|
| Antepartum Laboratory Results | Survey Panel | SHALL use LOINC code xx-APL for the section |
Document Specification
| Data Element | Opt | Section | Template ID |
|---|---|---|---|
| Survey Panel This section SHALL contain one or more Coded Results Sections and SHOULD use LOINC codes from the antepartum laboratory LOINC code list when possible. A document consumer SHOULD render these data in ascending date order. This ascending date order offers a visual representation that aids in the understanding of the course of care for antepartum laboratory tests. |
R | 1.3.6.1.4.1.19376.1.5.3.1.1.12.3.7 |
Sample LOINC Code List
| Lab | LOINC Code | Comments |
|---|---|---|
| Antibody Screen | 890-4 | |
| Blood Type | 883-9/10331-7/14578-9 | |
| HBsAg | 5195-3/5196-1/5197-9/7905-3 | |
| HCT_HGB | 718-7/4544-3/30350-3 | |
| Pap Test | 21440-3/21441-1/10524-7/18500-9/19765-7/19766-5 | |
| Rubella | 5334-8/25514-1/40667-8/8014-3 | |
| etc. |
Sample Antepartum Laboratory Document
<!-- Survey Panel -->
<organizer classCode="CLUSTER" moodCode="EVN">
<templateId root="2.16.840.1.113883.10.20.1.32"/>
<templateId root="1.3.6.1.4.1.19376.1.5.3.1.1.12.3.7"/>
<id root="" extension=""/>
<code code=" " displayName=" " codeSystem=" " codeSystemName=" "/>
<statusCode code="completed"/>
<effectiveTime value=""/>
<!-- one or more survey observations -->
<component typeCode="COMP">
<observation classCode="OBS" moodCode="EVN">
<templateId root="1.3.6.1.4.1.19376.1.5.3.1.1.12.3.6"/>
<!-- Coded Results -->
<templateId root="1.3.6.1.4.1.19376.1.5.3.1.3.28"/>
<id root=" " extension=" "/>
<code code="30954-2" displayName="STUDIES SUMMARY" codeSystem="2.16.840.1.113883.6.1" codeSystemName="LOINC"/>
<text>Text as described above</text>
<entry>
<procedure classCode="PROC" moodCode="EVN|INT">
<templateId root="1.3.6.1.4.1.19376.1.5.3.1.1.19"/>
<templateId root="2.16.840.1.113883.10.20.1.29"/>
<!-- see text of section 0 -->
<templateId root="2.16.840.1.113883.10.20.1.25"/>
<!-- see text of section 0 -->
<id root="" extension=""/>
<code code="890-4" codeSystem="2.16.840.1.113883.6.1" codeSystemName="LOINC" displayName="Antibody screen"/>
<text>
<reference value="#xxx"/>
</text>
<statusCode code="completed|active|aborted|cancelled"/>
<effectiveTime>
<low value=""/>
<high value=""/>
</effectiveTime>
<priorityCode code=""/>
<approachSiteCode code="" displayName="" codeSystem="" codeSystemName=""/>
<targetSiteCode code="" displayName="" codeSystem="" codeSystemName=""/>
<author/>
<informant/>
<entryRelationship typeCode="REFR">
<encounter classCode="ENC" moodCode="">
<templateId root="1.3.6.1.4.1.19376.1.5.3.1.4.4.1"/>
<id root="" extension=""/>
</encounter>
</entryRelationship>
<entryRelationship typeCode="RSON">
<act classCode="ACT" moodCode="EVN">
<templateId root="1.3.6.1.4.1.19376.1.5.3.1.4.4.1"/>
<id root="" extension=""/>
</act>
</entryRelationship>
</procedure>
</entry>
</observation>
</component>
</organizer>
Antepartum Education (APE)
Data Element Index
| Data Elements | CDA Section | Comments |
|---|---|---|
| Antepartum Education and Consents | Coded Patient Education and Consents | SHALL use LOINC code xx-APE for the section |
Document Specification
| Data Element | Opt | Section | Template ID |
|---|---|---|---|
| Coded Patient Education and Consents | R | 1.3.6.1.4.1.19376.1.5.3.1.1.9.39 |
Sample Snomed CT Code List
| Lab | LOINC Code | Comments |
|---|---|---|
| Risk factors identified by prenatal history | xxxxa | |
| Anticipated course of prenatal care | xxxxb | |
| Nutrition and weight gain counseling; special diet | xxxxc | |
| Toxoplasmosis precautions (cats/raw meat) | xxxxd | |
| Sexual activity | xxxxe | |
| etc. |
Antepartum Education Sample
<component>
<section>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.1.9.38'/>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.1.9.39'/>
<id root=' ' extension=' '/>
<code code='34895-3' displayName='EDUCATION NOTE'
codeSystem='2.16.840.1.113883.6.1' codeSystemName='LOINC'/>
<text>
Text as described above
</text>
<entry>
<!-- Required Procedure Entry element -->
<procedure classCode='PROC' moodCode='EVN|INT'>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.1.19'/>
<templateId root='2.16.840.1.113883.10.20.1.29'/><!-- see text of section 0 -->
<templateId root='2.16.840.1.113883.10.20.1.25'/><!-- see text of section 0 -->
<id root='' extension=''/>
<code code='xxxxxa' codeSystem='2.16.840.1.113883.6.96' codeSystemName='SNOMEDCT'
displayName='Risk factors'/>
<text><reference value='#xxx'/></text>
<statusCode code='completed|active|aborted|cancelled'/>
<effectiveTime>
<low value=''/>
<high value=''/>
</effectiveTime>
<priorityCode code=''/>
<approachSiteCode code='' displayName='' codeSystem='' codeSystemName=''/>
<targetSiteCode code='' displayName='' codeSystem='' codeSystemName=''/>
<author />
<informant />
<entryRelationship typeCode='REFR'>
<encounter classCode='ENC' moodCode=''>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.4.4.1'/>
<id root='' extension=''/>
</encounter>
</entryRelationship>
<entryRelationship typeCode='RSON'>
<act classCode='ACT' moodCode='EVN'>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.4.4.1'/>
<id root='' extension=''/>
</act>
</entryRelationship>
</procedure>
<procedure classCode='PROC' moodCode='EVN|INT'>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.1.19'/>
<templateId root='2.16.840.1.113883.10.20.1.29'/><!-- see text of section 0 -->
<templateId root='2.16.840.1.113883.10.20.1.25'/><!-- see text of section 0 -->
<id root='' extension=''/>
<code code='xxxxb' codeSystem='2.16.840.1.113883.6.96' codeSystemName='SNOMEDCT'
displayName='Anticipated course of care'/>
<text><reference value='#xxx'/></text>
<statusCode code='completed|active|aborted|cancelled'/>
<effectiveTime>
<low value=''/>
<high value=''/>
</effectiveTime>
<priorityCode code=''/>
<approachSiteCode code='' displayName='' codeSystem='' codeSystemName=''/>
<targetSiteCode code='' displayName='' codeSystem='' codeSystemName=''/>
<author />
<informant />
<entryRelationship typeCode='REFR'>
<encounter classCode='ENC' moodCode=''>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.4.4.1'/>
<id root='' extension=''/>
</encounter>
</entryRelationship>
<entryRelationship typeCode='RSON'>
<act classCode='ACT' moodCode='EVN'>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.4.4.1'/>
<id root='' extension=''/>
</act>
</entryRelationship>
</procedure>
</entry>
<entry>
<!-- Required if known Simple Observations element -->
<observation typeCode='OBS' moodCode='EVN'>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.4.13'/>
<id root='' extension=''/>
<code code='' displayName='' codeSystem='' codeSystemName=''/>
<!-- for CDA -->
<text><reference value='#xxx'/></text>
<!-- For HL7 Version 3 Messages
<text>text</text>
-->
<statusCode code='completed'/>
<effectiveTime value=''/>
<repeatNumber value=''/>
<value xsi:type='' …/>
<interpretationCode code='' codeSystem='' codeSystemName=''/>
<methodCode code='' codeSystem='' codeSystemName=''/>
<targetSiteCode code='' codeSystem='' codeSystemName=''/>
<author typeCode='AUT'>
<assignedAuthor typeCode='ASSIGNED'><id></assignedAuthor> <!-- for CDA -->
<!-- For HL7 Version 3 Messages
<assignedEntity typeCode='ASSIGNED'>
<Person classCode='PSN'>
<determinerCode root=''>
<name>…</name>
</Person>
<assignedEntity>
-->
</author>
</observation>
</entry>
<entry>
<!-- Required if known External References element -->
<entry>
<act classCode='ACT' moodCode='EVN'>
<templateId root='1.3.6.1.4.1.19376.1.5.3.1.4.4'/>
<id root='' extension=''/>
<code nullFlavor='NA' />
<text><reference value='#study-1'/></text>
<!-- For CDA -->
<reference typeCode='REFR|SPRT'>
<externalDocument classCode='DOC' moodCode='EVN'>
<id extension='' root=''/>
<text><reference value='http://foo..'/></text>
</externalDocument>
</reference>
<!-- For HL7 Version 3 Messages
<sourceOf typeCode='REFR|SPRT'>
<act classCode='DOC' moodCode='EVN'>
<id extension='' root=''/>
<text><reference value='http://foo…'</text>
</act>
</sourceOf>
-->
</act>
</entry>
</entry>
</section>
</component>