PCC Technical Framework Wikified: Difference between revisions
| Line 142: | Line 142: | ||
Year=2006-2007| | Year=2006-2007| | ||
Status=Draft}} | Status=Draft}} | ||
{{:Preface to Volume 2 of the PCC Technical Framework}} | |||
{{:Introduction to Volume 2 of the PCC Technical Framework}} | |||
{{:IHE Patient Care Coordination Transactions}} | |||
{{:IHE Patient Care Coordination Bindings}} | |||
{{:IHE Patient Care Coordination Namespaces and Vocabularies}} | |||
== Conventions == | |||
== Folder Content Modules == | |||
== CDA Release 2.0 Content Modules == | |||
This section contains content modules based upon the HL7 CDA Release 2.0 Standard, and related standards and/or implementation guides. | |||
=== CDA Document Content Modules === | |||
=== CDA Header Content Modules === | |||
=== CDA Section Content Modules === | |||
=== CDA Entry Content Modules === | |||
Revision as of 11:30, 11 May 2007
HIMSS and RSNA
Integrating the Healthcare Enterprise
IHE Patient Care Coordination
Technical Framework
Volumes I and II
Revision 2.0
2006-2007
Draft
http://forums.rsna.org under the “IHE” forum
Select the appropriate sub-forum for the technical framework you are commenting upon.
Forward
Integrating the Healthcare Enterprise (IHE) is an initiative designed to stimulate the integration of the information systems that support modern healthcare institutions. Its fundamental objective is to ensure that in the care of patients all required information for medical decisions is both correct and available to healthcare professionals. The IHE initiative is both a process and a forum for encouraging integration efforts. It defines a technical framework for the implementation of established messaging standards to achieve specific clinical goals. It includes a rigorous testing process for the implementation of this framework. And it organizes educational sessions and exhibits at major meetings of medical professionals to demonstrate the benefits of this framework and encourage its adoption by industry and users.
The approach employed in the IHE initiative is not to define new integration standards, but rather to support the use of existing standards, HL7, DICOM, IETF, and others, as appropriate in their respective domains in an integrated manner, defining configuration choices when necessary. When clarifications or extensions to existing standards are necessary, IHE refers recommendations to the relevant standards bodies.
This initiative has numerous sponsors and supporting organizations in different medical specialty domains and geographical regions. In North America the primary sponsors are the American College of Cardiology (ACC), the Healthcare Information and Management Systems Society (HIMSS) and the Radiological Society of North America (RSNA). IHE Canada has also been formed. IHE Europe (IHE-EUR) is supported by a large coalition of organizations including the European Association of Radiology (EAR) and European Congress of Radiologists (ECR), the Coordination Committee of the Radiological and Electromedical Industries (COCIR), Deutsche Röntgengesellschaft (DRG), the EuroPACS Association, Groupement pour la Modernisation du Système d'Information Hospitalier (GMSIH), Société Francaise de Radiologie ([www.sfr-radiologie.asso.fr SFR]), and Società Italiana di Radiologia Medica (SIRM). In Japan IHE-J is sponsored by the Ministry of Economy, Trade, and Industry (METI); the Ministry of Health, Labor, and Welfare; and [www.medis.or.jp MEDIS-DC]; cooperating organizations include the Japan Industries Association of Radiological Systems (JIRA), the Japan Association of Healthcare Information Systems Industry (JAHIS), Japan Radiological Society (JRS), Japan Society of Radiological Technology (JSRT), and the Japan Association of Medical Informatics (JAMI). Other organizations representing healthcare professionals are actively involved and others are invited to join in the expansion of the IHE process across disciplinary and geographic boundaries.
The IHE Technical Frameworks for the various domains (Patient Care Coordination, IT Infrastructure, Cardiology, Laboratory, Radiology, etc.) define specific implementations of established standards to achieve integration goals that promote appropriate sharing of medical information to support optimal patient care. These are expanded annually, after a period of public review, and maintained regularly through the identification and correction of errata. The current version for these Technical Frameworks may be found at www.ihe.net.
The IHE Technical Framework identifies a subset of the functional components of the healthcare enterprise, called IHE Actors, and specifies their interactions in terms of a set of coordinated, standards-based transactions. It describes this body of transactions in progressively greater depth. Volume I provides a high-level view of IHE functionality, showing the transactions organized into functional units called Integration Profiles that highlight their capacity to address specific clinical needs. Subsequent volumes provide detailed technical descriptions of each IHE transaction.
Content of the Technical Framework
This technical framework defines relevant standards and constraints on those standards in order to implement a specific use cases for the transfer of information between systems. This document is organized into 2 volumes as follows:
Volume 1 – Overview
This volume is provided as a high level overview of the profiles including descriptions of the use case, the actors involved, the process flow, and dependencies on other standards and IHE profiles. It is of interest to care providers, vendors' management and technical architects and to all users of the profile
Volume 2 – Transactions and Content Profiles
This volume is intended as a technical reference for the implementation of specific transactions in the use case including references to the relevant standards, constraints, and interaction diagrams. It is intended for the technical implementers of the profile.
How to Contact Us
IHE Sponsors welcome comments on this document and the IHE initiative. They should be directed to the discussion server at http://forums.rsna.org or to:
Didi Davis
Director of Integrating the Healthcare Enterprise
230 East Ohio St., Suite 500
Chicago, IL 60611
Email: ihe@himss.org
Volume 1
HIMSS and RSNA
Integrating the Healthcare Enterprise
IHE Patient Care Coordination
Technical Framework
Volumes I
Revision 2.0
2006-2007
Draft
Preface to Volume 1 of the PCC Technical Framework
Intended Audience
The intended audience of this document is:
- Healthcare professionals involved in informatics
- IT departments of healthcare institutions
- Technical staff of vendors participating in the IHE initiative
- Experts involved in standards development
- Those interested in integrating healthcare information systems and workflows
Related Information for the Reader
The reader of volume 1 should read or be familiar with the following documents:
- Volume 1 of the Cross-Enterprise Document Sharing (XDS) Integration Profile documented in the ITI Infrastructure Technical Framework
(See http://www.ihe.net/Technical_Framework/index.cfm ).
- Volume 1 of the Notification of Document Availability (NAV) Integration Profile documented in the ITI Infrastructure Technical Framework
(See http://www.ihe.net/Technical_Framework/index.cfm ).
- Volume 1 of the Audit Trail and Node Authentication (ATNA) Integration Profile documented in the ITI Infrastructure Technical Framework
(See http://www.ihe.net/Technical_Framework/index.cfm ).
- HL7 Clinical Document Architecture Release 2: Section 1, CDA Overview.
- Care Record Summary – Implementation Guide for CDA Release 2 (US Realm): Section 1
- Presentations from IHE Workshop: Effective Integration of the Enterprise and the Health System - June 28–29, 2005: http://www.ihe.net/Participation/workshop_2005.cfm, June 2005:
- Leveraging IHE to Build RHIO Interoperability
- Cross-Enterprise Document Sharing (XDS)
- Notification of Document Availability (NAV)
- Patient Care Coordination
- Use Cases for Medical Summaries
- Patient Care Coordination - Overview of Profiles
How this Volume is Organized
Section 2 describes the general nature, structure, purpose and function of the Technical Framework. Section 3 and the subsequent sections of this volume provide detailed documentation on each integration profile, including the Patient Care Coordination problem it is intended to address and the IHE actors and transactions it comprises.
The appendices following the main body of the document provide a summary list of the actors and transactions, detailed discussion of specific issues related to the integration profiles and a glossary of terms and acronyms used.
Conventions Used in this Document
This document has adopted the following conventions for representing the framework concepts and specifying how the standards upon which the IHE Technical Framework is based should be applied.
Technical Framework Cross-references
When references are made to another section within a Technical Framework volume, a section number is used by itself. When references are made to other volumes or to a Technical Framework in another domain, the following format is used:
<domain designator> TF-<volume number>: <section number>
where:
- <domain designator>
- is a short designator for the IHE domain (PCC= Patient Care Coordination, ITI = IT Infrastructure, RAD = Radiology)
- <volume number>
- is the applicable volume within the given Domain Technical Framework (e.g., 1, 2, 3), and
- <section number>
- is the applicable section number.
For example: PCC TF-1: 3.1 refers to Section 3.1 in volume 1 of the IHE Patient Care Coordination Technical Framework, ITI TF-2: 4.33 refers to Section 4.33 in volume 2 of the IHE IT Infrastructure Technical Framework.
IHE Actor and Transaction Diagrams and Tables
Each integration profile is a representation of a real-world capability that is supported by a set of actors that interact through transactions. Actors are information systems or components of information systems that produce, manage, or act on categories of information required by operational activities in the enterprise. Transactions are interactions between actors that communicate the required information through standards-based messages.
The diagrams and tables of actors and transactions in subsequent sections indicate which transactions each actor in a given profile must support.
The transactions shown on the diagrams are identified both by their name and the transaction number as defined in PCC TF-2 (Volume 2 of the PCC Technical framework). The transaction numbers are shown on the diagrams as bracketed numbers prefixed with the specific Technical Framework domain.
In some cases, a profile is dependent on a prerequisite profile in order to function properly and be useful. For example, Cross-Enterprise Sharing of Medical Summaries depends on Audit Trail and Node Authentication (ATNA). These dependencies can be found by locating the desired profile in the dependencies section of this document to determine which profile(s) are listed as prerequisites. An actor must implement all required transactions in the prerequisite profiles in addition to those in the desired profile.
Process Flow Diagrams
The descriptions of integration profiles that follow include process flow diagrams that illustrate how the profile functions as a sequence of transactions between relevant actors.
These diagrams are intended to provide an overview so the transactions can be seen in the context of an institution’s or cross-institutions’ workflow. Certain transactions and activities not defined in detail by IHE are shown in these diagrams in italics to provide additional context on where the relevant IHE transactions fit into the broader scheme of healthcare information systems. These diagrams are not intended to present the only possible scenario. Often other actor groupings are possible, and transactions from other profiles may be interspersed.
In some cases the sequence of transactions may be flexible. Where this is the case there will generally be a note pointing out the possibility of variations. Transactions are shown as arrows oriented according to the flow of the primary information handled by the transaction and not necessarily the initiator.
Copyright Permissions
Health Level Seven, Inc., has granted permission to the IHE to reproduce tables from the HL7 standard. The HL7 tables in this document are copyrighted by Health Level Seven, Inc. All rights reserved. Material drawn from these documents is credited where used.
IHE has been very fortunate in having the American College of Obstetricians and Gynecologists (ACOG) help us in the definition of the data found in the Antepartum Summary Profile (APS).
The Antepartum Summary Profile (APS) describes the content structures and specifications the American College of Obstetricians and Gynecologists (ACOG) views are necessary in an antepartum record. ACOG encourages the use of the content structures contained in the Antepartum Summary Profile of the Patient Care Coordination Technical Framework. ACOG does not endorse any EMR products. Companies or individuals that use these content structures in EMR product or service are prohibited from using ACOG's name and/or its logo on any promotional material, packaging, advertisement, website or in any other context related to the EMR product or service.
Braden Scale For Predicting Pressure Sore Risk, Copyright © Barbara Braden and Nancy Bergstrom, 1988. Reprinted with permission. Barabara Braden and Nancy Bergstrom have granted permission to use the Braden Scale in the IHE Functional Status Assessment Integration Profile to be provided to vendors for demonstration purposes only. Should a vendor chose to include the Braden Scale in their product, they must seek permission to do so from the copyright holders. More information is available from http://www.bradenscale.com/
Introduction
This document, the IHE Patient Care Coordination Technical Framework (PCC TF), defines specific implementations of established standards. These are intended to achieve integration goals that promote appropriate exchange of medical information to coordinate the optimal patient care among care providers in different care settings. It is expanded annually, after a period of public review, and maintained regularly through the identification and correction of errata. The latest version of the document is always available via the Internet at http://www.ihe.net/Technical_Framework/ , where the technical framework volumes specific to the various healthcare domains addressed by IHE may be found.
The IHE Patient Care Coordination Technical Framework identifies a subset of the functional components of the healthcare enterprises and health information networks, called IHE actors, and specifies their interactions in terms of a set of coordinated, standards-based transactions. The other domains within the IHE initiative also produce Technical Frameworks within their respective areas that together form the IHE Technical Framework. Currently, the following IHE Technical Framework(s) are available:
- IHE IT Infrastructure Technical Framework
- IHE Cardiology Technical Framework
- IHE Laboratory Technical framework
- IHE Radiology Technical Framework
- IHE Patient Care Coordination Technical Framework
Where applicable, references are made to other technical frameworks. For the conventions on referencing other frameworks, see the preface of this volume.
Relationship to Standards
The IHE Technical Framework identifies functional components of a distributed healthcare environment (referred to as IHE actors), solely from the point of view of their interactions in the healthcare enterprise. It further defines a coordinated set of transactions based on standards (such as HL7, IETF, ASTM, DICOM, ISO, OASIS, etc.) in order to accomplish a particular use case. As the scope of the IHE initiative expands, transactions based on other standards may be included as required.
At its current level of development, IHE has also created Content Integration Profiles to further specify the payloads of these transactions, again based on standards. This has become necessary as the healthcare industry moves towards the use of transaction standards that have been used in more traditional computing environments.
In some cases, IHE recommends selection of specific options supported by these standards. However, IHE does not introduce technical choices that contradict conformance to these standards. If errors in or extensions to existing standards are identified, IHE’s policy is to report them to the appropriate standards bodies for resolution within their conformance and standards evolution strategy.
IHE is therefore an implementation framework, not a standard. Conformance claims for products must still be made in direct reference to specific standards. In addition, vendors who have implemented IHE integration capabilities in their products may publish IHE Integration Statements to communicate their products’ capabilities. Vendors publishing IHE Integration Statements accept full responsibility for their content. By comparing the IHE Integration Statements from different products, a user familiar with the IHE concepts of actors and integration profiles can determine the level of integration between them. See PCC TF-1: Appendix C for the format of IHE Integration Statements.
Relationship to Product Implementations
The IHE actors and transactions described in the IHE Technical Framework are abstractions of the real-world healthcare information system environment. While some of the transactions are traditionally performed by specific product categories (e.g. HIS, Clinical Data Repository, Electronic Health record systems, Radiology Information Systems, Clinical Information Systems or Cardiology Information Systems), the IHE Technical Framework intentionally avoids associating functions or actors with such product categories. For each actor, the IHE Technical Framework defines only those functions associated with integrating information systems. The IHE definition of an actor should therefore not be taken as the complete definition of any product that might implement it, nor should the framework itself be taken to comprehensively describe the architecture of a healthcare information system.
The reason for defining actors and transactions is to provide a basis for defining the interactions among functional components of the healthcare information system environment. In situations where a single physical product implements multiple functions, only the interfaces between the product and external functions in the environment are considered to be significant by the IHE initiative. Therefore, the IHE initiative takes no position as to the relative merits of an integrated environment based on a single, all-encompassing information system versus one based on multiple systems that together achieve the same end.
Framework Development and Maintenance
The IHE Patient Care Coordination Technical Framework is continuously maintained and expanded on an annual basis by the IHE Patient Care Coordination Technical Committee. The development and maintenance process of the Framework follows a number of principles to ensure stability of the specification so that both vendors and users may use it reliably in specifying, developing and acquiring systems with IHE integration capabilities.
The first of these principles is that any extensions or clarifications to the Technical Framework must maintain backward compatibility with previous versions of the framework (except in rare cases for corrections) in order to maintain interoperability with systems that have implemented IHE Actors and Integration Profiles defined there. The IHE Patient Care Coordination Technical Framework is developed and re-published annually following a three-step process:
- The Patient Care Coordination Technical Committee develops supplements to the current stable version of the Technical Framework to support new functionality identified by the IHE Strategic and PCC Planning Committees and issues them for public comment.
- The Committee addresses all comments received during the public comment period and publishes an updated version of the Technical Framework for “Trial Implementation.” This version contains both the stable body of the Technical Framework from the preceding cycle and the newly developed supplements. It is this version of the Technical Framework that is used by vendors in developing trial implementation software for the IHE Connectathons.
- The Committee regularly considers change proposals to the Trial Implementation version of the Technical Framework, including those from implementers who participate in the Connectathon. After resolution of all change proposals received within 60 days of the Connectathon, the Technical Framework version is published as “Final Text”.
As part of the Technical framework maintenance the Committee will consider change proposals received after the publication to the “Final Text”.
History of Annual Changes
In the 2005-2006 cycle of the IHE Patient Care Coordination initiative, the first release of the IHE PCC Technical Framework introduced the following integration profile:
- Cross-Enterprise Sharing of Medical Summaries (XDS-MS) – a mechanism to automate the sharing process between care providers of Medical Summaries, a class of clinical documents that contain the most relevant portions of information about the patient intended for a specific provider or a broad range of potential providers in different settings. Medical Summaries are commonly created and consumed at points in time of transfers of care such as referrals or discharge.
In the 2006-2007 cycle of the IHE Patient Care Coordination initiative, the follow integration profiles were added to the technical framework.
- Exchange of Personal Health Record Content (XPHR) – provides a standards-based specification for managing the interchange of documents between a Personal Health Record used by a patient and systems used by other healthcare providers to enable better interoperability between these systems.
- Basic Patient Privacy Consents (BPPC) – enables XDS Affinity Domains to be more flexible in the privacy policies that they support, by providing mechanisms to record patient privacy consents, enforce these consents, and create Affinity Domain defined consent vocabularies that identify information sharing policies.
- Preprocedure History and Physical Content Profile (PPHP) – supports the exchange of information allowing for the assessment and amelioration of risks related to a procedure.
- Emergency Department Referral Profile (EDR) – provides a means to communicate medical summary data from an EHR System to an EDIS System.
About the Patient Care Coordination Integration Profiles
IHE Integration Profiles offer a common language that healthcare professionals and vendors can use to discuss integration needs of healthcare enterprises and the integration capabilities of information systems in precise terms. Integration Profiles specify implementations of standards that are designed to meet identified clinical needs. They enable users and vendors to state which IHE capabilities they require or provide, by reference to the detailed specifications of the IHE Patient Care Coordination Technical Framework.
Integration profiles are defined in terms of IHE Actors, transactions and their content. Actors (listed in PCC TF-1: Appendix A) are information systems or components of information systems that produce, manage, or act on information associated with clinical and operational activities. Transactions (listed in PCC TF-1: Appendix B) are interactions between actors that communicate the required information through standards-based messages. Content is what is exchanged in these transactions, and are defined by Content Profiles.
Vendor products support an Integration Profile by implementing the appropriate actor(s) and transactions. A given product may implement more than one actor and more than one integration profile.
Content Profiles define how the content used in a transaction is structured. Each transaction is viewed as having two components, a payload, which is the bulk of the information being carried, and metadata that describes that payload. The binding of the Content to an IHE transaction specifies how this payload influences the metadata of the transaction. Content modules within the Content Profile then define the payloads. Content modules are transaction neutral, in that what they describe is independent of the transaction in which they are used, whereas content bindings explain how the payload influences the transaction metadata.
The figure below shows the relations between the Content Integration Profiles of the Patient Care Coordination Domain.
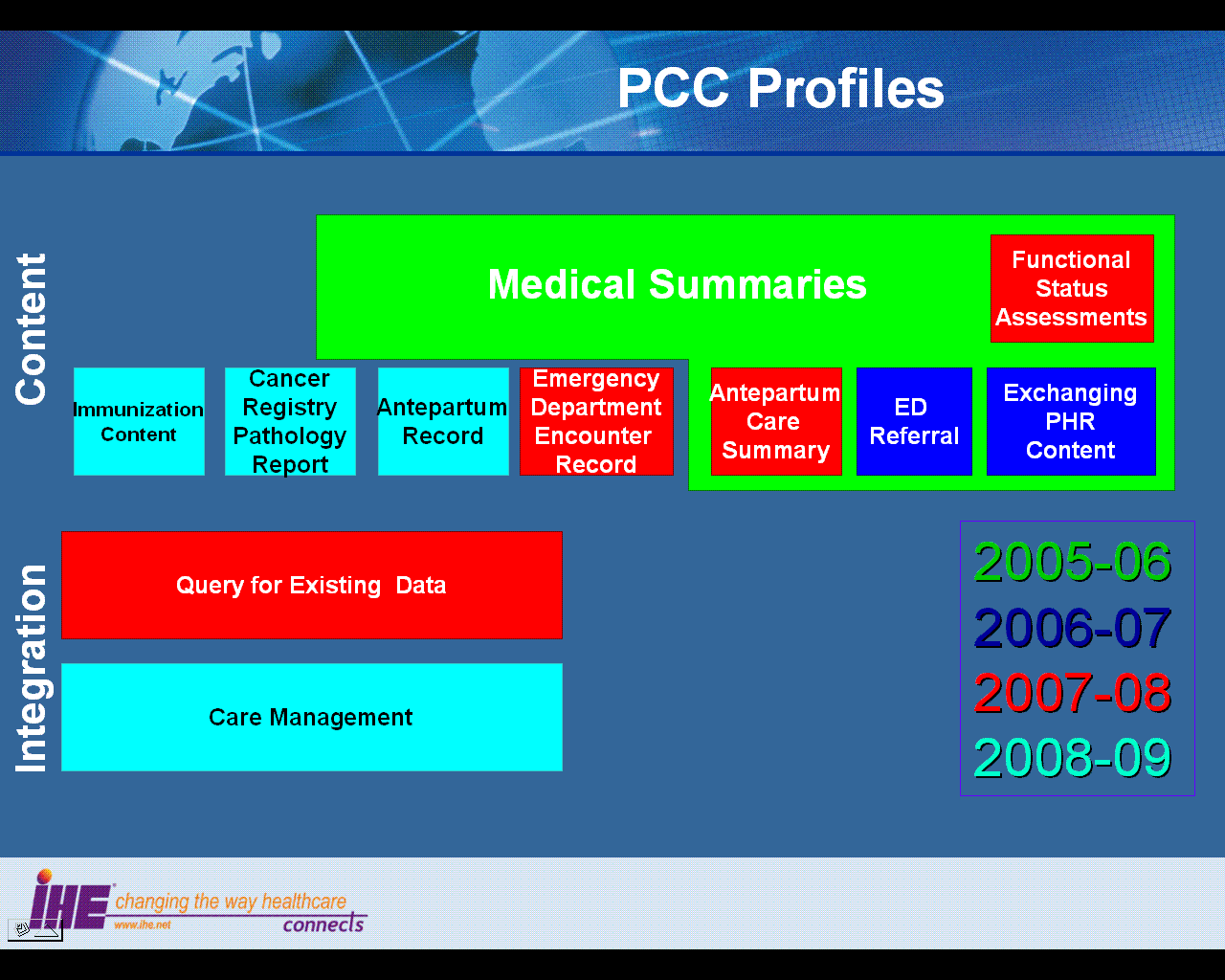
Dependencies of the PCC Integration Profiles
Dependencies among IHE Integration Profiles exist when implementation of one integration profile is a prerequisite for achieving the functionality defined in another integration profile. The table below defines these dependencies. Some dependencies require that an actor supporting one profile be grouped with one or more actors supporting other integration profiles. For example, Cross-Enterprise Sharing of Medical Summaries (XDS-MS) requires that its actors be grouped with a Secured Node Actor of the Audit Trail and Node Authentication (ATNA) Integration Profile. The dependency exists because XDS-MS and XDS actors must support a secured communication channel with proper auditing of the exchange of patient identified information in order to function properly in an environment where protection of patient privacy is critical.
| Integration Profile | Depends on | Dependency Type | Purpose |
| All PCC Content Profiles |
Audit Trail and Node Authentication (ATNA) | Each Content Creator and Content Consumer actor shall be grouped with the ATNA Secured Node Actor | Required to manage audit trail of exported PHI, node authentication, and transport encryption. |
| Consistent Time (CT) | Each Content Creator and Content Consumer actor shall be grouped with the Time Client Actor | Required to manage and resolve conflicts in multiple updates. | |
| Functional Status Assessments (FSA) | Cross Enterprise Document Exchange of Medical Summaries (XDS-MS) OR Exchange of Personal Health Record Content (XPHR) OR Emergency Department Referral (EDR) |
Content Consumers implementing the Functional Status Assessments profile shall be grouped with either the XDS-MS, XPHR or EDR Content Consumer. Content Creators implementing the Functional Status Assessments profile shall be grouped with either the XDS-MS, XPHR or EDR Content Creator. | Ensures that the Functional Status Assessment is communicated as part of an exchange of medical summary information. |
| Functional Status Assessments (QED) | Audit Trail and Node Authentication (ATNA) | Each actor in this profile shall be grouped with the ATNA Secure Node or Secure Application actor. | Required to manage audit trail of exported PHI, node authentication, and transport encryption. |
| Consistent Time (CT) | Each actor in this profile shall be grouped with the Time Client Actor | Required to manage and resolve conflicts in multiple updates. |
To support a dependent profile, an actor must implement all required transactions in the prerequisite profiles in addition to those in the dependent profile. In some cases, the prerequisite is that the actor selects any one of a given set of profiles.
PCC Integration Profiles Overview
In this document, each IHE Integration Profile is defined by:
- The IHE actors involved
- The specific set of IHE transactions exchanged by each IHE actor.
- The content of the IHE transactions
These requirements are presented in the form of a table of transactions required for each actor supporting the Integration Profile. Actors supporting multiple Integration Profiles are required to support all the required transactions of each Integration Profile supported. When an Integration Profile depends upon another Integration Profile, the transactions required for the dependent Integration Profile have not been included in the table.
The content of the transactions are presented as Content Integration Profiles. These are specification of the content to be exchange, along with explanations (called bindings) of how the content affects the transactions in which it is exchanged. It is expected that Content Integration Profiles will be used environments where the physician offices and hospitals have a coordinated infrastructure that serves the information sharing needs of this community of care. Several mechanisms are supported by IHE profiles:
- A registry/repository-based infrastructure is defined by the IHE Cross-Enterprise Document Sharing (XDS) and other IHE Integration Profiles such as patient identification (PIX & PDQ), and notification of availability of documents (NAV).
- A media-based infrastructure is defined by the IHE Cross-Enterprise Document Media Interchange (XDM) profile.
- A reliable messaging-based infrastructure is defined by the IHE Cross-Enterprise Document Reliable Interchange (XDR) profile.
- All of these infrastructures support Security and privacy through the use of the Consistent Time (CT) and Audit Trail and Node Authentication (ATNA) profiles.
For more details on these profiles, see the IHE IT Infrastructure Technical Framework, found here: http://www.ihe.net/Technical_Framework/.
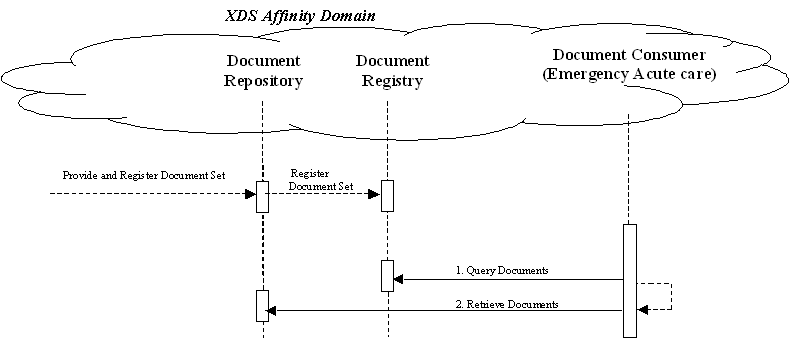
Such an infrastructure is assumed by the use cases that focus on the context for defining the specific clinical information content for this profile. These content integration profiles use similar transactions and differ only in the content exchanged. A process flow for these use cases using Cross Enterprise Document Sharing (XDS) and Notification of Document Availability (NAV) is shown in the figure below. Other process flows are possible using XDM and/or XDR.

These steps are:
- Extract/capture a collection of records into a set of documents packaged as an XDS Submission Set. This submission contains at least one clinical document, and may contain a number of other related clinical documents. For example, Medical Summaries are clinical documents (already known in the paper world), which often serve the dual purpose of documenting an encounter and providing the rationale for sending the information to another provider. This step utilizes the transactions provided by the ITI XDS profile to place the records in an XDS Repository (local or shared).
- The Repository ensures that the documents of the submission set are registered with the XDS Registry of the Affinity Domain (set of cooperating care delivery institutions).
- Notify the other provider that documents are now available for review. This step utilizes the transactions provided by the ITI NAV profile to perform the e-mail notification.
- The e-mail notification that contains no patient identified information is received by the specialist EMR system.
- The receiving provider can then utilize existing query transactions from the XDS profile to find the URL of the Documents.
- Finally, the receiving provider may choose to display the document, or import relevant information from these records into their own EMR system.
Unplanned Access to past Content
In many cases, a provider may need to assess information from the patient care history, and patients may have content in the XDS repository from prior visits to other providers. For example, Medical Summaries, as well as other documents such as laboratory and radiology reports are critical for emergency physicians and nurses to provide the best care to patient in acute conditions. The figure below shows the transactions required for this use case, again, using XDS. Other process flows are possible using XDM and/or XDR.
Note that IHE Integration Profiles are not statements of conformance to standards, and IHE is not a certifying body. Users should continue to request that vendors provide statements of their conformance to standards issued by relevant standards bodies, such as HL7 and DICOM. Standards conformance is a prerequisite for vendors adopting IHE Integration Profiles.
Also note that there are critical requirements for any successful integration project that IHE cannot address. Successfully integrating systems still requires a project plan that minimizes disruptions and describes fail-safe strategies, specific and mutually understood performance expectations, well-defined user interface requirements, clearly identified systems limitations, detailed cost objectives, plans for maintenance and support, etc.
Product Implementations
Developers have a number of options in implementing IHE actors and transactions in product implementations. The decisions cover three classes of optionality:
- For a system, select which actors it will incorporate (multiple actors per system are acceptable).
- For each actor, select the integration profiles in which it will participate.
- For each actor and profile, select which options will be implemented.
All required transactions must be implemented for the profile to be supported (for XDS-MS, refer to the transaction descriptions for XDS in ITI TF-2).
Implementers should provide a statement describing which IHE actors, IHE integration profiles and options are incorporated in a given product. The recommended form for such a statement is defined in PCC TF-1: Appendix C.
In general, a product implementation may incorporate any single actor or combination of actors. When two or more actors are grouped together, internal communication between actors is assumed to be sufficient to allow the necessary information flow to support their functionality; for example, the Document Source Actor of XDS-MS may use the Patient Identifier Cross-reference Consumer Actor to obtain the necessary patient identifier mapping information from its local patient id to that used in the document sharing domain. The exact mechanisms of such internal communication are outside the scope of the IHE Technical Framework.
When multiple actors are grouped in a single product implementation, all transactions originating or terminating with each of the supported actors shall be supported (i.e., the IHE transactions shall be offered on an external product interface).
The following examples describe which actors typical systems might be expected to support. This is not intended to be a requirement, but rather to provide illustrative examples.
An acute care EMR serving a hospital might include a Document Source Actor, Document Consumer Actor, a Document Repository Actor, a Patient Identification Consumer Actor, as well as a Secured Node Actor. An Ambulatory EMR serving a physician practice might include a Document Source Actor, Document Consumer Actor, a Patient Demographics Client Actor, as well as a Secured Node Actor.
Cross-Enterprise Sharing of Medical Summaries (XDS-MS) Integration Profile
Scope and Purpose
Patient, clinician, industry and governmental demands for improved healthcare quality have created increased focus to make patient healthcare information interoperability across disparate systems a reality.
A solution for interoperability is, however, not a simple undertaking. Unstructured textual data forms remains the predominate mechanism for information exchange among health care providers, and a good majority of data needed by physicians and other health care providers to make good clinical decisions is embedded in this free text. Efficient and effective interoperability therefore begins by identifying the most relevant documents and the most relevant sections within those documents.
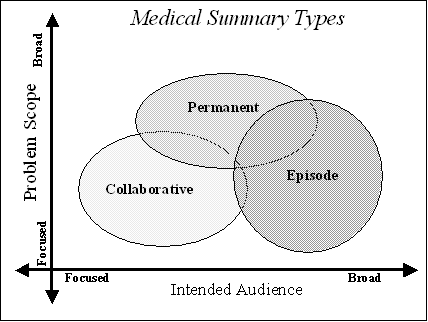
By their nature, Medical Summaries form a class of clinical documents that contain the most relevant portions of this information. As the name would indicate they have the purpose of summarizing, both abstracting the most important pieces of information from the EMR and recording free-text summaries at the time of medical summary creation. Operationally, they are commonly created at points in time of transfers of care from one provider to another or from one setting to another.
Patient transfers and, therefore, the summary documents that accompany these transfers can be categorized into 3 primary types: Episodic, Collaborative, or Permanent. These categories are important because they represent a breadth of use case scenarios for Medical Summaries. For example, summaries for collaborative transfers of care such as referral notes have a focused objective for providing the most relevant information about the patient intended for a specific provider. Collaborative summaries have a general audience that is generated as an artifact since they also provide the most relevant spot to obtain information about specific classes of patient problems that the patient has.
By contrast, episodic summaries have the primary purpose of highlighting the most relevant details of focused periods of time in a patient history. Examples include discharge summaries or history and physicals. Episodic summaries are written for a broad audience by intent.
Permanent transfers have yet a third purpose of summarizing the entirety of a patient's medical history and therefore covers a broader range of patient problems. The audience may be focused (as in a transfer to a new provider) or general (as in a discharge from the military).
The challenge is to identify the clinically relevant documents (and data elements those documents contain) that are used in typical "transfer of care" scenarios and then to provide interoperability standards to promote ease in transmission of those documents (and data elements). The Cross-Enterprise Sharing of Medical Summary (XDS-MS) Integration Profile facilitates this by defining the appropriate standards for document transmission and a minimum set of "record entries" that should be forwarded or made available to subsequent care provider(s) during specific transfer of care scenarios. In addition, this integration profile needs to define the utilization requirements/options for the receiving entity in order to ensure that the "care context" of the sending entity is appropriately maintained following the information transfer.
Process Flow
The basic process flow supported by XDS-MS mirrors current manual practices: someone gathers the appropriate documents from the patient medical record, copies them, packages them up with a cover letter explaining the reason the information is being sent, and then ships the package to the receiving provider. This is often accompanied by a telephone call from the sending provider to the receiving provider that indicates that such information is forthcoming.
Because the Collaborative care transfers and Episodic Care transfers differ significantly, these two use cases are defined. Users or implementers of this Integration Profile are offered options in the support of either of these two use cases. Permanent Care Summaries also differ significantly. However their use is less frequent; so this use case was deferred for future work.
Use Case 1: Ambulatory Specialist Referral
This use case involves a "collaborative" transfer of care for the referral of a patient from a primary care provider (PCP) to a specialist. This use case is a central component of an "e-referral" process, which typically requires an appropriate level of agreement/collaboration between the two parties prior to the actual transfer of clinical information being initiated.
The preconditions assume a PCP sees a patient in his office. The PCP has talked to the patient and performed an examination, and has decided to refer the patient to a specialist. An assumption is made that the PCP has an EMR system with capability to write notes and manage data elements. The specific data elements managed by the PCP's EMR are expected to be the source for the information used in creating the medical summary document related to this transfer of care. A variety of EMR implementations and usage by clinicians may result in some variability in the content of the medical summary.
The detailed content of the medical summary to support this use case will be detailed as part of the document content profile specification (See the Referral Summary Content Module below).
Steps to identify the specialist and obtain insurance preauthorization have been placed out of scope for this Integration Profile.
Post conditions include the specialist physician receiving the notification of referral, locating the documents (via the Document Registry), retrieving the Documents and viewing them and optionally importing data. Import assumes the specialist with an EMR system with the capability for managing those discrete data elements.
Use Case 2: Acute Care Discharge to Ambulatory Care Environment
This use case involves an episodic transfer of care in the form of a patient discharge from a hospital to home. The attending physician in the hospital generates a discharge summary document that is used by the hospital record keeping and billing abstraction. The attending physician in the hospital may or may not also be serving as the ambulatory PCP. If not, a copy of this record is sent to the PCP as well as other specialist providers that will have ambulatory follow-up care.
The events of the use case involve creation of the discharge summary, sharing it, and notifying other providers such as the PCP's office and the surgeon's office.
The post conditions include the receipt and viewing of the discharge summary with optional import into the ambulatory EMR system.
The detailed content of the medical summary to support this use case will be detailed as part of the document content profile specification (See the Discharge Summary Content Module below).
Content Interoperability Levels
The use cases described above imply different levels of interoperability. At the lowest level, a clinician simply needs to be able to access and view some content such as a medical summary. At this level, minimal structured data elements must be present – just enough metadata to verify that access to that document can be accessed appropriately associated with a visual representation of the document.
Beyond this simple metadata, nearly all medical summary documents have organizational elements that group the relevant parts of the medical summary. For humans this allows for more rapid review because it is easier to skip to portions of interest for care. Computers too can take advantage of this structuring. For example, it is relevant to see the list of discharge medications from a discharge summary in relation to current medications for comparison and reconciliation.
At a very high level of interoperability, the ability to pass fully structured and codified data is necessary for computer processing and mapping. For example, the ability to import medications identified in medical summaries from another institution could have tremendous potential for ensuring that medication orders are transferred correctly. Unfortunately, the cost for providing high levels of semantic interoperability is increased complexity of implementation, and therefore long implementation times.
The HL7 Clinical Document Architecture (CDA) standard and Care Record Summary (CRS) CDA implementation guides support progressive interoperability at multiple levels of complexity, from those needed to provide simple low level interoperability for supporting the most important use case of simple viewing to those providing a path to progressively higher levels of interoperability for vendors and providers wishing to implement it. CDA as constrained in the CRS implementation guides is therefore the base standard for the XDS-MS content profile.
The XDS-MS content profile builds on and further constrains the CDA-CRS implementation guide by defining the required and optional sections required for the Acute Care Discharge and Specialist Referral use cases. Additionally, it places constraints for the most important sections (Medication, Allergy and Problems) of Medical Summaries to ensure that structured field level data are provided.
The figure below shows how the XDS-MS Content profile defines these progressive levels of interoperability for sections of different importance. Header metadata must be present and coded. Most sections must define, at minimum, a section label to identify that section. For the Medication, Allergy, and Problems Sections, data must contain a more granular field level data as discrete text (for example dose or frequency). This is referred to as structured textual representation. Note that the textual strings in this structured text are not duplicates of the textual strings in the human readable text, but simply referenced extracts from the human readable text content, reducing the risk for inconsistencies
Granular field level data may then be optionally coded. If any coded terminology is used it shall be uniquely identified.

| Note: The lack of mature and broadly accepted standards for coded terminology requires that this integration profile not specify specific coded vocabularies. However, when agreements can be reached, the capability to exchange coded level information is possible. IHE has on its roadmap to continue working with appropriate standards bodies so that coded terminology standards can be added to this profile in the future. |
Use Case Conclusion
The process flow of this profile exhibits a great deal more power and flexibility than the existing manual process. The physician workflow is improved by reusing an existing work product in the very first step (the summary report) to accomplish two purposes: recording care that has been provided, and communicating with another provider.
Secondly, each step utilizes the power of inter-connected EMR systems to make the entire process faster, easier, and less reliant on human labor to accomplish the same feats. This results in reduced time to transfer records between providers, safer transport of the information, and more reliable receipt.
Lastly, the process facilitates the import of relevant data from one set of patient records to the receiving physicians EMR system, resulting in more reliable transfer of information, reduced labor costs transferring information from one provider to another and less time required by the patient to provide information that is already in the physician's possession.
Actors/Transaction
There are two actors in the XDS-MS profile, the Content Creator and the Content Consumer. Content is created by a Content Creator and is to be consumed by a Content Consumer. The sharing or transmission of content from one actor to the other is addressed by the appropriate use of IHE profiles described below, and is out of scope of this profile. A Document Source or a Portable Media Creator may embody the Content Creator Actor. A Document Consumer, a Document Recipient or a Portable Media Importer may embody the Content Consumer Actor. The sharing or transmission of content or updates from one actor to the other is addressed by the use of appropriate IHE profiles described in the section on Content Bindings with XDS, XDM and XDR.

Options
| Actor | Option |
|---|---|
| Content Consumer | View Option (1) |
| Document Import Option (1) | |
| Section Import Option (1) | |
| Discrete Data Import Option (1) | |
| Content Creator | Referral Option (1) |
| Discharge Summary Option (1) |
Content Consumer Options
View Option
This option defines the processing requirements placed on Content Consumers for providing access, rendering and management of the medical document. See the View Option in PCC TF-2 for more details on this option.
A Content Creator Actor should provide access to a style sheet that ensures consistent rendering of the medical document content as was displayed by the Content Consumer Actor.
The Content Consumer Actor shall be able to present a view of the document using this style sheet if present.
Document Import Option
This option defines the processing requirements placed on Content Consumers for providing access, and importing the entire medical document and managing it as part of the patient record. See the Document Import Option in PCC TF-2 for more details on this option.
Section Import Option
This option defines the processing requirements placed on Content Consumers for providing access to, and importing the selected section of the medical document and managing them as part of the patient record. See the Section Import Option in PCC TF-2 for more details on this option.
Discrete Data Import Option
This option defines the processing requirements placed on Content Consumers for providing access, and importing discrete data from selected sections of the medical document and managing them as part of the patient record. See the Discrete Data Import Option in PCC TF-2 for more details on this option.
Content Creator Options
Referral Option
Content Creators implementing this option shall create Referrals that comply with the Referral Content Module.
Discharge Summary Option
Content Creators implementing this option shall create Discharge Summaries that comply with the Discharge Summary Content Module.
Coded Terminologies
This profile supports the capability to record entries beyond the IHE required coding associated with structured data. Actors from this profile may choose to utilize coded data, but interoperability at this level requires an agreement between the communicating parties that is beyond the scope of this Profile.
To facilitate this level of interoperability, the applications that implement actors within this profile shall provide a link to their HL7 conformance profile within their IHE Integration statement. The conformance profile describes the structure of the information which they are capable of creating or consuming. The conformance profile shall state which templates are supported by the application implementing the profile Actors, and which vocabularies and/or data types are used within those templates. It should also indicate the optional components of the entry that are supported.
An Example HL7 Conformance Profile is available to show how to construct such a statement. See the HL7 Refinement Constraint and Localization for more details on HL7 conformance profiles.
Content Modules
Content modules describe the content of a payload found in an IHE transaction. Content profiles are transaction neutral. They do not have dependencies upon the transaction that they appear in. These dependencies are reflected in the Bindings listed above.
Referral Summary
All referral summaries shall be structured and coded as required by the Referral Summary Content Module described in PCC TF-2. The inclusion of the specific coded attributes explicitly defined as optional, may be supported by specific implementations of Document Sources using an IHE identified coded terminology of their choice. The requirements and manner in which implementations support such capabilities is beyond the scope of this Integration Profile.
Discharge Summary
All discharge summaries shall be structured and coded as required by the Discharge Summary Content Module described in PCC TF-2. The inclusion of the specific coded attributes explicitly defined as optional, may be supported by specific implementations of Document Sources using an IHE identified coded terminology of their choice. The requirements and manner in which implementations support such capabilities is beyond the scope of this Integration Profile.
Grouping with other Profile Actors
Content profiles may impose additional requirements on the transactions used when grouped with actors from other IHE Profiles.
Cross Enterprise Document Sharing, Media Interchange and Reliable Messages
Actors from the ITI XDS, XDM and XDR profiles embody the Content Creator and Content Consumer sharing function of this profile. A Content Creator or Content Consumer may be grouped with appropriate actors from the XDS, XDM or XDR profiles to exchange the content described therein. The metadata sent in the document sharing or interchange messages has specific relationships or dependencies (which we call bindings) to the content of the clinical document described in the content profile.
The Patient Care Coordination Technical Framework defines the bindings to use when grouping the Content Creator of this Profile with actors from the IHE ITI XDS, XDM or XDR Integration Profiles.
| Content | Binding | Actor | Optionality |
| Referral Summary | Medical Document Binding to XDS, XDM and XDR | Content Creator | O (Note 1) |
| Content Consumer | R | ||
| Discharge Summary | Medical Document Binding to XDS, XDM and XDR | Content Creator | O (Note 1) |
| Content Consumer | R |
Note 1: Content Creators must support generation of at least one type of content from this table with a transaction in order for the transaction to meet the requirements of the XDS-MS profile. Content Consumers must support both types of content to meet these requirements.
Notification of Document Availability (NAV)
When a Content Creator actor of the XDS-MS Integration Profile needs to notify other systems of documents, it may support the ITI Notification of Document Availability (NAV) Integration Profile. One of the Acknowledgement Request options may be used to request from a Document Consumer that an acknowledgement should be returned when it has received and processed the notification. When a Content Consumer wants to provide the capability to receive a Receive Notification Transaction it may support the Document Consumer Actor of the NAV Integration Profile. The Send Acknowledgement option may be used to issue a Send Acknowledgement to a Document Source that the notification was received and processed.
Document Digital Signature (DSG)
When a Content Creator Actor of the XDS-MS Integration Profile needs to digitally sign a medical summary or any other documents in a submission set, it may support the Digital Signature (DSG) Content Profile as a Document Source.
When a Content Consumer Actor of the XDS-MS Integration Profile needs to verify a Digital Signature, it may retrieve the digital signature document and may perform the verification against the signed document content.
Security Considerations
The XDS-MS Integration Profile assumes that a minimum security and privacy environment has been established across all participants. There must exist security policies regarding the use of training, agreements, risk management, business continuity and network security that need to be already in place prior to the implementation of XDS-MS.
The IHE ITI ATNA Integration Profile is required of the actors involved in the IHE transactions specified in this profile to protect node-to-node communication and to produce an audit trail of the PHI related actions when they exchange messages.
In addition, the IHE ITI DSG Integration Profiles can be applied to the actors involved in the transactions specified in this profile to securely identify individuals involved in transactions and verify document integrity and authorizations (DSG).
Interested parties should also read the detailed Security Considerations sections provided for each of the aforementioned profiles in the IHE ITI Technical Framework and its supplements.
The XDS-MS profile does have a few security considerations of its own.
EMR systems should be thoughtfully designed so that providers are able to review and verify information before it is imported into their EMR system, and that positive user acknowledgements are made before import, and audit trails are recorded when imports occur.
Imported information should be traceable both to the source [the sharing EMR], and the receiver that accepted it into the EMR system. XDS Affinity domain policies should support policies and procedures for tracing information flows between EMR systems.
Because the information being transferred is in XML, it will be common that different EMR systems utilize different transformations to render the contents into human readable form. A Content Creator should make available the transforms used by the sending provider to review the documents, and a Content Consumer must support rendering the information as seen by the sending provider, allowing both providers to see what was sent in its original rendered form.
Requirements of XDS-MS Actors
This section describes the specific requirements for each Actor defined within this profile. Specific details can be found in Volume 1 and Volume 2 of the technical framework.
Content Creator
- A Content Creator shall be able to create either a Referral Summary or a Discharge Summary, or both, according to the specifications for these content profiles found in PCC TF-2.
- A Content Creator shall be grouped with the Time Client Actor, and shall synchronize its clock with a Time Server.
- A Content Creator shall be grouped with the Secure Node or Secure Application Actor of the ATNA profile.
- All activity initiated by the application implementing the Content Creator shall generate the appropriate audit trail messages as specified by the ATNA Profile. The bare minimum requirements of a Content Creator are that it be able to log creation and export of clinical content.
- A Content Creator shall use secure communications for any document exchanges, according to the specifications of the ATNA profile.
Content Consumer
- A Content Consumer shall be able to consume a Referral Summary and a Discharge Summary.
- A Content Consumer shall implement the View Option or Discrete Data import option, or both.
- A Content Consumer that implements the Document Import or Section Import Option shall implement the View Option as well.
- A Content Consumer that implements the View option shall be able to:
- Demonstrate rendering of the document for display.
- Print the document.
- Display the document with its original stylesheet.
- Support traversal of any links contained within the document.
- A Content Consumer that implements the Document Import Option shall:
- Store the document.
- Demonstrate the ability to access the document again from local storage.
- A Content Consumer that implements the Section Import Option shall offer a means to import one or more document sections into the patient record as free text.
- A Content Consumer that implements the Discrete Data Import Option shall offer a means to import structured data from one or more sections of the document.
- A Content Consumer Actor shall be grouped with the Time Client Actor, and shall synchronize its clock with a Time Server.
- All activity initiated by the application implementing the Content Consumer shall generate the appropriate audit trail messages as specified by the ATNA Profile. The bare minimum requirements of a Content Consumer are that it be able to log views or imports of clinical content.
- A Content Consumer shall log events for any views of stored clinical content.
- A Content Consumer shall use secure communications for any document exchanges, according to the specifications of the ATNA profile.
Exchange of Personal Health Record Content Integration Profile (XPHR)
The Exchange of Personal Health Record Content (XPHR) integration profile describes the content and format of summary information extracted from a PHR system used by a patient for import into healthcare provider information systems, and visa versa. The purpose of this profile is to support interoperability between PHR systems used by patients and the information systems used by healthcare providers. This profile does not address all the data exchange requirements of PHR systems. A PHR system may leverage other IHE Integration and Content Profiles for interoperability in addition to the XPHR Content Profile. For example, a PHR Systems may implement XDS-MS to import medical summaries produced by EHR systems, XDS-I to import imaging information, XDS-Lab to import laboratory reports, et cetera.
Exchange of Personal Health Record Content (XPHR)
Upon seeing a healthcare provider for the first time, patients are requested to provide a great deal of information, including, their address, telephone numbers, birth date, sex, marital status, emergency contacts, insurance information, a medical and family history, and current medications and allergies. This information is also reviewed and updated on subsequent visits. This information is usually obtained by having the patient fill out one or more forms, whose contents are then manually transferred in to the information systems used by the healthcare provider. Automating this process will reduce transcription errors during the transfer of information, speed up the registration and check-in processes for patients, and also makes it possible for patients to have more participation in the management of their health information.
Providers also need to participate in helping patients to manage their healthcare information, however, providers should not be solely responsible for updating the patient's health record, since they often are only participating in a portion of the patient's overall health activities.
PHR systems allow patients to manage their healthcare information. EHR and other information systems allow healthcare providers to manage the electronic records they maintain for their patients. These two systems, operating separately, are not sufficient to allow patients and providers to collaborate in the care of the patient. What is needed is a way to integrate the activities of patients using a PHR system and healthcare providers using an EHR or other information system to provide for collaborative care between the patient and their provider.
The XPHR profile is intended to provide a mechanism for patients to supply the information most often requested by their healthcare providers, and to allow those same providers to assist patients in keeping their personal healthcare information up to date. It achieves this by allowing patients to provide a summary of their PHR information to providers, and gives providers a mechanism to suggest updates to the patient's PHR upon completion of a healthcare encounter.
Actors/Transaction
There are two actors in the XPHR profile, the Content Creator and the Content Consumer. Content is created by a Content Creator and is to be consumed by a Content Consumer. The sharing or transmission of content from one actor to the other is addressed by the appropriate use of IHE profiles described below, and is out of scope of this profile. A Document Source or a Portable Media Creator may embody the Content Creator Actor. A Document Consumer, a Document Recipient or a Portable Media Importer may embody the Content Consumer Actor. The sharing or transmission of content or updates from one actor to the other is addressed by the use of appropriate IHE profiles described in the section on Content Bindings with XDS, XDM and XDR.

Options
| Actor | Option |
|---|---|
| Content Consumer | View Option (1) |
| Document Import Option (1) | |
| Section Import Option (1) | |
| Discrete Data Import Option (1) | |
| Content Creator | Update Option |
Content Consumer Options
View Option
This option defines the processing requirements placed on Content Consumers for providing access, rendering and management of the medical document. See the View Option in PCC TF-2 for more details on this option.
A Content Creator Actor should provide access to a style sheet that ensures consistent rendering of the medical document content as was displayed by the Content Consumer Actor.
The Content Consumer Actor shall be able to present a view of the document using this style sheet if present.
Document Import Option
This option defines the processing requirements placed on Content Consumers for providing access, and importing the entire medical document and managing it as part of the patient record. See the Document Import Option in PCC TF-2 for more details on this option.
Section Import Option
This option defines the processing requirements placed on Content Consumers for providing access to, and importing the selected section of the medical document and managing them as part of the patient record. See the Section Import Option in PCC TF-2 for more details on this option.
Discrete Data Import Option
This option defines the processing requirements placed on Content Consumers for providing access, and importing discrete data from selected sections of the medical document and managing them as part of the patient record. See the Discrete Data Import Option in PCC TF-2 for more details on this option.
Content Creator Options
Update Option
Content Creators supporting the update option shall create be able to create a PHR Update Module Content document structured and coded as required by the PHR Update Module Content found in PCC TF-2.
Coded Terminologies
This profile supports the capability to record entries beyond the IHE required coding associated with structured data. Actors from this profile may choose to utilize coded data, but interoperability at this level requires an agreement between the communicating parties that is beyond the scope of this Profile.
To facilitate this level of interoperability, the applications that implement actors within this profile shall provide a link to their HL7 conformance profile within their IHE Integration statement. The conformance profile describes the structure of the information which they are capable of creating or consuming. The conformance profile shall state which templates are supported by the application implementing the profile Actors, and which vocabularies and/or data types are used within those templates. It should also indicate the optional components of the entry that are supported.
An Example HL7 Conformance Profile is available to show how to construct such a statement. See the HL7 Refinement Constraint and Localization for more details on HL7 conformance profiles.
XPHR Content Modules
PHR Extract Module
The content exchanged shall be structured and coded as required by the PHR Extract Module Content. The Content Creator Actor creates a PHR Extract and shares it with the Content Consumer.
PHR Update Module
The content exchanged shall be structured and coded as required by the PHR Update Module Content. The Content Creator Actor creates a PHR Update document as an addendum to a previously exchanged PHR Extract document. This Update is an addendum to the prior document, and reflects changes to that document that are suggested by the Content Creator Actor. A Content Consumer actor shall support viewing of an Update document, and may support import of the Update to reflect those changes to the PHR.
The purpose of this content module is to provide a mechanism whereby healthcare providers, using applications that implement the Content Creator Actor, can suggest updates to a PHR for a patient.
XPHR Integration Profile Process Flow
One key use scenario has been identified as an example. This use case originated with the Cross-Enterprise Document Sharing on Media (XDM) profile, and is reproduced here.
Personal Health Record (PHR) to ED/Primary Care EHR
Precondition: A patient is using a Personal Health Record application system at home for the record keeping of patient-originated medical information (e.g. social history, family history), snapshots of clinical information that may have been provided from previous care encounters (e.g. medication list, immunization records, etc), and current observations from home care medical devices (e.g. blood pressure, blood sugar level, etc).
Events: The patient requests their provider give them initial information to initialize their new PHR system. Later the patient does an extract of his PHR onto a portable media (USB key, CD) to bring to the care facility as a current set of medical data for the clinician. The patient experiences a medical condition requiring that he needs to present at the ED or his PCP for care. The ED physician or primary care physician receives the portable media from the patient and loads it an office PC to display and/or import, as desired, the information provided on the portable media. Following the encounter, the provider does an extract of appropriate data elements from the office EMR to yield a snapshot of the patient's medical record. This snapshot is then transferred to an interchange media for the patient to bring home and update his private PHR. The patient imports this document and uses the information in it to update the content of their PHR: e.g., by applying the changes recorded in the PHR Update appropriately .
Postcondition: The patient's PHR is up to date.

Grouping with Other Actors
Cross Enterprise Document Sharing, Media Interchange and Reliable Messages
Actors from the ITI XDS, XDM and XDR profiles embody the Content Creator and Content Consumer sharing function of this profile. A Content Creator or Content Consumer may be grouped with appropriate actors from the XDS, XDM or XDR profiles to exchange the content described therein. The metadata sent in the document sharing or interchange messages has specific relationships or dependencies (which we call bindings) to the content of the clinical document described in the content profile.
The Patient Care Coordination Technical Framework defines the bindings to use when grouping the Content Creator of this Profile with actors from the IHE ITI XDS, XDM or XDR Integration Profiles.
| Content | Binding | Actor | Optionality |
| PHR Extract | Medical Document Binding to XDS, XDM and XDR | Content Creator | R |
| Content Consumer | R | ||
| PHR Update | Medical Document Binding to XDS, XDM and XDR | Content Creator | O |
| Content Consumer | R |
Document Digital Signature (DSG)
Content Creator actors should digitally sign all documents using the Digital Signature (DSG) Content Profile.
Content Consumer actors should verify the Digital Signature of the submission set before use of the information it contains.
Requirements of XPHR Actors
This section describes the specific requirements for each Actor defined within this profile. Specific details can be found in Volume 1 and Volume 2 of the technical framework.
Content Creator
- A Content Creator shall be able to create a PHR Extract according to the specification for that content profile found in PCC TF-2.
- A Content Creator implementing the Update option shall be able to create a PHR Update according to the specification for that content profile found in PCC TF-2.
- A Content Creator shall be grouped with the Time Client Actor, and shall synchronize its clock with a Time Server.
- A Content Creator shall be grouped with the Secure Node or Secure Application Actor of the ATNA profile.
- All activity initiated by the application implementing the Content Creator shall generate the appropriate audit trail messages as specified by the ATNA Profile. The bare minimum requirements of a Content Creator are that it be able to log creation and export of clinical content.
- A Content Creator shall use secure communications for any document exchanges, according to the specifications of the ATNA profile.
Content Consumer
- A Content Consumer shall be able to consume a PHR Extract and a PHR Update.
- A Content Consumer shall implement the View Option or Discrete Data import option, or both.
- A Content Consumer that implements the Document Import or Section Import Option shall implement the View Option as well.
- A Content Consumer that implements the View option shall be able to:
- Demonstrate rendering of the document for display.
- Print the document.
- Display the document with its original stylesheet.
- Support traversal of any links contained within the document.
- A Content Consumer that implements the Document Import Option shall:
- Store the document.
- Demonstrate the ability to access the document again from local storage.
- A Content Consumer that implements the Section Import Option shall offer a means to import one or more document sections into the patient record as free text.
- A Content Consumer that implements the Discrete Data Import Option shall offer a means to import structured data from one or more sections of the document.
- A Content Consumer Actor shall be grouped with the Time Client Actor, and shall synchronize its clock with a Time Server.
- All activity initiated by the application implementing the Content Consumer shall generate the appropriate audit trail messages as specified by the ATNA Profile. The bare minimum requirements of a Content Consumer are that it be able to log views or imports of clinical content.
- A Content Consumer shall log events for any views of stored clinical content.
- A Content Consumer shall use secure communications for any document exchanges, according to the specifications of the ATNA profile.
Basic Patient Privacy Consents (BPPC) Integration Profile
The Basic Patient Privacy Consents Integration profile was transferred to the IT Infrastructure Domain in the Summer of 2007. This profile will be released as a supplement to the IT Infrastructure Technical Framework in August of 2007, and can be found here http://www.ihe.net/Technical_Framework/index.cfm#IT
For discussion see Basic Patient Privacy Consents
Volume 1
HIMSS and RSNA
Integrating the Healthcare Enterprise
IHE Patient Care Coordination
Emergency Department Referral (EDR)
Technical Framework Supplement
Volume I
Revision 3.0
2008-2009
Public Comment
- (PCC TF-1/Preface)Preface to Volume I of the PCC Technical Framework
- (PCC TF-1/Introduction)Introduction to the PCC Technical Framework
- (PCC TF-1/About)About the Patient Care Coordination Integration Profiles
- (PCC TF-1/Dependencies)Dependencies of the PCC Integration Profiles
- (PCC TF-1/Overview)PCC Integration Profiles Overview
- (PCC TF-1/History)History of Annual Changes
- (PCC TF-1/Product Implementations)Product Implementations
Emergency Department Referral (EDR) Integration Profile
Physicians frequently determine that patients either onsite, or calling in, should proceed directly to an emergency department for care. The referring physician has valuable data that can inform ED providers, including the history of the current problem, past medical problems, medications, allergies, and frequently a concrete assessment and plan for the patient such as hospital admission. Unfortunately, this information is inconsistently relayed to the ED provider who ultimately cares for the patient. Currently, this transfer of care requires verbal transfer of extensive information. Unfortunately, the ED provider recording the information may not be the person who will ultimately care for the patient, may not document sufficient detail, or may forget to document any information at all.
Loss of this data can lead to costly over-testing in the ED, or worse, an inappropriate disposition for the patient.
Using an EHR, an ED Referral is created; including the nature of the current problem, past medical history, and medications. Upon arrival of the patient to the ED, the patient is identified as a referral, and the transfer document is incorporated into the EDIS.
This profile may be used to cover a wide variety of ED referral situations, for example, primary care provider to ED Referral, Long term care to ED referral, or even ED to ED referral (as in the case of transfer from a level 2 Critical care facility to a level 1 facility).
Actors/Transaction
There are two actors in the EDR profile, the Content Creator and the Content Consumer. Content is created by a Content Creator and is to be consumed by a Content Consumer. The sharing or transmission of content from one actor to the other is addressed by the appropriate use of IHE profiles described below, and is out of scope of this profile. A Document Source or a Portable Media Creator may embody the Content Creator Actor. A Document Consumer, a Document Recipient or a Portable Media Importer may embody the Content Consumer Actor. The sharing or transmission of content or updates from one actor to the other is addressed by the use of appropriate IHE profiles described in the section on Content Bindings with XDS, XDM and XDR.

Options
| Actor | Option |
|---|---|
| Content Consumer | View Option (1) |
| Document Import Option (1) | |
| Section Import Option (1) | |
| Discrete Data Import Option (1) |
Content Consumer Options
View Option
This option defines the processing requirements placed on Content Consumers for providing access, rendering and management of the medical document. See the View Option in PCC TF-2 for more details on this option.
A Content Creator Actor should provide access to a style sheet that ensures consistent rendering of the medical document content as was displayed by the Content Consumer Actor.
The Content Consumer Actor shall be able to present a view of the document using this style sheet if present.
Document Import Option
This option defines the processing requirements placed on Content Consumers for providing access, and importing the entire medical document and managing it as part of the patient record. See the Document Import Option in PCC TF-2 for more details on this option.
Section Import Option
This option defines the processing requirements placed on Content Consumers for providing access to, and importing the selected section of the medical document and managing them as part of the patient record. See the Section Import Option in PCC TF-2 for more details on this option.
Discrete Data Import Option
This option defines the processing requirements placed on Content Consumers for providing access, and importing discrete data from selected sections of the medical document and managing them as part of the patient record. See the Discrete Data Import Option in PCC TF-2 for more details on this option.
Coded Terminologies
This profile supports the capability to record entries beyond the IHE required coding associated with structured data. Actors from this profile may choose to utilize coded data, but interoperability at this level requires an agreement between the communicating parties that is beyond the scope of this Profile.
To facilitate this level of interoperability, the applications that implement actors within this profile shall provide a link to their HL7 conformance profile within their IHE Integration statement. The conformance profile describes the structure of the information which they are capable of creating or consuming. The conformance profile shall state which templates are supported by the application implementing the profile Actors, and which vocabularies and/or data types are used within those templates. It should also indicate the optional components of the entry that are supported.
An Example HL7 Conformance Profile is available to show how to construct such a statement. See the HL7 Refinement Constraint and Localization for more details on HL7 conformance profiles.
ED Referral Document Content Module
An ED Referral content document is a type of referral summary, and incorporates the constraints defined for referral summaries found in Referral Summary. In addition, the ED Referral content profile includes additional information to support recording the mode of transportation, estimated time of arrival, and proposed disposition.
ED Referral Process Flow
Use Case 1: Provider to Emergency Department Referral
This use case involves a "collaborative" transfer of care for the referral of a patient from a care provider to the emergency department. This use case is a central component of an "e-referral" process, which typically requires an appropriate level of agreement and collaboration between the two parties prior to the actual transfer of clinical information being initiated.
Preconditions: The referring provider has an EMR system with capability to write notes and manage data elements, and share information. The specific data elements managed by the providers EMR are expected to be the source for the information used in creating the medical summary document related to this transfer of care. A variety of EMR implementations and usage by clinicians may result in some variability in the content of the medical summary. The receiving ED provider has an EDIS system with the capability to share information.
Events: A provider sees a patient, or has spoken with the patient or a family member, and has decided to refer the patient to an ED. The provider creates an ED Referral summary document, and shares it. The detailed content of the medical summary to support this use case is detailed as part of the document content profile specification.
Post conditions: The ED specialist physician retrieve the Documents and views them, optionally importing data. Import assumes the specialist has an EDIS system with the capability for managing those discrete data elements.
Steps to identify the ED and obtain insurance preauthorization have been placed out of scope for this Integration Profile.
Grouping with other Profiles
Cross Enterprise Document Sharing, Media Interchange and Reliable Messages
Actors from the ITI XDS, XDM and XDR profiles embody the Content Creator and Content Consumer sharing function of this profile. A Content Creator or Content Consumer may be grouped with appropriate actors from the XDS, XDM or XDR profiles to exchange the content described therein. The metadata sent in the document sharing or interchange messages has specific relationships or dependencies (which we call bindings) to the content of the clinical document described in the content profile.
The Patient Care Coordination Technical Framework defines the bindings to use when grouping the Content Creator of this Profile with actors from the IHE ITI XDS, XDM or XDR Integration Profiles.
| Content | Binding | Actor | Optionality |
| ED Referral | Medical Document Binding to XDS, XDM and XDR | Content Creator | R |
| Content Consumer | R |
Requirements of EDR Actors
This section describes the specific requirements for each Actor defined within this profile. Specific details can be found in Volume 1 and Volume 2 of the technical framework.
Content Creator
- A Content Creator shall be able to create an ED Referral according to the specification for that content profile found in PCC TF-2.
- A Content Creator shall be grouped with the Time Client Actor, and shall synchronize its clock with a Time Server.
- A Content Creator shall be grouped with the Secure Node or Secure Application Actor of the ATNA profile.
- All activity initiated by the application implementing the Content Creator shall generate the appropriate audit trail messages as specified by the ATNA Profile. The bare minimum requirements of a Content Creator are that it be able to log creation and export of clinical content.
- A Content Creator shall use secure communications for any document exchanges, according to the specifications of the ATNA profile.
Content Consumer
- A Content Consumer shall implement the View Option or Discrete Data import option, or both.
- A Content Consumer that implements the Document Import or Section Import Option shall implement the View Option as well.
- A Content Consumer that implements the View option shall be able to:
- Demonstrate rendering of the document for display.
- Print the document.
- Display the document with its original stylesheet.
- Support traversal of any links contained within the document.
- A Content Consumer that implements the Document Import Option shall:
- Store the document.
- Demonstrate the ability to access the document again from local storage.
- A Content Consumer that implements the Section Import Option shall offer a means to import one or more document sections into the patient record as free text.
- A Content Consumer that implements the Discrete Data Import Option shall offer a means to import structured data from one or more sections of the document.
- A Content Consumer Actor shall be grouped with the Time Client Actor, and shall synchronize its clock with a Time Server.
- All activity initiated by the application implementing the Content Consumer shall generate the appropriate audit trail messages as specified by the ATNA Profile. The bare minimum requirements of a Content Consumer are that it be able to log views or imports of clinical content.
- A Content Consumer shall log events for any views of stored clinical content.
- A Content Consumer shall use secure communications for any document exchanges, according to the specifications of the ATNA profile.
Preprocedure History and Physical Integration Profile (PPHP)
The PPHP Profile is not being released for trial implementation. Components of this profile have been incorporated into the technical framework for use with other content profiles, and these remain in Volume II. It is expected that this profile will be withdrawn from the next revision of the final text.
Appendix A - Actor Descriptions
Actors are information systems or components of information systems that produce, manage, or act on information associated with operational activities in the enterprise.
- Content Creator
- The Content Creator Actor is responsible for the creation of content and transmission to a Content Consumer.
- Content Consumer
- A Content Consumer Actor is responsible for viewing, import, or other processing of content created by a Content Creator Actor.
Appendix B - Transaction Descriptions
Transactions are interactions between actors that transfer the required information through standards-based messages. The PCC Technical Framework does not define any specific transactions, as these are assumed to be carried out through the use of transactions defined in other IHE Profiles.
Appendix C - How to Prepare an IHE Integration Statement
IHE Integration Statements are documents prepared and published by vendors to describe the conformance of their products with the IHE Technical Framework. They identify the specific IHE capabilities a given product supports in terms of IHE actors and integration profiles described in the technical frameworks of each domain.
Users familiar with these concepts can use Integration Statements to determine what level of integration a vendor asserts a product supports with complementary systems and what clinical and operational benefits such integration might provide. Integration Statements are intended to be used in conjunction with statements of conformance to specific standards (e.g., HL7, IETF, DICOM, W3C, etc.).
IHE provides a process for vendors to test their implementations of IHE actors and integration profiles. The IHE testing process, culminating in a multi-party interactive testing event called the Connectathon, provides vendors with valuable feedback and provides a baseline indication of the conformance of their implementations. The process is not intended to independently evaluate, or ensure, product compliance. In publishing the results of the Connectathon and facilitating access to vendors' IHE Integration Statements, IHE and its sponsoring organizations are in no way attesting to the accuracy or validity of any vendor's IHE Integration Statements or any other claims by vendors regarding their products.
IMPORTANT -- PLEASE NOTE: Vendors have sole responsibility for the accuracy and validity of their IHE Integration Statements. Vendors' Integration Statements are made available through IHE simply for consideration by parties seeking information about the integration capabilities of particular products. IHE and its sponsoring organizations have not evaluated or approved any IHE Integration Statement or any related product, and IHE and its sponsoring organizations shall have no liability or responsibility to any party for any claims or damages, whether direct, indirect, incidental or consequential, including but not limited to business interruption and loss of revenue, arising from any use of, or reliance upon, any IHE Integration Statement.
Structure and Content of an IHE Integration Statement
An IHE Integration Statement for a product shall include:
- The Vendor Name
- The Product Name (as used in the commercial context) to which the IHE Integration Statement applies.
- The Product Version to which the IHE Integration Statement applies.
- A publication date and optionally a revision designation for the IHE Integration Statement.
- The following statement: "This product implements all transactions required in the IHE Technical Framework to support the IHE Integration Profiles, Actors and Options listed below:"
- A list of IHE Integration Profiles supported by the product and, for each Integration Profile, a list of IHE Actors supported. For each integration profile/actor combination, one or more of the options defined in the IHE Technical Framework may also be stated. Profiles, Actors and Options shall use the names defined by the IHE Technical Framework Volume I. (Note: The vendor may also elect to indicate the version number of the Technical Framework referenced for each Integration Profile.)
Note that implementation of the integration profile implies implementation of all required transactions for an actor as well as selected options.
The statement shall also include references and/or internet links to the following information:
- Specific internet address (or universal resource locator [URL]) where the vendor's Integration Statements are posted
- URL where the vendor's standards conformance statements (e.g., HL7, DICOM, etc.) relevant to the IHE transactions implemented by the product are posted.
- URL of the IHE Initiative's web page for general IHE information www.himss.org/ihe.
An IHE Integration Statement is not intended to promote or advertise aspects of a product not directly related to its implementation of IHE capabilities.
Format of an IHE Integration Statement
Each Integration Statement shall follow the format shown below. Vendors may add a cover page and any necessary additional information in accordance with their product documentation policies.
| IHE Integration Statement | Date | 12 Oct 2005 |
| Vendor | Product Name | Version |
| Any Medical Systems Co. | IntegrateRecord | V2.3 |
| This product implements all transactions required in the IHE Technical Framework to support the IHE Integration Profiles, Actors and Options listed below: | ||
| Integration Profiles Implemented | Actors Implemented | Options Implemented |
| Cross-Enterprise Sharing of Medical Summaries | Document Consumer | View Option |
| Audit Trail and Node Authentication | Secure Node | none |
| Patient Identity Cross-referencing | Patient Identifier Cross-reference Consumer | PIX Update Notification |
| Internet address for vendor's IHE information:www.anymedicalsystemsco.com/ihe | ||
| Links to Standards Conformance Statements for the Implementation | ||
| HL7 | www.anymedicalsystemsco.com/hl7 | |
| Links to general information on IHE | ||
| In North America: www.ihe.het | In Europe: www.ihe-europe.org | In Japan: www.jira-net.or.jp/ihe-j |
IHE Integration Statement template
An IHE Integration Statement template (MS Word version) is available here.
The IHE Product Registry
The assumption of an integration statement is that all actors listed are functionally grouped and conform to any profile specifications for such groupings. In case of exceptions the vendor must explicitly describe the functional groupings.
IHE has developed a new Web-based database of Integration Statements. The IHE Product Registry enables developers to create, manage and publish Integration Statements for their commercial and open source healthcare IT systems. It allows users to browse for these systems based on their conformance with specific IHE Actors and Profiles. The system is open for use by developers and users now!
Glossary
The following terms are used in various places within this technical framework, and are defined below. The complete IHE Glossary is available on the IHE Wiki at http://wiki.ihe.net/index.php/IHE_Glossary .
- Actor
- An entity within a use case diagram that can perform an action within a use case diagram. Possible actions are creation or consumption of a message
- ADT
- Admit, Discharge & Transfer.
- Affinity Domain Policy
- Affinity Domain Policy that clearly defines the appropriate uses of the XDS Affinity Domain. Within this policy is a defined set of acceptable use Privacy Consent Policies that are published and understood.
- ASTM
- Formerly the American Society of Testing and Materials, now ASTM International. An SDO that develops a number of standards across a wide variety of industries, including healthcare.
- ATNA
- Audit Trail and Node Authentication. An IHE ITI profile.
- Care Context
The participations surrounding the care provision act, and the attributes of that act. Everything in the document header. Data history, links to clinical reasoning.
- CDA
- Clinical Document Architecture. An HL7 standard for the exchange for clinical documents.
- Content Binding
- A content binding describe how the payload used in an IHE transaction is related to and/or constrained by the data elements contained within the content sent or received in those transactions.
- CRS
- Care Record Summary. An implementation guide that constrains CDA Release 2 for Care Record Summary documents.
- CT
- Consistent Time Integration Profile.
- DICOM
- Digital Imaging and Communication in Medicine
- DSG
- Digital Signatures. An IHE ITI Profile.
- EDIS
- Emergency Department Information System.
- eMPI
- Enterprise Master Patient Index.
- EMR
- Electronic Medical Record, an Electronic Health Record system used within an enterprise to deliver care (also called EHR-CR by IHE-XDS).
- Estimated Time of Arrival
- the time the patient being referred can be expected to arrive in the emergency department.
- EUA
- Enterprise User Authentication Integration Profile.
- Expected Actions
- Actions which should occur as the result of a trigger event.
- Functional Role
- Role an individual is acting under when they are executing a function. See ISO 21298
- HIMSS
- Healthcare Information and Management Systems Society.
- HL7
- Health Level Seven
- HIS
- Hospital Information System.
- IHE
- Integrating the Healthcare Enterprise.
- Interaction Diagram
- A diagram that depicts data flow and sequencing of events.
- IT
- Information Technology.
- MPI
- Master Patient Index.
- MRN
- Medical Record Number.
- NAV
- Notification of Document Availability
- OID
- Object Identifier. (See also 'Globally Unique Identifier').
- Patient Privacy Consent
- The act of a patient consenting to a specific Privacy Consent Policy.
- Patient Privacy Consent Document
- A document that follows the BPPC profile and captures the act of the patient consenting to a specific XDS Affinity Domain defined Privacy Consent Policy.
- Patient Identifier Cross-reference Domain
- Consists of a set of Patient Identifier Domains known and managed by a Patient Identifier Cross-reference Manager Actor. The Patient Identifier Cross-reference Manager Actor is responsible for providing lists of "alias" identifiers from different Patient Identifier Domains.
- Patient Identifier Domain
- A single system or a set of interconnected systems that all share a common identification scheme for patients. Such a scheme includes: (1) a single identifier-issuing authority, (2) an assignment process of an identifier to a patient, (3) a permanent record of issued patient identifiers with associated traits, and (4) a maintenance process over time. The goal of Patient Identification is to reduce errors.
- Portable Document Format.
- PIX
- Patient Identifier Cross Referencing. An IHE ITI Profile.
- PDQ
- Patient Demographics Query. An IHE ITI Profile.
- PHR
- Personal Health Record
- Privacy Consent Policy
- One of the acceptable-use Privacy Consent Policies that are agreed to and understood in the Affinity Domain.
- Privacy Consent Policy Act Identifier
- An Affinity Domain assigned identifier that uniquely defines the act of a patient consenting to a specific Affinity Domain: Privacy Consent Policy.
- Privacy Consent Policy Identifier
- An Affinity Domain assigned identifier (OID) that uniquely identifies the Affinity Domain: Privacy Consent Policy. There is one unique identifier (OID) for each Privacy Consent Policy within the Affinity Domain.
- Procedure
- In the context of a "Pre-procedure History and Physical," the "procedure" is a surgery or an invasive examination of a patient that is required by quality review organizations to be preceded by a pre-procedure assessment of procedure risk and anesthesia risk. This assessment is typically referred to as a "Pre-operative" or "Pre-procedure History and Physical."
- Process Flow Diagram
- A graphical illustration of the flow of processes and interactions among the actors involved in a particular example.
- Proposed disposition
- the intended disposition (i.e. admission to ICU, discharge to home, transfer to psychiatric hospital), if known, that the referring provider expects the patient will end up after the emergency department intervention.
- Role
- The actions of an actor in a use case.
- RSNA
- Radiological Society of North America.
- sig.
- A Latin abbreviation for signetur used to represent the instruction following the medication name.
- Scope
- A brief description of the transaction.
- Structural Role
- Role of an individual within an organization. See ISO 21298
- Transport Mode
- the method the patient employs, or is provided to get to the emergency department.
- Trigger Event
- An event such as the reception of a message or completion of a process, which causes another action to occur.
- UID
- Unique Identifier (See also Globally Unique Identifier).
- Universal ID
- Unique identifier over time within the UID type. Each UID must belong to one of specifically enumerated species. Universal ID must follow syntactic rules of its scheme.
- Use Case
- A graphical depiction of the actors and operation of a system.
- Wet Signature
- Ink on paper signature.
- XUA
- Cross Enterprise User Authentication
- XDS
- Cross Enterprise Document Sharing
Volume 2
HIMSS and RSNA
Integrating the Healthcare Enterprise
IHE Patient Care Coordination
Technical Framework
Volumes II
Revision 2.0
2006-2007
Draft
Preface to Volume 2
Intended Audience
The intended audience of this document is:
- Technical staff of vendors planning to participate in the IHE initiative
- IT departments of healthcare institutions
- Experts involved in standards development
- Anyone interested in the technical aspects of integrating healthcare information systems
Related Information for the Reader
The reader of volume 2 should read or be familiar with the following documents:
- Volume 1 of the Cross-Enterprise Document Sharing (XDS) Integration Profile documented in the ITI Infrastructure Technical Framework
(See http://www.ihe.net/Technical_Framework/index.cfm ). - Volume 1 of the Notification of Document Availability (NAV) Integration Profile documented in the ITI Infrastructure Technical Framework
(See http://www.ihe.net/Technical_Framework/index.cfm ). - Volume 1 of the Audit Trail and Node Authentication (ATNA) Integration Profile documented in the ITI Infrastructure Technical Framework
(See http://www.ihe.net/Technical_Framework/index.cfm ). - HL7 Clinical Document Architecture Release 2: Section 1, CDA Overview.
- Care Record Summary – Implementation Guide for CDA Release 2 (US Realm): Section 1
- Presentations from IHE Workshop: Effective Integration of the Enterprise and the Health System - June 28–29, 2005: http://www.ihe.net/Participation/workshop_2005.cfm, June 2005:
- for a RHIO-3.ppt Leveraging IHE to Build RHIO Interoperability
- Cross-Enterprise Document Sharing (XDS)
- Notification of Document Availability (NAV)
- Educ.ppt Patient Care Coordination
- Use Cases for Medical Summaries
- Ovrw.ppt Patient Care Coordination - Overview of Profiles
How this Document is Organized
Section 1 is the preface, describing the intended audience, related resources, and organizations and conventions used within this document.
Section 2 provides an overview of the concepts of IHE actors and transactions used in IHE to define the functional components of a distributed healthcare environment.
Section 3 defines transactions in detail, specifying the roles for each actor, the standards employed, the information exchanged, and in some cases, implementation options for the transaction.
Section 4 defines a set of payload bindings with transactions.
Section 5 defines the content modules that may be used in transactions.
Conventions Used in this Volume
This document has adopted the following conventions for representing the framework concepts and specifying how the standards upon which the IHE Technical Framework is based should be applied.
The Generic IHE Transaction Model
Transaction descriptions are provided in section 4. In each transaction description, the actors, the roles they play, and the transactions between them are presented as use cases.
The generic IHE transaction description includes the following components:
- Scope: a brief description of the transaction.
- Use case roles: textual definitions of the actors and their roles, with a simple diagram relating them, e.g.:
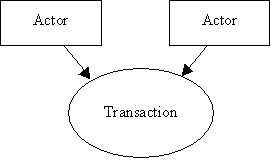
- Referenced Standards: the standards (stating the specific parts, chapters or sections thereof) to be used for the transaction.
- Interaction Diagram: a graphical depiction of the actors and transactions, with related processing within an actor shown as a rectangle and time progressing downward, similar to:
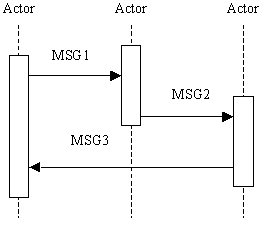
The interaction diagrams used in the IHE Technical Framework are modeled after those described in Grady Booch, James Rumbaugh, and Ivar Jacobson, The Unified Modeling Language User Guide, ISBN 0-201-57168-4. Simple acknowledgment messages are omitted from the diagrams for brevity.
- Message definitions: descriptions of each message involved in the transaction, the events that trigger the message, its semantics, and the actions that the message triggers in the receiver.
Copyright Permissions
Health Level Seven, Inc., has granted permission to the IHE to reproduce tables from the HL7 standard. The HL7 tables in this document are copyrighted by Health Level Seven, Inc. All rights reserved.
Material drawn from these documents is credited where used.
How to Contact Us
IHE Sponsors welcome comments on this document and the IHE initiative. They should be directed to the discussion server at http://forums.rsna.org or to:
Didi Davis
Director of Integrating the Healthcare Enterprise
230 East Ohio St., Suite 500
Chicago, IL 60611
Email: ihe@himss.org
Introduction
This document, the IHE Patient Care Coordination Technical Framework (PCC TF), defines specific implementations of established standards. These are intended to achieve integration goals that promote appropriate exchange of medical information to coordinate the optimal patient care among care providers in different care settings. It is expanded annually, after a period of public review, and maintained regularly through the identification and correction of errata. The latest version of the document is always available via the Internet at http://www.ihe.net/Technical_Framework/index.cfm , where the technical framework volumes specific to the various healthcare domains addressed by IHE may be found.
The IHE Patient Care Coordination Technical Framework identifies a subset of the functional components of the healthcare enterprises and health information networks, called IHE actors, and specifies their interactions in terms of a set of coordinated, standards-based transactions.
The other domains within the IHE initiative also produce Technical Frameworks within their respective areas that together form the IHE Technical Framework. Currently, the following IHE Technical Framework(s) are available:
- IHE IT Infrastructure Technical Framework
- IHE Cardiology Technical Framework
- IHE Laboratory Technical framework
- IHE Radiology Technical Framework
- IHE Patient Care Coordination Technical Framework
Where applicable, references are made to other technical frameworks. For the conventions on referencing other frameworks, see the preface of this volume.
Relationship to Standards
The IHE Technical Framework identifies functional components of a distributed healthcare environment (referred to as IHE actors), solely from the point of view of their interactions in the healthcare enterprise. At its current level of development, it defines a coordinated set of transactions based on standards (such as HL7, IETF, ASTM, DICOM, ISO, OASIS, etc.) in order to accomplish a particular use case. As the scope of the IHE initiative expands, transactions based on other standards may be included as required.
Each transaction may have as its payload one or more forms of content, as well as specific metadata describing that content within the transaction. The specification of the payload and metadata about it are the components of a Content Integration Profile. The payload is specified in a Content Module, and the impacts of any particular payload on a transaction are described within a content binding. The payloads of each transaction are also based on standards (such as HL7, IETF, ASTM, DICOM, ISO, OASIS, etc.), again, in order to meet the needs of a specific use case.
In some cases, IHE recommends selection of specific options supported by these standards. However, IHE does not introduce technical choices that contradict conformance to these standards. If errors in or extensions to existing standards are identified, IHE's policy is to report them to the appropriate standards bodies for resolution within their conformance and standards evolution strategy.
IHE is therefore an implementation framework, not a standard. Conformance claims for products must still be made in direct reference to specific standards. In addition, vendors who have implemented IHE integration capabilities in their products may publish IHE Integration Statements to communicate their products' capabilities. Vendors publishing IHE Integration Statements accept full responsibility for their content. By comparing the IHE Integration Statements from different products, a user familiar with the IHE concepts of actors and integration profiles can determine the level of integration between them. See PCC TF-1: Appendix C for the format of IHE Integration Statements.
Relationship to Product Implementations
The IHE actors and transactions described in the IHE Technical Framework are abstractions of the real-world healthcare information system environment. While some of the transactions are traditionally performed by specific product categories (e.g. HIS, Clinical Data Repository, Electronic Health record systems, Radiology Information Systems, Clinical Information Systems or Cardiology Information Systems), the IHE Technical Framework intentionally avoids associating functions or actors with such product categories. For each actor, the IHE Technical Framework defines only those functions associated with integrating information systems. The IHE definition of an actor should therefore not be taken as the complete definition of any product that might implement it, nor should the framework itself be taken to comprehensively describe the architecture of a healthcare information system.
The reason for defining actors and transactions is to provide a basis for defining the interactions among functional components of the healthcare information system environment. In situations where a single physical product implements multiple functions, only the interfaces between the product and external functions in the environment are considered to be significant by the IHE initiative. Therefore, the IHE initiative takes no position as to the relative merits of an integrated environment based on a single, all-encompassing information system versus one based on multiple systems that together achieve the same end.
Relation of this Volume to the Technical Framework
The IHE Technical Framework is based on actors that interact through transactions using some form of content.
Actors are information systems or components of information systems that produce, manage, or act on information associated with operational activities in the enterprise.
Transactions are interactions between actors that transfer the required information through standards-based messages.
The implementation of the transactions described in this PCC TF-2 support the specification of Integration Profiles defined in PCC TF-1. The role and implementation of these transactions require the understanding of the Integration profile they support.
There is often a very clear distinction between the transactions in a messaging framework used to package and transmit information, and the information content actually transmitted in those messages. This is especially true when the messaging framework begins to move towards mainstream computing infrastructures being adopted by the healthcare industry.
In these cases, the same transactions may be used to support a wide variety of use cases in healthcare, and so more and more the content and use of the message also needs to be profiled, sometimes separately from the transaction itself. Towards this end IHE has developed the concept of a Content Integration Profile.
Content Integration Profiles specify how the payload of a transaction fits into a specific use of that transaction. A content integration profile has three main parts. The first part describes the use case. The second part is binding to a specific IHE transaction, which describes how the content affects the transaction. The third part is a Content Module, which describes the payload of the transaction. A content module is specified so as to be independent of the transaction in which it appears.
Content Modules
The Patient Care Coordination Technical Framework organizes content modules categorically by the base standard. At present, the PCC Technical Framework uses only one base standard, CDA Release 2.0, but this is expected to change over time. Underneath each standard, the content modules are organized using a very coarse hierarchy inherent to the standard. So for CDA Release 2.0 the modules are organized by document, section, entry, and header elements.
Each content module can be viewed as the definition of a "class" in software design terms, and has associated with it a name. Like "class" definitions in software design, a content module is a "contract", and the PCC Technical Framework defines that contract in terms of constraints that must be obeyed by instances of that content module. Each content module has a name, also known as its template identifier. The template identifiers are used to identify the contract agreed to by the content module. The PCC Technical Committee is responsible for assigning the template identifiers to each content module.
Like classes, content modules may inherit features of other content modules of the same type (Document, Section or Entry) by defining the parent content module that they inherit from. They may not inherit features from a different type. Although information in the CDA Header is in a different location that information in a CDA Entry, these two content modules are considered to be of the same type, and so may inherit from each other when necessary.
The PCC Technical Framework uses the convention that a content module cannot have more than one parent (although it may have several ancestors). This is similar to the constraint in the Java™ programming language, where classes can derive from only one parent. This convention is not due to any specific technical limitation of the technical framework, but does make it easier for software developers to implement content modules.
Each content module has a list of data elements that are required (R), required if known (R2), and optional (O). The presentation of this information varies with the type of content module, and is described in more detail below. Additional data elements may be provided by the sender that are not defined by a specific content module, but the receiver is not required to interpret them.
Required data elements must always be sent. Data elements that are required may under exceptional circumstances have an unknown value (e.g., the name of an unconscious patient). In these cases the sending application is required to indicate the reason that the data is not available.
Data elements that are marked required if known (R2) must be sent when the sending application has that data available. The sending application must be able to demonstrate that it can send all required if known elements, unless it does not in fact gather that data. When the information is not available, the sending application may indicate the reason that the data is not available.
Data elements that are marked optional (O) may be sent at the choice of the sending application. Since a content module may include data elements not specified by the profile, some might ask why these are specified in a content module. The reason for specifying the optional data elements is to ensure that both sender and receiver use the appropriate semantic interpretation of these elements. Thus, an optional element need not be sent, but when it is sent, the content module defines the meaning of that data element, and a receiver can always be assured of what that data element represents when it is present. Senders should not send an optional data element with an unknown value. If the value is not known, simply do not send the data element.
Other data elements may be included in an instance of a content module over what is defined by the PCC Technical Framework. Receivers are not required to process these elements, and if they do not understand them, must ignore them. Thus, it is not an error to include more than is asked for, but it is an error to reject a content module because it contains more than is defined by the framework. This allows value to be added to the content modules delivered in this framework, through extensions to it that are not defined or profiled by IHE. It further allows content modules to be defined later by IHE that are refinements or improvements over previous content modules.
For example, there is a Referral Summary content module defined in this framework. In later years an ED Referral content module can be created that inherits the constraints of the Referral Summary content module, with a few more use case specific constraints added. Systems that do not understand the ED Referral content module but do understand the Referral Summary content module will be able to interoperate with systems that send instances of documents that conform to the ED Referral content module. This interoperability, albeit at a reduced level of functionality, is by virtue of the fact that ED Referrals are simply a refinement of the Referral Summary.
In order to retain this capability, there are a few rules about how the PCC Technical Committee creates constraints. Constraints that apply to any content module will always apply to any content modules that inherit from it. Thus, the "contracts" are always valid down the inheritance hierarchy. Secondly, data elements of a content module will rarely be deprecated. This will usually occur only in the cases where they have been deprecated by the base standard. While any specific content module has a limited scope and set of use cases, deprecating the data element prevents any future content module from taking advantage of what has already been defined when a particular data element has been deprecated simply because it was not necessary in the original use case.
Document Content Module Constraints
Each document content module will define the appropriate codes used to classify the document, and will also describe the specific data elements that are included. The code used to classify it is specified using an external vocabulary, typically LOINC in the case of CDA Release 2.0 documents. The set of data elements that make up the document are defined, including the whether these data elements must, should or may be included in the document. Each data element is typically a section within the document, but may also describe information that is contained elsewhere within of the document (e.g., in the header). Each data element is mapped into a content module via a template identifier, and the document content module will further indicate whether these are data elements are required, required if known or optional.
Thus, a document content module shall contain as constraints:
- The template identifier of the parent content module when there is one.
- The LOINC code or codes that shall be used to classify the document.
- A possibly empty set of required, required if known, and optional section content modules, and their template identifiers.
- A possibly empty set of required, required if known, and optional header content modules, and their template identifiers.
- Other constraints as necessary.
The template identifier for the document will be provided in the narrative, as will the legal LOINC document type codes and if present, any parent template identifier.
The remaining constraints are presented in two tables. The first table identifies the relevant data elements as determined during the technical analysis, and maps these data elements to one or more standards. The second table actually provides the constraints, wherein each data element identified in the first table is repeated, along with whether it is required, required if known, or optional. Following this column is a reference to the specification for the content module that encodes that data element, and the template identifier assigned to it. The simple example below completes the content specification described above. A simplified example is shown below.
| == Development Only ==
The PCC Wiki Content is used only for development of IHE PCC Content. The Normative content of the PCC Technical Framework and the current supplements can be found at http://www.ihe.net/Technical_Framework/index.cfm#PCC
|
| Data Element Name | Opt | Template ID |
|---|---|---|
| Sample Section Comment on section |
R | SampleSectionOID |
| Sample Entry Comment on entry |
R2 | SampleEntryOID |
Conformance
CDA Release 2.0 documents that conform to the requirements of this content module shall indicate their conformance by the inclusion of the appropriate <templateId> elements in the header of the document. This is shown in the sample document below.
<ClinicalDocument xmlns='urn:hl7-org:v3'> <typeId extension="POCD_HD000040" root="2.16.840.1.113883.1.3"/> <templateId root='SampleDocumentOID'/> <id root=' ' extension=' '/> <code code=' ' displayName=' ' codeSystem='2.16.840.1.113883.6.1' codeSystemName='LOINC'/> <title>Sample Document</title> <effectiveTime value='20260410012005'/> <confidentialityCode code='N' displayName='Normal' codeSystem='2.16.840.1.113883.5.25' codeSystemName='Confidentiality' /> <languageCode code='en-US'/> : <component><structuredBody> <component> <section> <templateId root='SampleSectionOID'/> <!-- Required Sample Section Section content --> </section> </component> |
Schematron
<pattern name='Template_SampleDocumentOID'>
<rule context='*[cda:templateId/@root="SampleDocumentOID"]'>
<!-- Verify that the template id is used on the appropriate type of object -->
<assert test='../cda:ClinicalDocument'>
Error: The Sample Document can only be used on Clinical Documents.
</assert>
<!-- Verify the document type code -->
<assert test='cda:code[@code = "{{{LOINC}}}"]'>
Error: The document type code of a Sample Document must be {{{LOINC}}}
</assert>
<assert test='cda:code[@codeSystem = "2.16.840.1.113883.6.1"]'>
Error: The document type code must come from the LOINC code
system (2.16.840.1.113883.6.1).
</assert>
<assert test='.//cda:templateId[@root = "SampleSectionOID"]'>
<!-- Verify that all required data elements are present -->
Error: The Sample Document Document must contain a(n) Sample Section Section.
See http://wiki.ihe.net/index.php?title=SampleDocumentOID
</assert>
<assert test='.//cda:templateId[@root = "SampleEntryOID"]'>
<!-- Alert on any missing required if known elements -->
Warning: The Sample Document Document should contain a(n) Sample Entry Entry.
See http://wiki.ihe.net/index.php?title=SampleDocumentOID
</assert>
</rule>
</pattern>
}}
Section Content Module Constraints
Section content modules will define the content of a section of a clinical document. Sections will usually contain narrative text, and so this definition will often describe the information present in the narrative, although sections may be wholly comprised of subsections.
Sections may contain various subsections, and these may be required, required if known or optional. Sections may also contain various entries, and again, these may be required, required if known, or optional. A section may not contain just entries; it must have at least some narrative text or subsections to be considered to be valid content.
Again, sections can inherit features from other section content modules. Once again, sections are classified using an external vocabulary (again typically this would be LOINC), and so the list of possible section codes is also specified. Sections that inherit from other sections will not specify a LOINC code unless it is to restrict the type of section to smaller set of LOINC codes specified by one of its ancestors.
Thus, a section content module will contain as constraints:
- The template identifier of the parent content module when there is one.
- The LOINC code or codes that shall be used to classify the section.
- A possibly empty set of required, required if known, and optional section content modules, and their template identifiers for the subsections of this section.
- A possibly empty set of required, required if known, and optional entry content modules, and their template identifiers.
- Other constraints as necessary.
These constraints are presented in this document using a table for each section content module, as shown below.
| == Development Only ==
The PCC Wiki Content is used only for development of IHE PCC Content. The Normative content of the PCC Technical Framework and the current supplements can be found at https://www.ihe.net/resources/technical_frameworks/#pcc
| ||||||||||||||||||||||||||||
| Template ID | SampleSectionOID | |
|---|---|---|
| Parent Template | foo (SampleParentOID) | |
| General Description | Desription of this section | |
| LOINC Codes | Opt | Description |
| XXXXX-X | R | SECTION NAME |
| Entries | Opt | Description |
| OID | R | Sample Entry |
| Subsections | Opt | Description |
| OID | R | Sample Subsection |
Parent Template
The parent of this template is foo.
<component> <section> |
Uses
See Templates using the Sample Section
Entry and Header Content Modules Constraints
Entry and Header content modules are the lowest level of content for which content modules are defined. These content modules are associated with classes from the HL7 Reference Information Model (RIM). These "RIM" content modules will constrain a single RIM class. Entry content modules typically constrain an "Act" class or one of its subtypes, while header content modules will normally constrain "Participation", "Role" or "Entity" classes, but may also constrain an "Act" class.
Entry and Header content modules will describe the required, required if known, and optional XML elements and attributes that are present in the CDA Release 2.0 instance. Header and Entry content modules may also be built up using other Header and Entry content modules.
An entry or header content module may also specify constraints on the vocabularies used for codes found in the entry, or data types for the values found in the entry.
Thus, an entry or header content module will contain as constraints:
- The template identifier of the parent content module when there is one.
- A description of the XML elements and attributes used in the entry, along with explanations of their meaning.
- An indication of those XML elements or attributes that are required, required if known, or optional.
- Vocabulary domains to use when coding the entry.
- Data types used to specify the value of the entry.
- Other constraints as necessary.
An example is shown below:
| ==== Sample Entry ====
Some text describing the entry. <observation classCode='OBS' moodCode='EVN'> <templateId root='foo'/> </observation> <observation classCode='OBS' moodCode='EVN'>Some details about the observation element <templateId root='foo'/>Some details about the template id element |
IHE Transactions
This section defines each IHE transaction in detail, specifying the standards used, and the information transferred.
IHE Patient Care Coordination Bindings
This section describes how the payload used in a transaction of an IHE profile is related to and/or constrains the data elements sent or received in those transactions. This section is where any specific dependencies between the content and transaction are defined.
A content integration profile can define multiple bindings. Each binding should identify the transactions and content to which it applies.
The source for all required and optional attributes have been defined in the bindings below. Three tables describe the three main XDS object types: XDSDocumentEntry, XDSSubmissionSet, and XDSFolder. XDSSubmissionSet and XDSDocumentEntry are required. Use of XDSFolder is optional. These concepts are universal to XDS, XDR and XDM.
The columns of the following tables are:
- <XXX> attribute – name of an XDS attribute, followed by any discussion of the binding detail.
- Optional? - Indicates the required status of the XDS attribute, and is one of R, R2, or O (optional). This column is filled with the values specified in the XDS Profile as a convenience.
- Source Type – Will contain one of the following values:
| Source Type | Description |
| SA | Source document Attribute – value is copied directly from source document. The Source/Value column identifies where in the source document this attribute comes from. Specify the location in XPath when possible. |
| SAT | Source document Attribute with Transformation – value is copied from source document and transformed. The Source/Value column identifies where in the source document this attribute comes from. Specify the location in XPath when possible. Extended Discussion column must not be empty and the transform must be defined in the extended discussion |
| FM | Fixed (constant) by Mapping - for all source documents. Source/Value column contains the value to be used in all documents. |
| FAD | Fixed by Affinity Domain – value configured into Affinity Domain, all documents will use this value. |
| CAD | Coded in Affinity Domain – a list of acceptable codes are to be configured into Affinity Domain. The value for this attribute shall be taken from this list. |
| CADT | Coded in Affinity Domain with Transform - a list of acceptable codes are to be configured into Affinity Domain. The value for this attribute shall be taken from this list. |
| n/a | Not Applicable – may be used with an optionality R2 or O attribute to indicate it is not to be used. |
| DS | Document Source – value comes from the Document Source actor. Use Source/Value column or Extended Discussion to give details. |
| O | Other – Extended Discussion must be 'yes' and details given in an Extended Discussion. |
- Source/Value – This column indicates the source or the value used.
The following tables are intended to be summaries of the mapping and transforms. The accompanying sections labeled 'Extended Discussion' are to contain the details as necessary.
Medical Document Binding to XDS, XDM and XDR
This binding defines a transformation that generates metadata for the XDSDocumentEntry element of appropriate transactions from the XDS, XDM and XDR profiles given a medical document and information from other sources. The medical document refers to the document being stored in a repository that will be referenced in the registry. The other sources of information include the configuration of the Document Source actor, the Affinity Domain, the site or facility, local agreements, other documents in the registry/repository, and this Content Profile.
In many cases, the CDA document is created for the purposes of sharing within an affinity domain. In these cases the context of the CDA and the context of the affinity domain are the same, in which case the following mappings shall apply.
In other cases, the CDA document may have been created for internal use, and are subsequentyly being shared. In these cases the context of the CDA document would not neccessarily coincide with that of the affinity domain, and the mappings below would not necessarily apply.
Please note the specifics given in the table below.
XDSDocumentEntry Metadata
| XDSDocumentEntry Attribute | Optional? | Source Type | Source/ Value |
|---|---|---|---|
| availabilityStatus | R | DS | |
| authorInstitution | R2 | SAT |
$inst <=
/ClinicalDocument/author |
| authorPerson | R2 | SAT |
$person <= /ClinicalDocument/author
|
| authorRole | R2 | SAT | This metadata element should be based on a mapping of the participation function defined in the CDA document to the set of author roles configured for the affinity domain. If the context of the CDA coincides with that of the affinity domain, then the following x-path may be appropriate: /ClincicalDocument/author/ participationFunction |
| authorSpecialty | R2 | SAT | This metadata element should be based on a mapping of the code associated with the assignedAuthor to detailed defined classification system for healthcare providers such configured in the affinitity domain. Possible classifications include those found in SNOMED-CT, or the HIPAA Healthcare Provider Taxonomy. If the context of the CDA coincides with that of the affinity domain, then the following x-path may be appropriate: /ClinicalDocument/author/ assignedAuthor/code |
| classCode | R | CADT | Derived from a mapping of /ClinicalDocument/code/@code to an Affinity Domain specified coded value to use and coding system. Affinity Domains are encouraged to use the appropriate value for Type of Service, based on the LOINC Type of Service (see Page 53 of the LOINC User's Manual). Must be consistent with /ClinicalDocument/code/@code |
| classCodeDisplayName | R | CADT | DisplayName of the classCode derived. Derived from a mapping of /ClinicalDocument/code/@code to the appropriate Display Name based on the Type of Service. Must be Consitent with /ClinicalDocument/code/@code |
| confidentialityCode | R | CADT | Derived from a mapping of /ClinicalDocument/confidentialityCode/@code to an Affinity Domain specified coded value and coding system. When using the BPPC profile, the confidentialyCode may also be obtained from the <authorization> element.
|
| comments | O | DS | |
| creationTime | R | SAT | /ClinicalDocument/effectiveTime
|
| entryUUID | R | DS | |
| eventCodeList | O | CADT | These values express a collection of keywords that may be relevant to the consumer of the documents in the registry. They may come from anywhere in the CDA document, according to its purpose. |
| eventCodeDisplayNameList | R (if event Code is valued) |
CADT | These are the display names for the collection of keywords described above. |
| formatCode | R | FM | The format code for each PCC Document content profile is provided within the document specifications. |
| healthcareFacilityTypeCode | R | CAD | A fixed value assigned to the Document Source and configured form a set of Affinity Domain defined values. Must be concistent with /clinicalDocument/code |
| healthcareFacility TypeCodeDisplay Name |
R | CAD | Must be concistent with /clinicalDocument/code |
| intendedRecipient (for XDR, XDM) | O | SAT |
$person <=
/ClinicalDocument/intendedRecipient
"^^^^^&", |
| languageCode | R | SA | /ClinicalDocument/languageCode |
| legalAuthenticator | O | SAT | $person <= /ClinicalDocument/ legalAuthenticator
|
| mimeType | R | FM | text/xml |
| parentDocumentRelationship | R (when applicable) |
DS | Local document versions need not always be published, and so no exact mapping can be determined from the content of the CDA document. The parentDocumentRelationship may be determined in some configurations from the relatedDocument element present in the CDA dsocument. If the context of the CDA coincides with that of the affinity domain, then the following x-path may be appropriate: /ClinicalDocument/relatedDocument/@typeCode |
| parentDocumentId | R (when parent Document Relationship is present) |
DS | Local document versions need not always be published, and so no exact mapping can be determined from the content of the CDA document. The parentDocumentId may be determined in some configurations from the relatedDocument element present in the CDA dsocument. If the context of the CDA coincides with that of the affinity domain, then the following x-path may be appropriate: $docID <= /ClinicalDocument/ relatedDocument/parentDocument/id
|
| patientId | R | DS | The XDS Affinity Domain patient ID can be mapped from the patientRole/id element using transactions from the ITI PIX or PDQ profiles. See sourcePatientId below. If the context of the CDA coincides with that of the affinity domain, then the following x-path may be appropriate:
|
| practiceSettingCode | R | CAD | This elements should be based on a coarse classification system for the class of specialty practice. Recommend the use of the classification system for Practice Setting, such as that described by the Subject Matter Domain in LOINC. |
| practiceSettingCodeDisplayName | R | CAD | This element shall contain the display names associated with the codes described above. |
| serviceStartTime | R2 | SAT | /ClinicalDocument/documentationOf/ serviceEvent/effectiveTime/low/ @value
|
| serviceStopTime | R2 | SAT | /ClinicalDocument/documentationOf/ serviceEvent/effectiveTime/high/ @value
|
| sourcePatientId | R | SAT | $patID <= /ClinicalDocument/recordTarget/ patientRole/id
|
| sourcePatientInfo | R | SAT | /ClinicalDocument/recordTarget/ patientRole
|
| title | O | SA | /ClinicalDocument/title |
| typeCode | R | CADT | /ClinicalDocument/code/@code
|
| typeCodeDisplay Name |
R | CADT | /ClinicalDocument/code/@displayName |
| uniqueId | R | SAT | $docID <= /ClinicalDocument/id
|
XDSSubmissionSet Metadata
The submission set metadata is as defined for XDS, and is not necessarily affected by the content of the clinical document. Metadata values in an XDSSubmissionSet with names identical to those in the XDSDocumentEntry may be inherited from XDSDocumentEntry metadata, but this is left to affinity domain policy and/or application configuration.
Use of XDS Submission Set
This content format uses the XDS Submission Set to create a package of information to send from one provider to another. All documents referenced by the Medical Summary in this Package must be in the submission set.
Use of XDS Folders
No specific requirements identified.
Configuration
IHE Content Profiles using this binding require that Content Creators and Content Consumers be configurable with institution and other specific attributes or parameters. Implementers should be aware of these requirements to make such attributes easily configurable. There shall be a mechanism for the publishing and distribution of style sheets used to view clinical documents.
Extensions from other Domains
Scanned Documents (XDS-SD)
XDS-SD is a CDA R2 document and thus conforms to the XDS Metadata requirements in the PCC-TF, volume 2, Section 5 unless otherwise specified below.
XDSDocumentEntry
XDS-SD leverages the XDS DocumentEntry Metadata requirements in the PCC-TF, volume 2, Section 5.1.1.1.1 and in PCC_TF-2/Bindings unless otherwise specified below
XDSDocumentEntry.formatCode
The XDSDocumentEntry.formatCode shall be urn:ihe:iti:xds-sd:pdf:2008 when the document is scanned pdf and urn:ihe:iti:xds-sd:text:2008 when the document is scanned text. The formatCode codeSystem shall be 1.3.6.1.4.1.19376.1.2.3.
XDSDocumentEntry.uniqueId
This value shall be the ClinicalDocument/id in the HL7 CDA R2 header. The root attribute is required, and the extension attribute is optional. In accordance with the XDS.a profile, total length is limited to 128 characters; for XDS.b the limit is 256 characters. Additionally see PCC-TF, volume 2, Section 5.1.1.1.1 or PCC_TF-2/Bindings for further content specification.
Relating instances of XDS-SD documents
In general, most instances of XDS-SD will not have parent documents. It is possible, however, in some specific use cases that instances of XDS-SD documents are related. For example, for a particular document it may be the case that both the PDF scanned content and somewhat equivalent plaintext need to be wrapped and submitted. Each document would correspond to separate XDSDocumentEntries linked via an XFRM Association that indicates one document is a transform of the other. These can be submitted in a single submission set, or in separate ones. Other specific examples may exist and this profile does not preclude the notion of a parent document for these cases.
XDSSubmissionSet
No additional constraints. Particular to this profile, a legitimate use of submission sets would be to maintain a logical grouping of multiple XDS-SD documents. We encourage such usage. For more information, see PCC-TF-2 Section 5.1.1.1.2 or PCC_TF-2/Bindings.
XDSFolder
No additional requirements. For more information, see PCC-TF-2 Section 5.1.1.1.3 or PCC_TF-2/Bindings.
Basic Patient Privacy Consents (BPPC)
Laboratory Reports (XD-LAB)
XD-Lab is a CDA R2 document and thus conforms to the XDS Metadata requirements in the PCC-TF, volume 2, Section 5 unless otherwise specified below.
XDSDocumentEntry
XD-Lab leverages the XDS DocumentEntry Metadata requirements in the PCC-TF, volume 2, Section 5.1.1.1.1 and in PCC_TF-2/Bindings unless otherwise specified below
XDSDocumentEntry.eventCodeList
XD-Lab documents further constrain the the XDSDocumentEntry.eventCodeList to the following.
| Attribute | Optional? | Source Type | Source/ Value |
|---|---|---|---|
| eventCodeList | R2 | SAT | ClinicalDocument / component / structuredBody / component / section / entry / act / entryRelationship / organizer (templateId="1.3.6.1.4.1.19376.1.3.1.1")/ component / observation(templateId="1.3.6.1.4.1.19376.1.3.1.1.1")/code
AND ClinicalDocument / component / structuredBody / component / section / entry / act / subject / code If the document has Reportable Condition, then this code shall be among those listed in the eventCodeList. Additionally, if the document contains information about a Non-Human Subject, then the code that indicates what this subject is shall be among those listed in the eventCodeList. Thus, this attribute has been enhanced from the XDS profile from O to R2. |
XDSDocumentEntry.formatCode
The XDSDocumentEntry.formatCode shall be urn:ihe:lab:xd-lab:2008 The formatCode codeSystem shall be 1.3.6.1.4.1.19376.1.2.3.
XDSSubmissionSet
No additional constraints. For more information, see PCC-TF-2 Section 5.1.1.1.2 or PCC_TF-2/Bindings.
XDSFolder
No additional requirements. For more information, see PCC-TF-2 Section 5.1.1.1.3 or PCC_TF-2/Bindings.
Namespaces and Vocabularies
This section lists the namespaces and identifiers defined or referenced by the IHE PCC Technical Framework, and the vocabularies defined or referenced herein.
The following vocabularies are referenced in this document. An extensive list of registered vocabularies can be found at http://www.hl7.org/oid/.
| codeSystem | codeSystemName | Description |
| 1.3.6.1.4.1.19376.1.5.3.1 | IHE PCC Template Identifiers | This is the root OID for all IHE PCC Templates. A list of PCC templates can be found below in CDA Release 2.0 Content Modules. |
| 1.3.6.1.4.1.19376.1.5.3.2 | IHEActCode | See IHEActCode Vocabulary below |
| 1.3.6.1.4.1.19376.1.5.3.3 | IHE PCC RoleCode | See IHERoleCode Vocabulary below |
| 1.3.6.1.4.1.19376.1.5.3.4 | Namespace OID used for IHE Extensions to CDA Release 2.0 | |
| 2.16.840.1.113883.10.20.1 | CCD Root OID | Root OID used for by ASTM/HL7 Continuity of Care Document |
| 2.16.840.1.113883.5.112 | RouteOfAdministration | See the HL7 RouteOfAdministration Vocabulary |
| 2.16.840.1.113883.5.1063 | SeverityObservation | See the HL7 SeverityObservation Vocabulary |
| 2.16.840.1.113883.5.7 | ActPriority | See the HL7 ActPriority Vocabulary |
| 2.16.840.1.113883.6.1 | LOINC | Logical Observation Identifier Names and Codes |
| 2.16.840.1.113883.6.96 | SNOMED-CT | SNOMED Controlled Terminology |
| 2.16.840.1.113883.6.103 | ICD-9CM (diagnosis codes) | International Classification of Diseases, Clinical Modifiers, Version 9 |
| 2.16.840.1.113883.6.104 | ICD-9CM (procedure codes) | International Classification of Diseases, Clinical Modifiers, Version 9 |
| 2.16.840.1.113883.6.26 | MEDCIN | A classification system from MEDICOMP Systems. |
| 2.16.840.1.113883.6.88 | RxNorm | RxNorm |
| 2.16.840.1.113883.6.63 | FDDC | First DataBank Drug Codes |
| 2.16.840.1.113883.6.12 | C4 | Current Procedure Terminology 4 (CPT-4) codes. |
| 2.16.840.1.113883.6.257 | Minimum Data Set for Long Term Care | The root OID for Minimum Data Set Answer Lists |
| 1.2.840.10008.2.16.4 | DCM | DICOM Controlled Terminology; PS 3.16 Content Mapping Resource, Annex D |
| 2.16.840.1.113883.6.24 | MDC | ISO/IEEE 11073 Medical Device Nomenclature |
| 2.16.840.1.113883.3.26.1.5 | NDF-RT | National Drug File Reference Terminology (NCI version) |
| 2.16.840.1.113883.11.19465 | nuccProviderCodes | National Uniform Codes Council Healthcare Provider Terminology |
| 2.16.840.1.113883.6.255.1336 | X12DE1336 | Insurance Type Code (ASC X12 Data Element 1336) |
| 2.16.840.1.113883.6.256 | RadLex | RadLex (Radiological Society of North America) |
| 1.3.6.1.4.1.19376.1.5.3.1.3.43 | PCC.ODH | Vocabulary OID used in ODH IG |
The IHE FormatCode vocabulary is now managed in an Implementation Guide published using FHIR.
- formal canonical URI https://profiles.ihe.net/fhir/ihe.formatcode.fhir/ValueSet-formatcode.html
- formal publication URL https://profiles.ihe.net/fhir/ihe.formatcode.fhir/
- FormatCode gitHub repository for source of the Implementation Guide can be used to register issues, or create pull requests for modifications. Formal governance is managed by ITI Technical Committee.
This FormatCode vocabulary represents:
- Code System 1.3.6.1.4.1.19376.1.2.3
- Value Set 1.3.6.1.4.1.19376.1.2.7.1
IHEActCode Vocabulary
| CCD | ASTM/HL7 Continuity of Care Document | |
| CCR | ASTM CCR Implementation Guide |
The IHEActCode vocabulary is a small vocabulary of clinical acts that are not presently supported by the HL7 ActCode vocabulary. The root namespace (OID) for this vocabulary is 1.3.6.1.4.1.19376.1.5.3.2. These vocabulary terms are based on the vocabulary and concepts used in the CCR and CCD standards listed above.
| Code | Description |
| COMMENT | This is the act of commenting on another act. |
| PINSTRUCT | This is the act of providing instructions to a patient regarding the use of medication. |
| FINSTRUCT | This is the act of providing instructions to the supplier regarding the fulfillment of the medication order. |
| IMMUNIZ | The act of immunization of a patient using a particular substance or class of substances identified using a specified vocabulary. Use of this vocabulary term requires the use of either the SUBSTANCE or SUBSTCLASS qualifier described below, along with an identified substance or class of substances. |
| DRUG | The act of treating a patient with a particular substance or class of substances identified using a specified vocabulary. Use of this vocabulary term requires the use of either the SUBSTANCE or SUBSTCLASS qualifier described below, along with an identified substance or class of substances. |
| INTOL | An observation that a patient is somehow intollerant of (e.g., allergic to) a particular substance or class of substances using a specified vocabulary. Use of this vocabulary term requires the use of either the SUBSTANCE or SUBSTCLASS qualifier described below, along with an identified substance or class of substances. |
| SUBSTANCE | A qualifier that identifies the substance used to treat a patient in an immunization or drug treatment act. The substance is expected to be identified using a vocabulary such as RxNORM, SNOMED CT or other similar vocabulary and should be specific enough to identify the ingredients of the substance used. |
| SUBSTCLASS | A qualifier that identifies the class of substance used to treat a patient in an immunization or drug treatment act. The class of substances is expected to be identified using a vocabulary such as NDF-RT, SNOMED CT or other similar vocabulary, and should be broad enough to classify substances by mechanism of action (e.g., Beta Blocker), intended effect (Dieuretic, antibiotic) or ... |
| For Public Comment | What else needs to appear above for SUBSTCLASS? |
IHERoleCode Vocabulary
The IHERoleCode vocabulary is a small vocabulary of role codes that are not presently supported by the HL7 Role Code vocabulary. The root namespace (OID) for this vocabulary is 1.3.6.1.4.1.19376.1.5.3.3.
| Code | Description |
| EMPLOYER | The employer of a person. |
| SCHOOL | The school in which a person is enrolled. |
| AFFILIATED | An organization with which a person is affiliated (e.g., a volunteer organization). |
| PHARMACY | The pharmacy a person uses. |
Conventions
Folder Content Modules
CDA Release 2.0 Content Modules
This section contains content modules based upon the HL7 CDA Release 2.0 Standard, and related standards and/or implementation guides.
