Clinical Research, Public Health and Quality use of EHR Data
Scope
In this paper, we are looking for several things. First, for each of our stakeholders, we would like them to describe each of their problem stakeholders, and the tasks and workflows that are executed under the current state of affairs.
Secondly, we will review both the similaries and differences between stakeholders, tasks and workflows from each of the three communititees. This will help define the scope of the problems that we want to solve.
Lastly, we will put forth a proposed plan of work, not just for the PCC domain, but also to other domains, including IT Infrastructure, Laboratory, and the newly formed Quality domain.
Clinical Trials
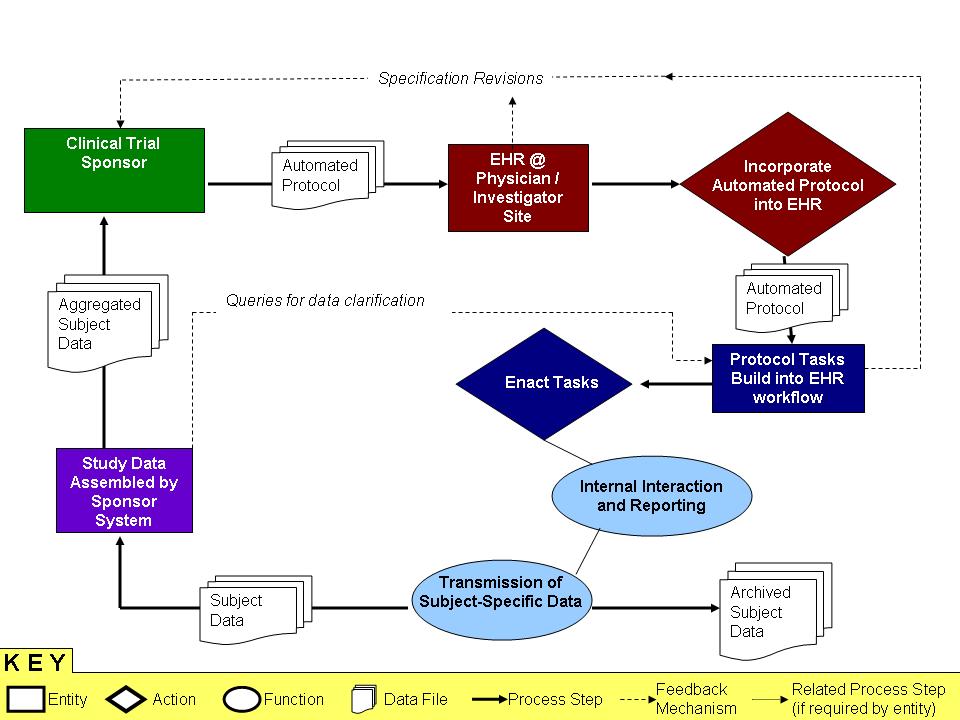
The initial interest of the CDISC community -- the biopharmaceutical companies who sponsor clinical trials -- was to insert a research protocol into an EHR as an executable piece of workflow. While this bears semblance to other 'case management' use cases, the phrase will not make sense to the clinical trial community.
The embedded image (also included as a Powerpoint link) shows how protocol insertion might work.
Media:Media-ProcessDiagramClinicalTrial_CaseMgt_14Mar07_lb.ppt
Public Health Reporting
Introduction
Definition of Public Health (functions and services)
Organization of Public Health (local, state and federal)
Relevance to IHE (scope of activities)
Community Health considerations in a RHIO – vision statement
Stakeholders:
Safety-net clinics
Healthcare providers (private)
Local Health Department
State Health Department
Other Governmental Agencies (e.g. DOE/CDC/HHS)
Other healthcare providers (e.g. hospitals, labs, RX, Nursing home, home health)
Medicaid/Social Services case workers
Disease Management Departments
Case Managers (may be within any of the above)
Emergency responders
Use Case
Example use cases
HEDIS
HEDIS for reporting purposes only
HEDIS for clinical practice guidelines
HEDIS as annual measure – interim case management/outreach - proactive
Case Management – what individual does to manage the disease
Chronic Diseases Management (Asthma , Diabetes , COPD, Heart, obesity)
Disease Management – a aggregate analysis of care delivery for a disease entity
Chronic Diseases Management (Asthma , Diabetes , COPD, Heart, obesity)
Decision Support
1. Community Record
Bioterrorism Preparedness/surveillance
Direct Care providers
1. Case Management
2. Scheduled public care
3. Health Education
Environmental health (abatement, asbestos)
Preventive care services
1. Maternal and Child Health
a. Prenatal (nutrition, WIC, genetic testing), Newborn (e.g. pku, a1c), hearing, immunization, birth defects, vital registration, lead screening, school, vision, developmental assessment (mental, physical), nutrition (Early Periodic Screening Diagnostic Tests EPSDT)
2. Physicians A1C's law to order testing on annual physicals (EGFR), not required to report results – Public Act to perform mandatory testing as part of the physical. Educational component may be needed.
3. School Health
a. Healthy Child (communicable disease reporting, lead, TB, chronic care Asthma/Diabetic, immunization)
b. Sick
i. Walkins
ii. Medication administration
iii. Participation/non-participation in physical activities
iv. Assistive devices (e.g. insulin pump, wheelchair)
v. Special education (developmental disabilities)
c. Security/Privacy
i. Parent consent to share sensitive data
ii. Minimum data set
iii. Consent
iv. Audit
v. Access Control (DOE vs DPH employed nurses)
vi. FERPA
vii. COPPA
d. Surveillance
i. Absentee
ii. Vitals on walkin (e.g. fever, viral infections, rashes, diahrea, injuries, obesity)
Scenario
Today – paper based
after electronic environment
Workflow for school health scenario (take from the document)
Parent requests form vs Provider fills in health form (after system – if the child is age 5, generate form)
Provider signs health form
Actor/transaction
Disease management system – used to handle disease on individual and aggregate basis; system needs to interface to both aggregate and clinical care data
For Aggregate Investigations
Investigation Resource
Community Record
HEDIS for reporting purposes only
HEDIS for clinical practice guidelines
HEDIS as annual measure – interim case management/outreach - proactive
Analyzer
for school health scenario
Parent provides RHIO consent for release restrictions to school system (BPPC)
Parent provides RHIO consent for release of school health record to system
Provider/EHR generates School Health Form including DSG
Provider EMR submits school health form to RHIO (DOE?) (Provide and Register)
School nurse retrieves health form from RHIO into local school EMR (document Consumer)
School nurse EMR generates walkin visit medical summary (XDS-MS)
EMR sends medical summary to RHIO (Provide and Register)
(School attendance system generates school attendance data)
Local public health retrieves Medical data from RHIO school and medical system submissions (document consumer) (?Aggregate Data Retrieval)
Local public health analyses data for trend analysis
Condition detected through trending (e.g. flu) Case investigation
Intervention
Communication with parent
In-school services to mitigate illness (e.g. vaccination)
In-school Education (opportunity?)
Data Dictionary
Element
Definition
Standard vocabulary
Issues
Recommendations
Take forms from 50 states (e.g. school health forms) for the selected domain
HEDIS – A1C – Cross-work with Quality Domain
collect Disease Registry for Diabetes
A1C
Case Management forms for Diabetes
Quality Reporting
Definition of Quality (Safe, Effective, Efficient, Patient-Centered, Timely and Equitable)
Five key areas in which information technology could contribute to an improved health care delivery system:<ref>Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century. 2001. p 31.</ref>
Access to the medical knowledge-base
Computer-aided decision support systems
Collection and sharing of clinical information
Reduction in errors
Enhanced patient and clinician communication
As summary, the Quality Domain includes aggregate measures of performance as well as individual case reporting of adverse events (including but not limited to Hospital Acquired Infections <HAIs>, adverse drug events <ADEs>, sentinel events, and others).
Quality Vision as defined by AHIC (see Appendix A)
National Quality Enterprise
Stakeholders
Consumers
Providers (Hospitals, ambulatory practices, pharmacies, labs, radiology clinics)
Clinical Practitioners (Physicians / Physician Practices /Ambulatory Practices, Laboratorian, radiologist, case managers, pharmacists, etc)
Employers
Policymakers
Accreditors
Research Community
Vendor of healthcare information systems
Performance Measure Development Organizations
Performance Measure Endorsers/ Approvers
Performance Measure Adopter (Payors, etc)
Clearinghouse/ Outsourced Measure Calculator/ Benchmarking Service
Performance Measure Implementers/ Receivers
Defining Characteristics of the Healthcare System with Respect to the Quality Enterprise
Receiving Care (includes consumer education/decision support)
Delivering Encounter-based Care (includes practitioner education/decision support)
Managing Health of Defined Populations (Cohort)
Coordination of Care (for 1 person across care venues)
Improving Quality
Measuring and Reporting Quality
Reimbursement (e.g. pay-for-performance)
Accreditation
Certification
Defining Characteristics of the National Quality Infrastructure
Metrics
EHR Products
EHR Adoption
Data Stewardship
Data Aggregation
Population Reporting and Feedback
Public Reporting
Health Information Exchange and Intermediaries
Privacy and Security, Secondary Uses of Data
Medical Education
Knowledge products
Enablers and Barriers
Enablers
- Clear value proposition supports the use of HIT capabilities for quality assessment, quality improvement and informed decision making
- Collaboration between providers, purchasers, consumers and accreditors/oversight bodies and professional certification entities produce uniform standards for sharing and aggregating health data and for public reporting
- Collaboration between regional quality measurement initiatives and RHIOs or NHIN service providers
- Standard approach for EHRs to routinely produce quality data based on approved measures that span care delivery
- Designation of a national health data stewardship entity to oversee appropriate use of data
- Comprehensive medical record across points of care obtained via health information exchange networks to enable intelligent alerts to providers
- Measure developers identify data and HIT requirements in order to implement measures into clinical care and software
- Certification of HIT based on criteria to enable reporting of an expanded set of AQA and HQA quality measurement in EHRs
- Education of consumers on how to obtain data and assess quality of care along with sharing of data with patients' PHRs will increase consumer stake in quality measurement
- Overall payment system that provides incentives for quality and safe care
- Cultural change that encourages performance reporting
- Certification of clinical decision support capabilities in EHRs
- Additional pilot projects that provide leadership for a national framework and act as learning laboratories to link public and private data sets and assess clinical quality, cost of care and patient experience
- Personal Health Records
Barriers
- Lack of a clear business model for health information exchange
- Lack of a clear business model for quality
- Limited set of national consensus measures; robust measures not yet developed for all physician specialties
- Lack of standards for data collection and aggregation
- Lack of standardized mechanisms for external reporting including data stewardship
- Lack of alignment of payment with quality performance
- Gaps in regulations and practices relating to privacy/security and secondary use of data
- Slow translation of research into practice at the point of care
- Quality assessment tightly linked with site of care or individual clinicians; few integrated or episode-based metrics
- Lack of coordination in quality measurement
- Gaps in quality management capabilities of EHRs
- Clinical documentation unstructured using non-standardized nomenclature
- HIE operational in few regions
- Poor provider economics- higher costs of doing business, declining reimbursement and the expectation of implementing information technology solutions
- Lack of a complete medical record to support CDS (Clinical Decision Support)
- Reluctance to share data
- PHR adoption
- EHR adoption
Organization of Quality (local, state and federal)[May be adequately defined in the components above]
Today
manual extract from or chart review EHR
often doesn't happen
claims reporting (e.g. PQRI (physician quality reporting initiative))
credentialing and accrediting organizations (responsible for selecting measures).
There are multiple concurrent credentialing and accrediting activities for the same practitioners. (e.g. Payor accreditation, state licensing requirements for physician groups include quality measures that could be conflicting or have multiple reporting requirements)
Measured developing organizations work with these bodies to create the measures
Proposed Workflow
Indicates goes to vendor short-term
longer-term – EHR incorporates directly
(insert diagram)
Quality Reporting Consumer
[May be informed by or replaced by the content in the Stakeholder section from the AHIC table as indicated above.]
Payers/ Insurers,
Regulators and policy makers (e.g. state agencies, federal regulators, etc)
Credentialing and accrediting organizations (responsible for selecting measures)
Measured developing organizations work with these bodied to create the measures (e.g. 3M that sells sw to manage performance measures, demanders of healthcare measures-payers, facilities that want to benchmark themselves regarding quality of care.
Provider Organization
Decision support
This section encompasses internal decision support capabilities for concurrent (or interactive) decision support which may be managed through multiple means, e.g., order sets, protocols, care plans, aggregated alerts and reminders, individual alerts and reminders. Management of concurrent decision support should be enabled by quality measurement and reporting elements defined externally or locally. Methodologies for attaining successful quality outcomes require careful attention to local practice and workflow and therefore such methodologies should not be proscriptive.
Continuous Quality Improvement (CQI)
This section refers to capability to compare dynamically, in near real-time, and retrospectively, performance with respect to structural, process and outcome measures of quality, whether defined and transmitted from an external stakeholder or identified locally. Methodologies for attaining quality outcomes require alignment with local workflow and practice and therefore such methodologies should not be proscriptive. The site for aggregation of data for such CQI practices can be inherent within the EHR or external to the EHR either at the practice location or managed by a third party data warehouse organization or vendor. Such data management tactics must be determined by the healthcare organization, yet enabled by the input and export for the quality domain.
External reporting of quality measures for
accountability
pay for performance
contractual
Policy issues impacting Quality measures
Medical home
Concern for specialty or primary care provided by multiple practitioners – who is accountable
Provider responsibility assignment, vs payor assignment may differ
Referred providers and practitioners (e.g. specialty providers, radiology center)
Attribution
to individual practitioner
to process
to practice/clinic/hospital
health plan
provider networks
e.g comorbidity/mortality post-surgical; score by MD, need to risk adjust, and consider process factors may not be accounted for in the physician scorecard; quality measure/reporting should be mindful of reporting and measures at appropriate levels
Quality of measures
Inconsistency of measures
cohort definition
attribution
metric
Measure standards
different insurers requiring different measure and care delivery criteria
similar process measures used for attribution to different care providers
Types of quality measures
Structural
EMR certified for decision support
Using EMR for e-prescribing
Outcome
return to work
functional status improvement
Process
procedure done
lab order
test result improvement
Relevance to target audience
Quality considerations in a RHIO – vision statement
Electronic Data Capture from EMR
Within as part of workflow
From outside of the usual clinical workflow
Query
Publish and Subscribe
Payload Content
Message
source data
summary data
Document
source data
summary data
Filter Data
Numerator
Those in the cohort that receive the care/process expected
Describes case definition for the population in question
Denominator
The cohort (case definition)
Exclusions from cohort
Beware of too much complexity req up front
Exclusions
Numerator
1.1.1.1.1.1 Retrospective removal from denominator
1.1.1.1.1.2 E.g. patient compliance
1.1.1.1.1.3 Patient leaves practice (death, move, change doctors)
Denominator
1.1.1.1.1.4 E.g. allergy to medication class
1.1.1.1.1.5 Failure of therapy trial
1.1.1.1.1.6 Contra-indicated conditions
Where in the workflow do you trigger the rule (inserting step in provider's workflow)
Variable in each implementation
Avoid too much prescription – want to show that it gets done
Could be through order
External to EHR (after the fact)
Vision – improve patient care – could be within EHR during visit, but early on will likely be post-visit
Prospective reporting/analysis before it affects the measure
Relevance to IHE (scope of activities)
PCC or Component Constructs
Payload Content
Message
Document
EMR Query
Performance Measurement Rule (XML, BPL, Gello?)
ITI
Publish/Subscribe
Query
Quality
Framework
Measures
Use Case
Example use cases
Adverse Event Reporting (Sentinel)
Hospital acquired infection
patient falls (unplanned descent to the floor
PQRI specifies 'with injury'
ANA Nursing does not specify 'with injury'
Measures
A1C
Antiplatelet Therapy (CAD-1): Percentage of patients with CAD who were prescribed antiplatelet therapy
Workflow for quality measurement
Insert Powerpoint flow diagram
Insert Aggregate data diagram from IHE ITI document
Include Swim Lane Diagram
Actor
Measure Rule Information Resource (Investigation Resource ) (some database of the encoded rules that may be pushed to or polled by the provider system
Payor
Accreditor
Licensor
Certifier
Provider Systems (CIS) (Information/document source) (Hospitals, ambulatory practices, pharmacies, labs, radiology clinics)
EMR
EHR
Disease Management System
Quality Management System
Risk Management System
Research Community
Measure definition
Providers
System-consumers
Analyzer
Clearinghouse/ Outsourced Measure Calculator/ Benchmarking Service Information System (receives raw from Provider System CIS)
Receivers (receives raw or aggregate data from Provider System CIS)
Performance Measure Implementers
System-Consumer/client decision system (Report Card system)
Person/individual
employer
regulator
Policy makers
licensing board
certification board
Public Health System
Payors
Accrediting Bodies (e.g. Joint Commission)
transaction
Glossary
HEDIS
HEDIS for reporting purposes only
HEDIS for clinical practice guidelines
HEDIS as annual measure – interim case management/outreach - proactive
Case Management – what individual does to manage the disease
Chronic Diseases Management (Asthma , Diabetes , COPD, Heart, obesity)
Disease Management – a aggregate analysis of care delivery for a disease entity
Chronic Diseases Management (Asthma , Diabetes , COPD, Heart, obesity)
Decision Support
Community Record
Direct Care providers
Case Management
schedule public care
Preventive care services
Physicians A1C's law to order testing on annual physicals (EGFR),.
Security/Privacy
Minimum data set
Consent(Authorization)
Audit
Access Control
Scenario
Today – paper based
after electronic environment
Data Dictionary
Element
Definition
Standard vocabulary
Issues
Market Need
Use Case
Similarities and Differences
Standards Used
Opportunities and Challenges
Patient Care Coordination
IT Infrastructure
Quality
Glossary of Terms
- Public Health
- (derive definition from Anna Orlova's presentation)