Antepartum Summary Form C
Introduction
This is a draft of the Antepartum Summary Profile (ACS) supplement to the Patient Care Coordination Technical Framework. This draft is a work in progress, not the official supplement or profile.
Profile Abstract
The Antepartum Summary Profile (ACS) one-paragraphs-desc
Glossary
- Term
- Definition
Issue Log
Open Issues
- Issue
- Issue
Closed Issues
Volume I
Add the following bullet to the list of profiles
- Antepartum Summary - one-line descr
Dependencies
Add the following row(s) to the list of dependencies
| Integration Profile | Dependency | Dependency Type | Purpose |
|---|---|---|---|
| Antepartum Summary |
Profile Name
The Antepartum Summary Profile (ACS) one-paragraphs-desc
Obstetrical patients in labor and admitted to Labor and Delivery must have a complete summary of their antepartum ambulatory care available at the time of admission to evaluate and / or ameliorate risk. This same data is required at any visit to Labor and Delivery for any other problems or special needs a patient may require.
As the patient is seen over a finite period in the office, aggregation of specific relevant data is important to the evaluation of the obstetrical patient upon presentation to Labor and Delivery. During the 40 weeks of a typical pregnancy duration, the patient will have had an initial History and Physical Examination, followed by repetitive office visits with multiple laboratory studies, imaging (usually ultrasound) studies, and serial physical examinations with recordings of vital signs, fundal height, and the fetal heart rate. The original New OB History & Physical, ongoing Medical Diagnoses, the Estimated Due Date, outcomes of any prior pregnancies, serial visit data on the appropriate growth of the uterus and assessments of fetal well being, authorizations, laboratory and imaging studies must all be presented and evaluated upon entry to the Labor and Delivery Suite to ensure optimal care for the patient and the fetus.
While for labor patients the planned method of delivery may be vaginal (natural), there is a substantive chance the delivery route may be surgical, requiring anesthesia and post-surgical care.
Current practice is to copy the (paper) chart at various times during the pregnancy (as at 28 weeks and at 36 weeks of completed gestation), and transport the copies of the chart to the hospital the patient intends to use for delivery. Should the patient arrive prior to the chart copy arriving, or if the chart (or information within the chart) is missing on presentation of the patient to Labor and Delivery (a frequent occurrence), often the staff or clinicians repeat laboratory or imaging studies. This results in unwarranted and duplicative tests, is wasteful of time and resources, and leads to dissatisfied patients. Further, missing or incomplete information about the patient’s clinical status may create a situation where critical information is unavailable to clinicians, which may ultimately result in an injury, inadequate aftercare or other undesirable outcome .
Significantly, a large portion of patients arrive in L&D without complete documentation. In one recent U.S. study , ~70% of patients (with paper charts) arrived in L&D without their current medical record being available. While in this study, only one hospital was involved, one can see the extent of the issue, with pregnant patients possibly going to a different hospital than planned (preterm labor, rapid labor and unable to make it to the planned delivery hospital, or visiting a distant city), moving mid-care, or with a covering physician (rather than the primary obstetrician) on call.
In a Swedish study done in the 1990’s, critical data on paper records were incomplete from 45 to 87.5% of the time. Thus, availability of current medical records remains a significant problem for most hospital Labor and Delivery units; availability of key information electronically will significantly enhance patient safety.
Use Cases
Use Case Name 1
- Pre-condition
- The patient’s obstetrician sees the patient for her pregnancy in the ambulatory (office) setting. During the pregnancy, the patient is noted to have a medical problem requiring consultation with a Maternal-Fetal Medicine specialist (perinatologist). The office obtains pre-authorization from the insurance payer for the consult, and for the intended or anticipated route of delivery, and transmits that information to both the consultant and to the hospital.
- Events
- The patient is seen in the obstetrician’s office where a complete medical and relevant social history are taken by the nurse and recorded in the office EHR, incorporating data from the perinatologist’s consultation report as appropriate. Laboratory and imaging reports ordered by the perinatologist as well as the perinatologist’s consultation report are displayed electronically to the obstetrician. The obstetrician reviews the consultation report from the perinatologist’s office and imaging studies ordered by the perinatologist along with data recorded by the nurse. Physical exam reveals some abnormalities. The obstetrician orders additional laboratory studies, and sends the patient to the hospital to Labor and Delivery.
When the laboratory results return, the physician completes the admission H&P, Allergies, Medications, includes the data prepared or ordered by the perinatologist, and makes it available to L&D. This data includes an assessment of the patient’s health status, and the requisite data summarized from the antepartum care given. The charge nurse for L&D documents that the complete collection of documents needed is available. The Post-Partum discharge planning is notified and assures that there is a suitable environment with appropriate support for post-delivery after-care.
- Post-condition
- The Pre-delivery H&P and Antepartum Summary with appropriate relationships to the Perinatologist Consultation, and all the antepartum laboratory and imaging studies are available to the obstetrician and the birthing center personnel for incorporation into their respective EHRs. The H&P is also available to the patient for viewing and incorporation into the patient’s PHR, and into the newborn baby’s PHR.
Use Case Name 2
One or more paragraphs describing a clinical scenario.
Actors/Transaction
| Actor | Transaction | Opt. | Section |
|---|---|---|---|
| Actor 1 | Transaction 1 | R | #Transaction 1 |
Options
| Actor | Option | Section |
|---|---|---|
| Actor 1 | Option 1 | #Option 1 |
Option 1
A description of option 1.
Grouping
Process Flow
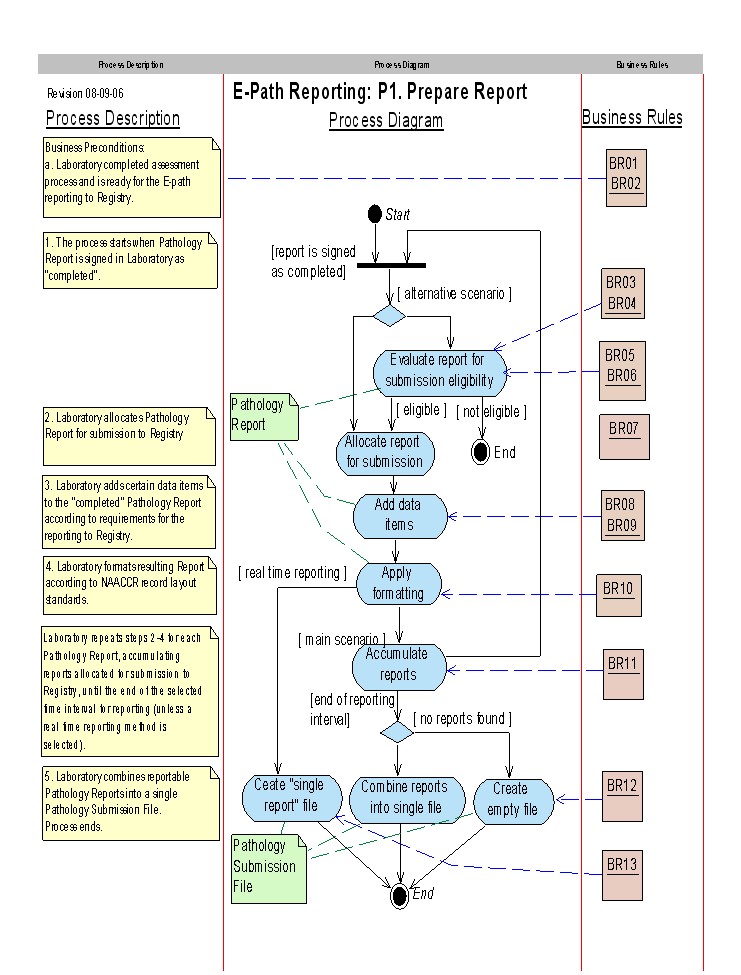
More text about process flow
Actor Definitions
- Actor
- Definition
Transaction Definitions
- Transaction
- Definition
Volume II
Transaction 1
Scope
Use Case Roles
[[image:ucr.jpr|frame|center]
- Actor
- Actor 1
- Role
- Role of Actor 1
lather, rise and repeat for each actor
Referenced Standards
- STD
- Description