Bed Management: Difference between revisions
JohnMoehrke (talk | contribs) |
|||
| (30 intermediate revisions by one other user not shown) | |||
| Line 1: | Line 1: | ||
This profile is to manage the interoperability issues that surround the bed management tasks that are involved with admissions to the various hospital departments from the emergency department. | |||
__TOC__ | |||
=='''Summary'''== | |||
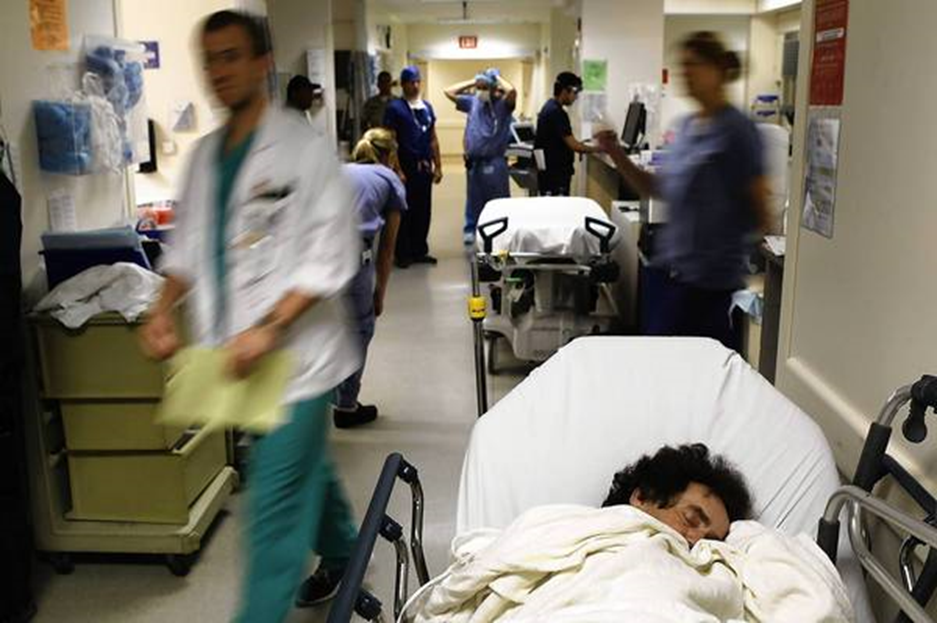
[[image: ED pic for BED.png|300px]] | |||
Bed management is the ability for a healthcare facility or system to have real-time operational awareness of the status of all of its available beds and to be able to plan for the expedient use of beds through coordination of the bed turnover process. Beds are a scarce resource, and the limitation of access to beds leads to delays and waste within healthcare systems. | |||
'''Due to a lack of interoperability in the emergency department several problems occur: | |||
*Work inefficiencies are decreased for emergency department providers and other staff with no mechanism to monitor patient status in real-time | *Work inefficiencies are decreased for emergency department providers and other staff with no mechanism to monitor patient status in real-time | ||
*Delays in patient transfers to other inpatient departments | *Delays in patient transfers to other inpatient hospital departments occur | ||
*Siloed data which results in | *Siloed data which results in: | ||
**Poor data quality for process and performance improvement activities | |||
**Inability to effectively perform care coordination | |||
==Benefits== | =='''Benefits'''== | ||
A robust, integrated bed management not only improves patient care, but also impacts a hospital's financial status. The benefits of this profile | A robust, integrated bed management process not only improves patient care, but also impacts a hospital's financial status. The benefits of this profile are: | ||
* Increased efficiency | * Increased efficiency | ||
| Line 23: | Line 30: | ||
* Improved patient transfer and care coordination data, resulting in better predictive planning | * Improved patient transfer and care coordination data, resulting in better predictive planning | ||
'' | =='''Details'''== | ||
This transport profile facilitates bed management for patients admitted from the ED. Inefficiencies in transferring patients between the emergency department and inpatient setting result in poorer patient outcomes (e.g., morbidity, mortality or length of stay), increased patient dissatisfaction and poorer resource utilization in the ED. This profile describes how communications between the ED and various inpatient systems can improve care, reduce cost and result in higher patient satisfaction, and enable tracking and monitoring of these activities to support quality improvement activities. | |||
This profile does not address how charge information is transferred from various involved systems to the back office, or how discharge or transfers from the inpatient setting to other settings are handled. | |||
==Systems Affected== | =='''Systems Affected'''== | ||
| Line 37: | Line 43: | ||
* ''Admission/Discharge/Transfer (ADT) System'' | * ''Admission/Discharge/Transfer (ADT) System'' | ||
* ''Emergency Department Information System (EDIS)'' | * ''Emergency Department Information System (EDIS)'' | ||
* '' | * ''Bed Management System (BMS)'' | ||
'' | == '''Actors & Transactions:''' == | ||
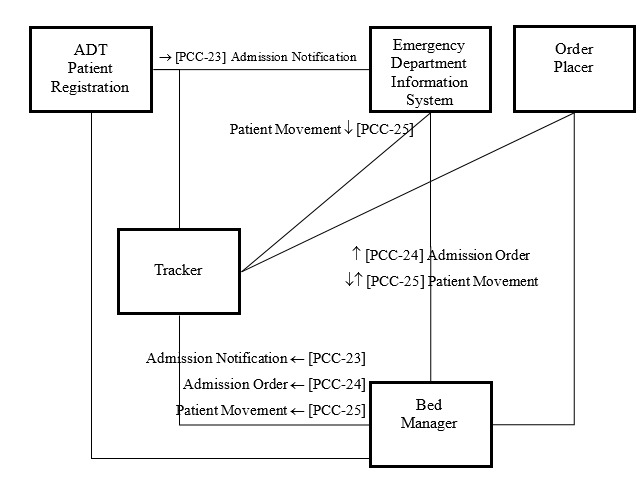
' | ''''[[Image:BED ActorTransaction Diagram.png|550px]] | ||
''' | =='''Specifications'''== | ||
'' | '''Profile Status: '''Trial Implementation'' | ||
''' | '''Documents:''' | ||
The BED Profile is designed to work alongside the IHE IT Infrastructure PAM Profile, but has differing requirements upon what actors are used and additional requirements for the messages that they send. | |||
* IHE ITI Patient Administration Management Profile [http://wiki.ihe.net/index.php/Patient_Administration_Management:] | |||
''' | '''Underlying Standards:''' | ||
:* HL7 v2.6 ADT, Patient Administration [http://www.hl7.org HL7] | |||
:* HL7 EDIS Functional Profile - Registration Release 1 (v.1.4) | |||
''' | '''Related Profiles''' | ||
'' | ''None. '' | ||
| Line 97: | Line 80: | ||
This page is based on the [[Profile Overview Template]] | This page is based on the [[Profile Overview Template]] | ||
[[Category:Profiles]][[Category:Patient Care Coordination]][[Category: | [[Category:Profiles]][[Category:Patient Care Coordination]][[Category:HL7v2]] | ||
Latest revision as of 10:14, 4 November 2019
This profile is to manage the interoperability issues that surround the bed management tasks that are involved with admissions to the various hospital departments from the emergency department.
Summary
Bed management is the ability for a healthcare facility or system to have real-time operational awareness of the status of all of its available beds and to be able to plan for the expedient use of beds through coordination of the bed turnover process. Beds are a scarce resource, and the limitation of access to beds leads to delays and waste within healthcare systems.
Due to a lack of interoperability in the emergency department several problems occur:
- Work inefficiencies are decreased for emergency department providers and other staff with no mechanism to monitor patient status in real-time
- Delays in patient transfers to other inpatient hospital departments occur
- Siloed data which results in:
- Poor data quality for process and performance improvement activities
- Inability to effectively perform care coordination
Benefits
A robust, integrated bed management process not only improves patient care, but also impacts a hospital's financial status. The benefits of this profile are:
- Increased efficiency
- Reduced delays and waste
- Improved patient transfer and care coordination data, resulting in better predictive planning
Details
This transport profile facilitates bed management for patients admitted from the ED. Inefficiencies in transferring patients between the emergency department and inpatient setting result in poorer patient outcomes (e.g., morbidity, mortality or length of stay), increased patient dissatisfaction and poorer resource utilization in the ED. This profile describes how communications between the ED and various inpatient systems can improve care, reduce cost and result in higher patient satisfaction, and enable tracking and monitoring of these activities to support quality improvement activities. This profile does not address how charge information is transferred from various involved systems to the back office, or how discharge or transfers from the inpatient setting to other settings are handled.
Systems Affected
- Electronic Health Record (EHR)
- Admission/Discharge/Transfer (ADT) System
- Emergency Department Information System (EDIS)
- Bed Management System (BMS)
Actors & Transactions:
Specifications
Profile Status: Trial Implementation
Documents:
The BED Profile is designed to work alongside the IHE IT Infrastructure PAM Profile, but has differing requirements upon what actors are used and additional requirements for the messages that they send.
- IHE ITI Patient Administration Management Profile [1]
Underlying Standards:
- HL7 v2.6 ADT, Patient Administration HL7
- HL7 EDIS Functional Profile - Registration Release 1 (v.1.4)
Related Profiles
None.
This page is based on the Profile Overview Template