PaLM F2F Minutes 2017-Nov: Difference between revisions
| Line 150: | Line 150: | ||
</ul> | </ul> | ||
=='''Minutes - Monday, November | =='''Minutes - Monday, November 13, 2017'''== | ||
| Line 407: | Line 407: | ||
<li>Goal of this profile is to document the event and not the specimen itself. Consider this as a snapshot of the specimen at the time of the event. If you need to look for ALL associated tests, may need to look in more places and not rely on SET to find all related orders on a specimen.</li> | <li>Goal of this profile is to document the event and not the specimen itself. Consider this as a snapshot of the specimen at the time of the event. If you need to look for ALL associated tests, may need to look in more places and not rely on SET to find all related orders on a specimen.</li> | ||
</ul> | </ul> | ||
=='''Minutes - Tuesday, November 14, 2017'''== | =='''Minutes - Tuesday, November 14, 2017'''== | ||
Revision as of 14:53, 20 December 2017
IHE PaLM Face to Face Meeting, November 13 - 15, 2017 Cagliari, Sardinia IT
Attendees
| Name | 13-Nov | 14-Nov | 15-Nov |
|---|---|---|---|
| Gunter Haroske | x | x | x |
| Jurgen De Decker (tc) | x | x | x |
| Jim Harrison | x | x | x |
| Raj Dash | x | x | x |
| Mary Kennedy | x | x | x |
| Carolyn Knapik | x | x | x |
| Riki Merrick | x | x | x |
| Kenichi Takahashi | x | x | x |
| François Macary | x | x | x |
| Alessandro Sulis | x | x | x |
| Francesca Frexia | x | x | x |
| Daniel Rutz | x | x | x |
| Mario Villace | x | x | x |
| Toon Claeys | x | x | x |
| Jessica Poisson (tc) | x PM | x PM | |
| Vittorio Meloni | x | x | x |
| Genichi Kato | x | x | x |
| Cecilia Mascia | x | x | x |
| Luca Lianas | x | x | x |
| Filip Migom | x | x | x |
| Megumi Kondo | x | x | x |
| Paolo Anedda | x | ||
| Alessandra Gocca | x | ||
| Andrea Costaglioli | x PM | x AM | |
| David De Mena (tc) | x | ||
| David Clunie (tc) | x AM | x | |
| Pieter De Smet (tc) | x AM | x | |
| Romaric Croes (tc) | x AM | ||
| Frank Van Apeldoorn (tc) | x | ||
| Ralf Zwoenitzer (tc) | x |
- tc indicates attendance via teleconference
Supporting Documents
- Word version of minutes
- Supporting documents See minutes for which document relate to which section
Summary and Action Items (details follow in Minutes)
- TMA
- Need for additional stakeholders from TM domain (nursing, )
- Change requests to base standard attempted for Jan. & May WGMs -> delay until ?
- Pre-adopt approved new features
- Wait for Japan’s expectations this month
- LCC
- Publish for public comment (request sent Nov15 to MJ)
- Public comment period until end January
- Process comments (2nd hour of February or March call)
- Publish TI in June
- SET
- Choose the standard
- Check standard’s coverage (using the 2nd hour of the monthly calls in December and January)
- Request for changes -> delay for approval
- Write Vol 2
- APSR 2.0
- Migrate media wiki content to pubswiki.ihe.net ( tbd KH)
- Publish for TI -> target date January 25
- Digital Pathology
- White paper scheduled
- Skeleton + initial content shared on GoogleGroup Nov 25.
- December 13 call -> assignment chapters/contributors + draft the monthly call calendar for S1 2018
- First draft for January for sharing within PaLM committee and with DICOM WG 26.
- Re-check alignment of specimen representation
- DICOM supplement 122 / HL7 Specimen DAM / IHE PaLM
- Start producing the first set of profiles (image acquisition, image retrieval & display, ordering/reporting, …)
- Join DICOM WG 26 in Helsinki around June 1st to work on the profiles
- 1st profiles for public comment after November meeting?
- LSH
- Waiting confirmation of interest from Roche Diagnostic
- Reactivate and invite other stakeholders to participate.
- PaLM TF Maintenance
- Write the CP (Filip + Riki + François)
- Potentially one or two additional CPs
- CP balloting
- Integration into TF
- Publish release 9.0 in June.
Minutes - Monday, November 13, 2017
Synopsis of PaLM assets and ongoing projects discussed during the meeting:
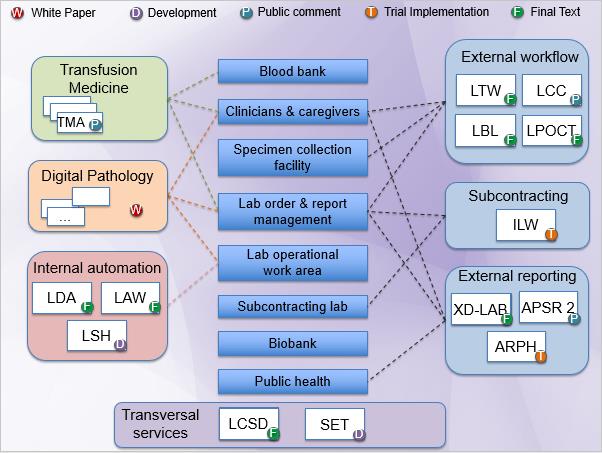
Summary of milestones set by the meeting:
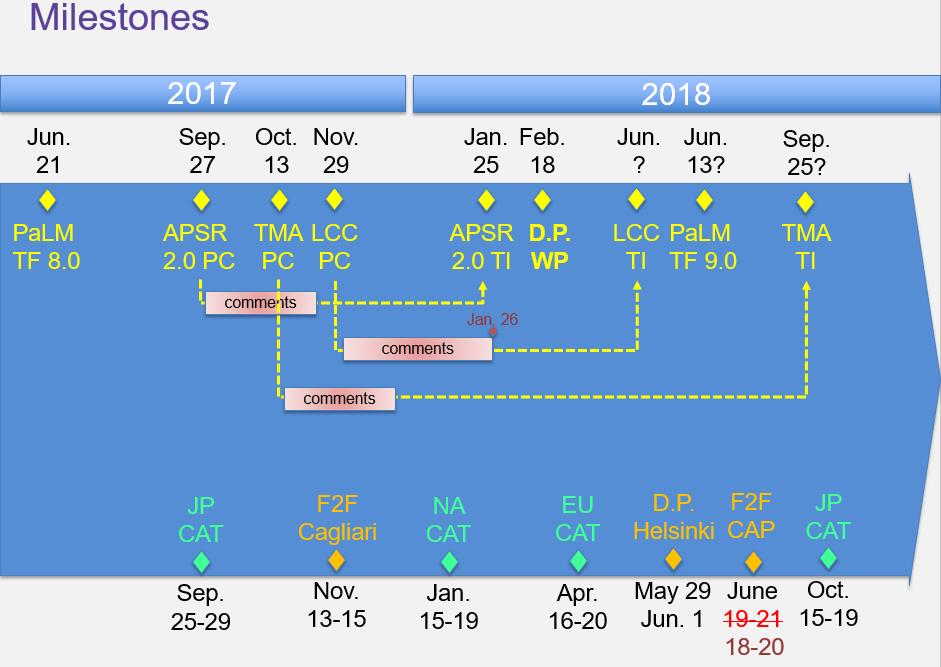
Thank you to CRS4 for hosting the meeting!
Introductions were given around the table and teleconference for attendees.
(See PaLM_meeting_Cagliari2017_FM_v2.pptx)
Agenda was reviewed with no changes: https://docs.google.com/spreadsheets/d/1Tl6oyF0BxPEMOQ8R3smz_eM6ZboMbZCqwC-pDjwB3x8/edit#gid=0
Other meetings of interest: possible co-meeting with DICOM. ECDP 2018 (European Congress on Digital Pathology) will take place in Helsinki, Finland, May 30th – June 1st. http://digitalpathologysociety.org/14th-european-congress-on-digital-pathology-ecdp-2018/
APSR 2.0: (see APSR 2.0 PC Remarks.pptx)
- Gunter shared pdf draft for Public Comment that was published September 2017: http://ihe.net/uploadedFiles/Documents/PaLM/IHE_PaLM_Suppl_APSR_2.0_PC_2017-09-27.pdf
- Art décor tool now used to produce the APSR profile on CDA template (free tool): https://art-decor.org/mediawiki/index.php/Main_Page
- We will need help from Kai to deal with the OID issue. The annotation comment uses the PCC OID and there is a collision with OIDs due to large volume of projects working in art décor (international patient summary, EPSOS, etc.) and no good central OID management tool at this time.
- The media wiki hosted by Germany is migrating to a new wiki to be used by IHE (pilot project).
- Reason for statusCode of not allowing active for the observation entries
- Do we reinstate the missing value set, OR
- Use the statusCode value set and constrain to final and aborted?
- Corrections are handled by full replacement of the entire report (CDA) with link to replacing document. The corrected / changed result is not clearly indicated. Consider either:
- a header indicator in replacement reports that indicates where the change is, or
- add a new section that lists all the references to the sections that are changed
- May not be possible identify the actual correction, as that is often in narrative form.
- Would be good to (at least) identify which section to focus attention on.
- Review the base CDA standard for possible solution.
- Need to consider other changes that are important for patient care (diagnosis change either minor or major error), and those not affecting patient care.
= If implementing this, we should consider the clinical impact of revision as well.
- IHE-Lab extension is in header to the status of the entire report. We will need assistance from Kai to develop a solution.
- Do we need Payer information in header?
- This was requested by cancer registry.
- Could we use this section from PCC or should we add a participant in the header indicating this is insurance?
- XD-Lab is an open document template, so we can add additional unspecified content (receiver does not need to raise an error if present, but also does not need to consume it) The header level would be the better location for this
- Do we want to allow 0..* for insurance? We would need to define what each one means, when sending more than one. This would be ONLY limited to patient member ID and Name/ID for the insurance company. (in Germany public health requests payment from insurance in order to reimburse the pathologist). We need to get a better idea of what elements we need as part of that insurance.
- Include a note in the accompanying text that intention is just for reference, not the entire insurance related information, leaving the recipient to get more research based on the IDs provided.
- Ask Kai what the difference in the tool is between “includes” or “contains” regarding author in additional observation versus in all other sections. We can then decide which way to proceed. Contains seems more compact.
- Additive: in SpecimenDAM have additive in 2 places (in container and in the processing activity). In APSR we use the processing additive. There may be a difference in the vocabulary between the container (for transport) and the processing additives for preparation of specimen.
- The circular reference is correct, since we can have recursive parent-child relationships.
- ICD-O codes: not all are publically available (but supposed to be).
- Why not use SCT? They are missing the cancer detail. iPaLM SCT could work on adding gap concepts to SCT. Gunter to bring some examples to PaLM.
- ICD-O-3 has 1:1 map to SCT. We can research newer concepts.
- M code has first 4 digits describing the morphology, the /5th digit describes the behavior part of the tumor. Can you have all behaviors for all morphologies? If not, it will be difficult to validate the codes.
- Should we allow multiple code systems (SCT and ICD-O codes) in this element?
- High level sections in APSR: would it be valuable to have molecular observations in a separate section instead of using the additional observation? Check with Clinical Genomic regarding CDA templates (Cambridge 2013)
SNOMED CT Candidate Free Subset: (See ppt: PaLM_meeting_Cagliari2017_FM_v2.pptx)
- SNOMED IHTSDO is now SNOMED International, headquartered in London
- There is an effort starting in USA by University of Nebraska’s Scott Campbell (chair of iPALM at SNOMED International) with a deliverable focused 3 year plan to create SCT codes for all CAP cancer protocols.
- Harmonized with Australia, Sweden, UK, and Canadian rules.
- We will need to check with Netherlands (European organization for SCT harmonization) as to their status with this effort.
- Working on genomic concepts related to cancer with clinically actionable components. Breast, colon, and melanoma are completed.
- SCT codes will be listed in University of Nebraska’s extension in UMLS and will be available.
- LOINCs are generated for SCT observables created for these cancer protocols. Discussions are ongoing about migrating LOINC into SNOMED International.
- Francois introduced APSR to the SNOMED International work and they will use it as basis to attach the vocabulary binding for the cancer work.
- CAP direction for incorporating SCT: the vocabulary will be added into the work. Scott will have to deconstruct some of the SDC eCC representation. This might adjust the data model to be of a more clinical data focus as additional material to the eCC work.
- Since SNOMED International requires country based membership (or per individual implementation) – annual fees based on GDP of each country – more info: https://www.snomed.org/about. It cannot be a required vocabulary
- How many concepts to add for synoptic cancer reporting? For variance reporting would be under 100, but several 100/protocol. TMN is not part of it due to an AJCC licensing issue. Prognostic staging is excluded (includes biomarkers and other indicators), but should be able to include limited TNM staging declaration.
- Next step will be in January, so if there are more requests for free SCT codes, add now and send to Co-Chairs.
- Here is the list for review: https://docs.google.com/spreadsheets/d/13zfwPYsetLIOwOFqe59TVLVMVA1-_vlIxN9k7-dpOyg/edit#gid=0
IHE PaLM updates around the world:
- Japan: (see ppt: PaLM-IHE-Japan.pptx)
- Change in Lab Co-chair: Yoshimi Hirasawa is replaced by Naomi Ishii.
- IHE Connectathon had about 160 participants. Summary results will be posted soon on the internet.
- LTW-MB = national extension for microbiology used in Japan
- US:
- LAW to CLSI AUTO-16 conversion: the plan is to publish for proposed draft vote for 60 days at the beginning of 2018. This will replace the old ASTM standards used for instrument connections: CLSI is ISO TC 212 supported.
- Connectathon will be held January 15-19, 2018 in Cleveland, Ohio. LTW and XD-Lab, maybe LPOCT (single vendor) and LAW (if Orchard joins) will be tested.
- LOI / LRI update: both are in ballot reconciliation. Added profiles include clinical genomics to LRI and newborn screening for LOI and LRI. Publication is expected sometime in January or February 2018.
- Europe:
- Belgium:
- LTW has experienced some implementation.
- CDA reporting using XD-Lab to forward lab results to the physician. They will use a messaging wrapper for exchange.
- France:
- larger hospitals are implementing LTW
- Use of XD-Lab is mandated from laboratories
- Not sure a lot of folks have implemented for microbiology
- IHE-Europe Connectathon in the HAGUE, 16-20 April 2018.
- New HL7 project to represent micro for handoff from hospital to nursing homes (care transition between acute care and long term care). There are new PSS CCDA infectious disease additions.
- Belgium:
LCC Update to review for publication for comment
- A pathologist can place an order for HER2 testing, it can be added to the system, and refinement on the exact block that the order should be made on can occur at a later point in time. LCC could potentially be used for that, as long as the system can handle the incomplete order. In current systems the pathologist in the laboratory does that adjustment. GAO profile (clinical decision support profile) does something similar? Example skin sample placed order for GU test – currently need to cancel the test and add in a manual order that needs to be authorized later.
- The LCC already makes note that all use cases are lab based, because of our expertise.
- Pharmacy may have to look at how the RDX segment may need to be changed to match the added field in OBR segment in the OML and (in radiology) OMG messages.
- Will circulate to google group and then will send for publishing on Wednesday, so all comments should be submitted by COB Tuesday to the group.
TMA:
- No comments received on the document (comment period closed yesterday).
- First in series of Transfusion Medicine profiles: Adverse event reporting – prior to that have the dispensing workflow and then the ordering of the units (some issues exist with linking crossmatching to encounters or patient MRNs etc.)
- HL7 v2 specification does not currently handle the detail about the adverse reaction, so we will need to propose a new v2 message to get that covered. It is planned to work with HL7 Patient Care group, who is designing FHIR handling and data modeling (allergy reaction)
- Adverse outcome on patient side could be relevant, but is not part of the current documentation (due to terminology being based on US centric reporting requirements (who is reporting to whom).
- Reviewing the profile: http://ihe.net/uploadedFiles/Documents/PaLM/IHE_PaLM_Suppl_TMA_Rev1.0_PC_2017-10-13.pdf
- Open issues:
- New codes for the HL70513 Blood Transfusion Disposition status (at the unit level) will need a harmonization proposal for the next cycle Mar 2018.
- Need to additionally include status that describes when administration was interrupted – with or without a reaction. Suggest to pull the existing equivalence from the treatment completion status (HL70322), which has less useful codes (Complete, refused, not administered, partially administered). (Ask Margaret about nutrition administration status codes).
- Do we need to document a rate change for blood transfusion like you do for IVs?
- Clotting factor – is that medication or blood product? (Ask Jessica)
- Finland has national blood management system and red cross system for adverse reactions (may need independent reaction consumer).
- France is building national infrastructure for adverse event reporting which supports keeping that actor separate. Our focus is suspected reaction, not a verified reaction that is reported to the authorities for investigation (this is prior to the blood bank having to report to authorities). Consider adding the report from the blood product filler to the adverse event consumer.
- The instructions are to stop the transfusion at any time there is suspected reaction and call the bloodbank, so it indeed is a different “beast”. Is there terminology around this? Probability is assessed/ determined by the blood bank (possible, probable, confirmed, what other?). Would it be useful to capture the assessment from the blood bank to the transfusion documenter?
- Is the report from the transfusion documenter suspected initially and then confirmed from blood product filler? The assessment is in the blood bank system that will be reported back to the EHR (currently as a narrative pathology report) and if appropriate, also to the PH authorities.
- Highlighting specific antibodies is currently non–standard script. Some systems may need this.
- When the blood product is contaminated it needs to be sent to the supplier of the blood product. This bleeds into the inventory workflow. We have ruled OOS, but we may need to refine. This occurs more commonly with platelets.
- Will need reaction consumer as stand-alone actor.
- 2 phases of LAB-76
- One for suspected reaction from documenter to filler. This filler is actually an order to evaluate the observations sent.
- One for evaluation of reaction from filler to documenter (and possibly to public health). This may be a distinct translation, because it is a logically a different step in the workflow with different semantics.
- Is the blood product filler, not the blood transfusion documenter that reports to the adverse event consumer? The endpoints are different systems, but is the role the same?
- If there is no reaction, the transfusion is continued, or repeated – so no report is sent.
- Dan will try to adjust the diagram for us to review
- LAB-76 is expected to carry the observations about the relevant vitals for the suspected reaction messages. This may not be needed for confirmed reactions but should be possible to send.
- In Belgium there is requirement to document the vitals (RR, pulse and temp) for patients with transfusions every 15 minutes. Should the vitals be sent ONLY in the documenting message, or should they be included in the transfusion status message? Vitals at the start of transfusion are the baseline vitals. Vitals in the transfusion status message are not a continuous feed.
- Vital attached to suspected reaction message are useful; it would be useful to include the baseline vitals as well as ALL vitals up to the moment in time that the reaction occurs. It may be better to only include the vitals from the start of transfusion/pre-transfusion and those at the time the reaction occurs.
- We may need to review the OBX-29/OBX-30 value sets to cover other reaction types as well as noting which ones are vitals.
- The described scope is fine with the following exception: The line about whole blood transfusion not being needed should be changed so that whole blood is added as another available blood product.
- Need more description on the workflow. Consider for the next round of review.
- Currently reporting to FDA is ONLY for fatalities due to blood transfusion via phone or email.
- Open issues:
SET: (seePaLM_SET_F2F_Cagliari.pptx)
- Container definition may be:
- A single tube when the specimen is collected;
- A shipping box that holds multiple containers (so we can track the box a specimen is shipped in);
- Specimen can be spread across multiple containers, which is why we use specimen ID pus container ID (i.e. 24 hour urine collected in multiple containers).
- Does the label on the tube contain the specimenID as well as the container ID? In many cases, systems will assign the container ID based on the specimenID, and may add further IDs to the specimen, such as -01, or -A, but it is not mandated.
- Need to clarify whether the specimenID refers to the parent specimen ONLY or to ANY specimen, including a derived specimen. In the specimen DAM we consider each derived specimen, including aliquots, as specimens.
- Wil have to look at LBL profile use of specimen ID and container ID.
- Matrix open issues (red font items)
- Do we need to include associated ordered tests in SET? That would be only for specimen container prepared and specimen collection events.
- We must be able to represent the timestamp of the event.
- We need to define these timestamps:
- Effective time of the event (for example the collection date/time, the processing date/time, the transport date/time)
- Event documentation time (Entered into system)
- Message created / sent
- FHIR resource includes the reference to the procedureRequest.
- Drop the placer group number and the associated test list (should be in the order workflow). We may need to list the dependency on another profile to query for the order information based on the placer order number. This would be limited to the time of the event.
- Goal of this profile is to document the event and not the specimen itself. Consider this as a snapshot of the specimen at the time of the event. If you need to look for ALL associated tests, may need to look in more places and not rely on SET to find all related orders on a specimen.