Digital Pathology Aid for Telemedicine
1. Proposed Workitem: Digital Pathology Aid for Telemedicine
- Proposal Editor: Francesca Vanzo, Gregorio Canal
- Editor: Mauro Zanardini, Francesca Vanzo, Gregorio Canal, Gianluca Pavan
- Date: N/A (Wiki keeps history)
- Version: N/A (Wiki keeps history)
- Domain: Pathology and Laboratory in Medicine
2. The Problem
The exchange of digital pathology images is becoming increasingly in demand among different settings. Due to the high specialization required, not many anatomic pathologists are able to report any kind of biopsies (i.e. specific types of kidney biopsies) and this leads to an increased number of preventable treatment as dialysis and transplants, with a potential worsening of the patient quality of life and high costs for health organizations and public administrations. Currently the digital pathology is not deployed in all LHAs and HTs as well as the image access and sharing among them in this field. The lifecycle management of these kinds of images begins in the scanner and often ends in the local hard disk of the scanner itself or in some non standard external storage that is carried to a consultant or forwarded with legacy format or internet links. The image management should move across department or enterprise boundaries also according to a Vendor Neutral Archive approach and an accurate sharing of information and to privacy and security regulations. The newly published profile and white paper of the IHE PaLM domain and several IHE profiles come to the rescue for the digitization and to provide a framework for this scope.
The potentiality of having a guidance available to obtain a teleconsultation on the matter will allow to limit high costs for health organizations also preventing claims, and will improve patient quality of life moving toward a collaborative working environment. In fact, the creation of a pathology network would also enable the pooling of expertise and competence as well as the collaboration between different hospital trusts and local health authorities with different levels of specialization. Under an economic point of view, the offsetting between the necessary adjustments or upgrades costs and benefits will be reached and overtaken by the teleconsulting financial compensation. The actual systems are very rarely integrated to share and allow the reconciliation of patient data in this context. The main areas to be addressed are: the generation and acceptance of the request, the creation of the Image Study by digitizing the microscope slide (Specimen UID, Kos for pathology and other features according to DICOM Supplements 122 and 145), the storage, the sharing and the display of the imaging content, the reporting (signed structured report where possible), the availability of the report for the requester also in a EHR perspective, the optional dialogue system between physicians and the administrative closing of the procedure.
These aspects require a set of agreements according to well developed guidelines provided by several IHE profiles and DICOM specifications, and must be contextualized on the anatomic pathology for the not completely covered steps. This part needs to be further developed or easily and in practice explicated.
3. Key Use Case
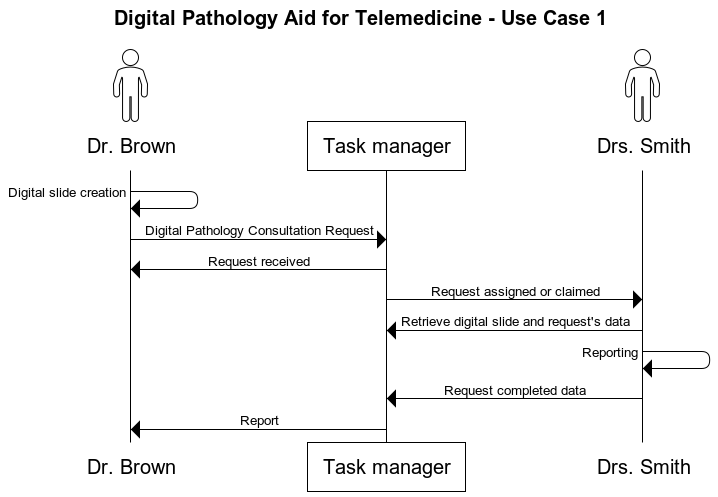
Use Case 1 Dr. Brown, a Goodcare Hospital’s anatomic pathologist, during the execution of an examination notices something that needs to be further investigated on a kidney biopsy slide. He decides to ask Drs. Smith, a Sacred Heart Hospital’s kidney specialist pathologist, for a consultation. Therefore using his workstation, Dr. Brown sends a consultation request which is assigned to Drs. Smith. Drs. Smith agrees to the request, retrieves the related images and starts the reporting. The report results are shared with Dr. Brown, who can decide which is the best therapy or other actions for the patient.
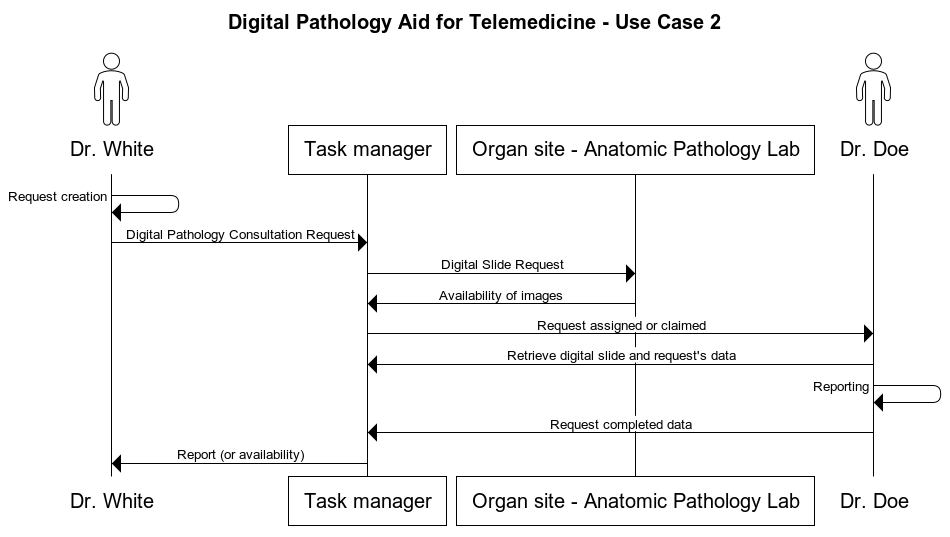
Use Case 2 Dr. White is in charge of a transplant unit at the Memorial Hospital and is made aware of the availability of a liver in another site which has not been previously analyzed and there is no anatomic pathologist on call in that hospital unit. The suitability of the organ is affected by the medical history of the donor, elapsed time and an anatomic pathology examination must be performed. Dr. White sends an urgent consultation request with his workstation, to the available anatomic pathologist. Dr. Doe claims the request, retrieves the related images and starts the reporting with his workstation. The report results are shared with Dr. White, who provides the information to the doctor in charge for the transplant decisions.
4. Standards and Systems
Existing systems that are/could be involved in the problem/solution:
- Anatomic Pathology LIS - Order Filler
- PACS
- VNA
- Order Placer
- Document Repository
- Document Registry
- Patient Identification Management
Standards which might be relevant to the solution:
Standards:
- DICOM (in general and specifically Supplement 122, Supplement 145)
- HL7
IHE Profiles:
- XDS (Cross-Enterprise Document Sharing)
- XDS-I.b (Cross-Enterprise Document Sharing for Imaging)
- XRR-WD (Cross-Enterprise Remote Reporting for Imaging)
- DSUB (Document Metadata Subscription)
- DPIA (Digital Pathology Image Acquisition)
- ATNA (Audit Trail and Node Authentication)
- XUA (Cross-enterprise User Assertion)
- PDQ (Patient Demographic Query)
- PIX (Patient Identifier Cross-referencing)
- XDW (Cross-Enterprise Document Workflow)
Other components:
- Digital Slide Scanners
- BPPC (Basic Patient Privacy Consents)
- APPC (Advanced Patient Privacy Consents)
- Patient Demographic Source
5. Discussion
<Include additional discussion or consider a few details which might be useful for the detailed proposal> :<Why IHE would be a good venue to solve the problem and what you think IHE should do to solve it.>
As the countries move forward with their guidelines to face COVID-19, telemedicine is becoming crucial and the several guidelines and standards highlighted by IHE, represent the key to face it in a long term for a stable use over time. IHE has the tools to compose the workflow solution.
- <What might the IHE technical approach be? Existing Actors? New Transactions? Additional Profiles?>
The approach is firstly to take into consideration profiles and guidelines of IHE PaLM. In addition to this, the XRR, XDS-I.b and XDS profiles are useful for the reporting and image/document sharing as well as the Supplements from the DICOM Working group 26 (with the DICOM Pathology data model as mentioned in the IHE PaLM DPIA profile). As well as SWF (Scheduled Workflow) profile from Radiology Domain is helpful for the registration, ordering, scheduling, imaging acquisition, storage and viewing transactions (for the possibly features not covered by IHE PaLM profiles). Main existing actors: Acquisition manager, Acquisition modality, Image manager, Image archive, Image display, Imaging Document Consumer, Imaging Document Source, Document repository, Document registry, Document Consumer, Task Manager, ...
Main existing transactions (where applicable to Pathology images and data) in the cross-enterprise approach:
- [RAD-68] Provide and register Imaging Document Set MTOM/XOP
- [ITI-42] Register Document Set-b
- [ITI-18] Registry Stored Query
- [RAD-55] WADO Retrieve
- [RAD-69] Retrieve Imaging Document Set
- [RAD-16] Retrieve Images
- [RAD-17] Retrieve Presentation States
- [RAD-27] Retrieve Reports
- [RAD-31] Retrieve Key Image Note
- [RAD-45] Retrieve Evidence Documents
- [ITI-43] Retrieve Document Set
- [ITI-9] PIX Query
- <What are some of the risks or open issues to be addressed?>
The fact that most of the actors and the transactions taken into account are drawn from established IHE profiles, allows to conclude that the risks are minimized. It is in the digital pathology Image exchange where the only kind of issues may potentially lie, however the time is now ripe to take this step forward. Significant experience: DICOM Digital Pathology Connectathon organized by DICOM WG 26 during the 14th European Congress on Digital Pathology held in Helsinki (29th-1st June 2018).